Abstract
Background
New oral anticoagulant agents, such as apixaban, rivaroxaban, dabigatran, or endoxaban, have recently become for patients an alternative option to conventional treatment in the therapy of venous thromboembolism (VTE). Thus, we aimed to review the available information on adverse events (AEs) of apixaban compared to conventional therapy (heparin or vitamin K antagonists) in randomized controlled trials (RCTs) on patients treated for VTE, with a particular attention to sex subgroups.
Methods
An electronic search in MEDLINE and Embase was performed by using the keywords “apixaban” and “venous thromboembolism”. All RCTs focused on apixaban in the treatment and prevention of VTE were evaluated for the presence of AEs. AEs were classified as serious, bleeding, and cause of discontinuation. Moreover, we also searched by using the keywords “gender” and “venous thromboembolism” and “anticoagulants”.
Results
Considering all subjects enrolled in the eleven RCTs as a whole to investigate the occurrence of AEs, we extrapolated an events/subjects rate of 57.8% for AEs (6,445/11,144), 7.7% for serious AEs (975/12,647), 9.1% for bleeding events (1,229/13,454), and 3.2% for discontinuation of apixaban (421/13,039). The percentage of AEs was lower in subjects treated with apixaban than in those treated with conventional VTE therapy (53% vs 56.3%, respectively). However, only one study provided data on separate analysis by sex of either efficacy or safety of apixaban.
Conclusion
Under the patient’s perspective, apixaban could represent a good choice in the treatment of VTE, due to its pharmacological, economical, and safety profile. These positive aspects are certainly present in both sexes, since the available studies include a correct percentage of women, but data with separate analyses by sex are extremely limited. Future clinical trials should include in their results on clinical impact and outcomes a stratification by sex, and studies aimed to evaluate possible sex-related differences for these drugs should be strongly encouraged.
Introduction
Venous thromboembolism (VTE) represents a common clinical condition that encompasses deep vein thrombosis (DVT) and pulmonary embolism (PE), with an overall annual incidence of 108 per 100,000 inhabitants in the USA.Citation1 In fact, PE and DVT are considered a different expression of the same clinical condition, since ~70% of patients with PE had a DVT, and 30%–70% of patients with DVT had a clinical or subclinical PE.Citation2 Physicians should always consider PE which represents a life-threatening condition, ranking second among causes of out-of-hospital sudden death in the general population,Citation3 and also in hospitalized patients, mortality due to PE is high.Citation4 For these reasons, treatment of VTE should be familiar to any clinician. Therapy of PE and DVT was based on anticoagulant approach with parenteral or subcutaneous heparin or oral anticoagulants, represented by warfarin or new oral anticoagulants (NOAs), such as apixaban, rivaroxaban, dabigatran, or endoxaban.Citation5 The vitamin K antagonists (VKAs) warfarin and acenocoumarol represent the old standard treatment for VTE, and their efficacy in prevention of recurrent VTE could be quantified as decreasing recurrent risk of ~3%.Citation6 The main limitations of this therapy are the need of frequent control of coagulation pattern (international normalized ratio, INR) with some costs and logistic discomfort for patients, possible food and drug interactions leading to alterations of anticoagulant effect, and high incidence of bleeding complications. Thus, a low adherence to this therapy could be an expected consequence, and trials dealing with patients on VKAs for VTE showed that poor adherence could be detected by low percent of time in therapeutic range and with an increased risk of thromboembolic complications.Citation7 NOAs include factor Xa inhibitors (rivaroxaban, apixaban, and endoxaban) and factor IIa inhibitors (dabigatran). NOAs do not require routine laboratory monitoring and frequent changes in dosage, suggesting an improvement in pharmacological adherence. However, results from a meta-analysis study of 18 randomized trials including >100,000 patients showed