Abstract
Thalidomide may be used as a treatment option for pyoderma gangrenosum (PG) and myelodysplastic syndrome (MDS). Herein, we aimed to report a patient who was treated well with thalidomide and whose diagnosis was PG with MDS. A 61-year-old man with painless ecchymotic lesions in his right upper extremity was admitted to the hospital in Isparta, Turkey, in January 2015. The lesions were diagnosed as PG. In his anamnesis, it was found that he was diagnosed with MDS 6 years ago and had been treated with cyclosporine at 2×100 mg for 5 years, which was stopped in January 2015. Aspiration from liver lesion revealed the presence of Mycobacterium tuberculosis, so antituberculosis treatment was started. Bone marrow investigation revealed MDS-refractory anemia with excess blasts (7%). For lesions in bilateral upper extremities, thalidomide treatment was started at 50 mg/d. After 1 month from the initiation of thalidomide treatment, the lesions in upper extremities had disappeared. In the literature, there are some reports of patients with PG who were successfully treated with thalidomide. Our patient is a complicated case who simultaneously has MDS, PG, and tuberculosis infection. The reason for thalidomide usage in our patient was the need of immune modulation without immune suppression. Our patient has tolerated the drug well, and excellent response was obtained after 1 month of initiation of thalidomide treatment. To conclude, thalidomide is a very effective drug acting as an immune modulator, which is useful in the clinical management of both MDS and PG.
Introduction
Pyoderma gangrenosum (PG) is an occasional neutrophilic dermatosis. Therapy could be difficult because of painful skin lesions. Incidence of the disease is ~5/1,000,000.Citation1 Inflammatory bowel diseases, hematological malignancies, or rheumatologic diseases have been diagnosed in majority of patients.Citation2–Citation4 Myelodysplastic syndromes (MDSs) may be associated with PG.Citation3–Citation5 The mechanism of PG is not yet fully understood; however, disorders of immune system seem to have an important role.Citation5 Small traumas may aggregate PG. There were different types of PG lesions.Citation6 The main pattern is a painful ulcerative lesion. The clinical course can be very aggressive depending on the underlying disease. Steroids, tacrolimus, and cyclosporine may be used in the treatment. Thalidomide may be used as a treatment option in some patients.Citation4,Citation7,Citation8 Herein, we aimed to report a patient who was diagnosed as PG with MDS and responded well to thalidomide treatment.
Case report
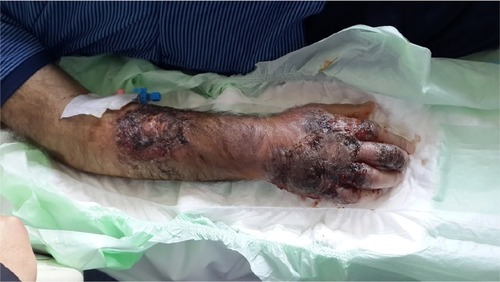
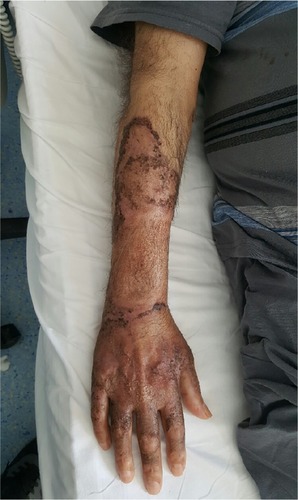
A 61-year-old man with painless ecchymotic lesions in his right upper extremity was admitted to the hospital in Isparta, Turkey, in January 2015. He was consulted to dermatology clinic, and he was given amoxicillin treatment. Punch biopsy was taken from the lesions that have revealed PG. Steroid treatment was given at 40 mg prednisolone for 2 days. The lesions were regressed immediately. He also had symptom of fever. Abdominal tomography was performed, which revealed lesions as 32×22 mm in liver and 35 mm diameter in spleen that were considered as abscess. Necrotic cells were observed from percutaneous samples, which were taken from abscess. He was given antibiotics; however, the lesions appeared again. Because immature myeloid cells were seen in blood film, he was referred to our hospital in April 2015. In his anamnesis, it was found that he was diagnosed as MDS 6 years ago and had been treated with cyclosporine at 2×100 mg for 5 years, which was stopped in January 2015. On admission, his body temperature was 38.1°C. The laboratory tests showed: hemoglobin, 9.2 g/dL; white blood cells, 5.1×103/µL; and thrombocytes, 10×103/µL. Exogenous platelet apheresis replacement was performed. He had ecchymotic lesions in both his extremities (). Magnetic resonance imaging was performed for lesions that favor tuberculosis infection. Aspiration from liver lesion revealed the presence of Mycobacterium tuberculosis, so antituberculosis treatment was started. Bone marrow investigation revealed MDS-refractory anemia with excess blasts (7%). For lesions in bilateral upper extremities, thalidomide treatment was started at 50 mg/d. Lesions began to regress, and the patient tolerated thalidomide well, so the dose was increased to 100 mg/d. After 1 month from the initiation of thalidomide treatment, the lesions in upper extremities had disappeared ().
All of the ethical considerations were strictly handled in accordance with the Helsinki Declaration. As a standard of care/action of the hospitals of Hacettepe Medical School, it was confirmed based on patient records that the study participant gave written informed consent at the time of hospitalization and relevant diagnostic/therapeutic standards of care.