that total study discontinuation rates were not significantly different between NOAs and conventional therapy in VTE and prevention of stroke in atrial fibrillation (AF), whereas drug discontinuation with NOAs was significantly higher than with placebo in acute coronary syndromes.Citation8 NOAs could suffer main drug interaction, and clinical contraindications could limit their potential use; however, these drugs do not require frequent evaluations of coagulation parameters and do not show changes in their pharmacological effectiveness related to foods or body weight.Citation9,Citation10 Moreover, NOAs are considered to be a favorable alternative to heparin in long-term VTE treatment, but bleeding risk and the absence of reversal agent are their major limitations.Citation11 However, only a few data are available on possible differences by sex in the prescription of drugs, even if a little more is known on the use of antiplatelet agents (APAs). Results from a multicenter study in Italy, aiming to evaluate the existence of sex differences in treatment at hospital admission and prescription at discharge, showed the presence of statistical differences, among others, for APAs. At admission, men were more likely to be on APAs (41.7% vs 36.7%; P=0.0029), and at discharge, APAs (43.7% vs 37.3%; P=0.0003) continued to be prescribed more often in men.Citation12 A recent study carried out in the Netherlands compared adherence to NOAs with adherence to APAs. Mean adherence to NOAs was 84.2% compared with 87.3% to APAs. One in four NOAs users had a percentage of days covered by medication <80% compared with one in five APA users. No data by sex subgroups were available.Citation13
Thus, due to the paucity of available data, we decided to put ourselves in patients’ shoes, and the aim of this review was to analyze all adverse events (AEs) of apixaban compared to conventional therapy (heparin or VKAs) in randomized controlled trials (RCTs) of VTE treatment, with a particular attention to possible differences by sex.
Methods
We performed a literature search of electronic databases, MEDLINE and Embase, using the keywords “apixaban” and “venous thromboembolism”. The aim of this search was to identify all RCTs that analyze dapixaban for treatment and prevention of VTE, and the main outcome was the collection of data about AEs. AEs were classified as serious, bleeding, and cause of discontinuation. For any study, we required a minimum set of data, including author, journal and year of publication, and total number of patients treated with apixaban and/or with conventional therapy. Moreover, we made a comprehensive search by using the keywords “gender” and “venous thromboembolism” and “anticoagulants”.
Results
As for the first objective, 13 RCTs were identified, but only eleven were included in the analysis. Two RCTs were excluded because authors did not classified AEs as serious, bleeding, and cause of discontinuation.
reports the type of AEs considered only in studies in which subjects were treated with apixaban.Citation14–Citation24 Considering all subjects enrolled in the eleven RCTs as a whole to investigate the occurrence of AEs, we extrapolated an events/subjects rate of 57.8% for AEs (6,445/11,144), 7.7% for serious AEs (975/12,647), 9.1% for bleeding events (1,229/13,454), and 3.2% for discontinuation of apixaban (421/13,039). The overall percentages of AEs related to the number of patients treated with apixaban are reported in .
Figure 1 Extrapolated events/subjects rate of AEs in the eleven considered RCTs with apixaban.
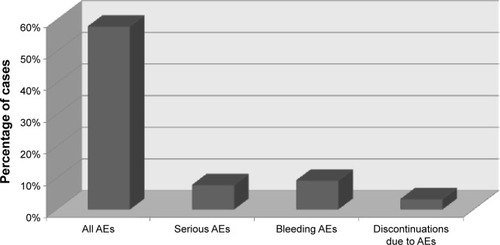
Table 1 Type of AEs in studies in which subjects were treated with apixaban
shows the AEs in different studies comparing apixaban and conventional therapy. The percentage of AEs was lower in subjects treated with apixaban than in those treated with conventional VTE therapy (53 vs 56.3%) ().
Figure 2 Number of patients, AEs, and percentages of AEs comparing apixaban and conventional therapy.
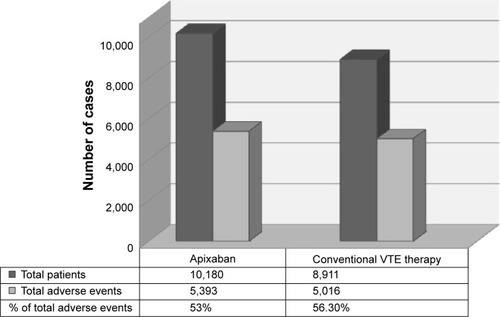
Table 2 AEs in different studies comparing apixaban and conventional therapy
provides additional data on the existence or not of subanalysis by sex in the studies comparing apixaban and conventional therapy.