Discussion
First-line treatment in PG often contains high-dose steroids, and if there is resistance to steroids, many immunosuppressive agents, such as cyclophosphamide, cyclosporine A, clofazamine, azathioprine, and chlorambucil, could also be used.Citation9 In the literature, there are some reports of patients with PG who were successfully treated with thalidomide. A 3-year-old refractory PG patient was successfully treated with thalidomide 100 mg/d.Citation10 The time required to achieve treatment response could be different between cases. For example, in one case, PG was treated with thalidomide after 6 months of initiation of therapy.Citation11 However, a refractory PG patient with penis involvement just healed in 5 days after the initiation of thalidomide with 100 mg/d.Citation12 Another PG patient responded to treatment after 10 weeks of thalidomide usage. In addition, thalidomide is effective against rheumatic diseases associated with PG. Two patients with Behcet’s syndrome and PG were successfully treated with thalidomide.Citation13,Citation14 An important concern about thalidomide usage in PG is the duration of treatment. In a PG patient, excellent treatment response was observed for 2 years with thalidomide 100 mg/d; however, after discontinuation of drug, relapse occurred.Citation15
There are several reports on PG in the English literature.Citation16,Citation17 The thalidomide activity mechanism is still not fully understood, but it is known that the result of usage of thalidomide exposes antiangiogenic effect and increases the oxidative stress.Citation18 Thalidomide increases the levels of interleukin (IL) 2, IL-4, and IL-5; however, it decreases the levels of tumor necrosis factor α, IL-6, IL-10, and IL-12.Citation19 It also modifies the secretion of interferon γ.Citation19 Thalidomide promotes proliferation and migration functions of keratinocytes. Thus, it is a very useful agent in skin lesions because it enhances reepithelialization.Citation20 Thalidomide could also be used as a treatment option for MDS.Citation21
Our patient is a complicated case who simultaneously has MDS, PG, and tuberculosis infection. The reason for thalidomide usage in our patient was the need of immune modulation without immune suppression. We did not prefer steroid and other immunosuppressive drugs because of M. tuberculosis infection. So, thalidomide was considered as the best option in our patient. Unlike previous cases, we have started the thalidomide treatment with 50 mg/d, and 1 week later, we have increased the dose to 100 mg/d. Our patient has tolerated the drug well, and excellent response was obtained after 1 month of initiation of thalidomide treatment. The plan for our patient is to continue the drug as long as the patient tolerates because there is a risk of relapse in case of discontinuation.
Conclusion
To conclude, thalidomide is a very effective drug acting as an immune modulator, which is useful in the clinical management of both MDS and PG.
Disclosure
The authors have no conflicts of interest in this work, including specific financial interests, relationships, and/or affiliations relevant to the subject matter or materials included.
References
- RuoccoESangiulianoSGravinaAGMirandaANicolettiGPyoderma gangrenosum: an updated reviewJ Eur Acad Dermatol Venereol200923100819470075
- Von den DrieschPPyoderma gangrenosum: a report of 44 cases with follow-upBr J Dermatol199713710009470924
- BennettMLJacksonJMJorizzoJLFleischerABJrWhiteWLCallenJPPyoderma gangrenosum. A comparison of typical and atypical forms with an emphasis on time to remission. Case review of 86 patients from 2 institutionsMedicine (Baltimore)2000793710670408
- BinusAMQureshiAALiVWWinterfieldLSPyoderma gangrenosum: a retrospective review of patient characteristics, comorbidities and therapy in 103 patientsBr J Dermatol2011165124421824126
- AhronowitzIHarpJShinkaiKEtiology and management of pyoderma gangrenosum: a comprehensive reviewAm J Clin Dermatol20121319122356259
- PowellFCHackettBCWallachDPyoderma gangrenosumGoldsmithLAKatzSIGilchrestBAFitzpatrick’s Dermatology in General Medicine18th edNew YorkMcGraw-Hill Companies, Inc2012371
- KimTHOhSYMyungSCPyoderma gangranosum of the penisJ Korean Med Sci200924120019949683
- FedermanGLFedermanDGRecalcitrant pyoderma gangrenosum treated with thalidomideMayo Clin Proc20007584210943240
- EhlingAKarrerSKleblFSchafflerAMuller-LadnerUTherapeutic management of pyoderma gangrenosumArthritis Rheum2004503076308415476233
- VenenciePYSauratJHPyoderma gangrenosum in a child. Treatment with thalidomideAnn Pediatr1982296769
- HeckerMSLebwohlMGRecalcitrant pyoderma gangrenosum: treatment with thalidomideJ Am Acad Dermatol1998384904919520035
- FarrellAMBlackMMBrackaABunkerCBPyoderma gangrenosum of the penisBr J Dermatol19981383373409602887
- MunroCSCoxNHPyoderma gangrenosum associated with Behcet’s syndrome – response to thalidomideClin Exp Dermatol1988134084103256462
- RustinMHGilkesJJRobinsonTWPyoderma gangrenosum associated with Behcet’s disease: treatment with thalidomideJ Am Acad Dermatol1990239419442254485
- BuckleyCSarkanyIBayoumiAHPyoderma gangrenosum with severe pharyngeal ulcerationJ R Soc Med1990835905912213811
- WollinaUPyoderma gangrenosum – a systemic disease?Clin Dermatol201533552753026321398
- WollinaUTchernevGPyoderma gangrenosum: pathogenetic oriented treatment approachesWien Med Wochenschr201416413–1426327324898196
- KimJHScialliARThalidomide: the tragedy of birth defects and the effective treatment of diseaseToxicol Sci201112211621507989
- SinghalSMehtaJThalidomide in cancerBiomed Pharmacother200256141211905508
- NascaMRO’TooleEAPalicharlaPWestDPWoodleyDTThalidomide increases human keratinocyte migration and proliferationJ Invest Dermatol199911372072410571725
- MustoPThalidomide therapy for myelodysplastic syndromes: current status and future perspectivesLeuk Res20042832533215109529