Table 3 Evaluation by sex in the studies comparing apixaban and conventional therapy
Discussion
The first observation of the present study is a confirmation of a lower prevalence of AEs related to VTE prevention and treatment with apixaban compared with conventional therapy. Total AEs were reported in 57.8% of patients, 9.1% had bleeding events, 7.7% had serious AEs, and only 3.2% of patients discontinued apixaban due to AEs. Apixaban is a selective inhibitor of factor Xa with an effect on inhibition of the conversion of prothrombin to thrombin,Citation25 recently approved by health authorities in Italy for the treatment and prevention of VTE (May 23, 2015), and previously, for prevention of cerebrovascular events in patients with AF (December 2, 2013). Peak plasma concentration of apixaban is reached after 3 hours post-dose, half-life is ~12 hours, and anticoagulant effect expires after 24 hours post-dose.Citation26 Oral bioavailability is ~52%; fixed therapeutical dosage, low hepatic metabolism (only 15%), and nonrenal metabolism allow minimal drug interactions and formations of reactive metabolites.Citation26 A recent meta-analysis on risk of major bleeding related to NOAs showed a higher risk of hip surgery, acute coronary syndrome, and thromboprophylaxis in medically ill patients.Citation27 The higher rate of major bleeding in these patients was related to longer duration of NOAs therapy and probably to the higher comorbidity. After the publication of the main RCTs with NOAs, several reviews analyzed the therapeutic potential and safety of NOAs compared with VKAs.Citation28 The meta-analysis performed by van der Hulle et al showed that NOAs had lower relative risk (RR) than conventional therapy for major gastrointestinal bleeding (−0.16%), major bleeding (−0.67%), clinically relevant nonmajor bleeding (−1.77%), and fatal bleeding (−0.09%).Citation29 These data were associated with an important efficacy of NOAs in reduction of recurrent VTE (−0.24%) and overall mortality (−0.10%). Similar results were reported by Kakkos et al, with a high safety of NOAs regarding bleeding events but only a non-inferiority in preventing recurrent symptomatic VTE and reduction of DVT.Citation30 Compared to placebo, NOAs had higher efficacy on reduction of VTE recurrence (7.24% vs 1.32%) associated with higher incidence of nonmajor bleeding events and any bleeding. On the contrary, major bleeding events were not statistically different in patients treated with NOAs and placebo.Citation30 An analysis performed by Mantha and Ansell on comparative efficacy of NOAs for the treatment of VTE showed that apixaban could have more effect in VTE prevention compared with dabigatran, rivaroxaban, and endoxaban, even if no statistical difference was detected.Citation31 Similarly, Kang and Sobieraj reported a significantly lower incidence of major bleeding in patients treated with apixaban than in those treated with dabigatran and endoxaban, including lower risk of the composite end point (major and clinically relevant bleeding) compared to other NOAs.Citation32 A further meta-analysis comparing NOAs in VTE patients showed no significant differences in risk for recurrent VTE, major bleeding, or all-cause mortality between the different molecules but identified that low dose of apixaban (2.5 mg BID) was related to less clinically significant nonmajor bleeding than other NOAs.Citation33 Therefore, apixaban has been reported to be an effective and safe alternative to conventional therapy for acute or long-term treatment of VTE and to have a more favorable safety profile compared to other therapies.Citation34 Moreover, apixaban characteristics were confirmed in patients with mild and moderate renal insufficiency compared to VKAs.Citation35 NOAs, compared to conventional therapy, represent an economically acceptable strategy for VTE prophylaxis also in surgical patients.Citation36 To this extent, apixaban is associated with the greatest reduction in medical costs (−$918) compared to VTE patients treated with standard therapy.Citation37
The second main observation from this study is that the variable “sex” is not considered so much. For example, occurrence of VTE in patients with cancer is associated with unfavorable prognosis, and VTE treatment is less effective and more complicated in cancer patients. Comparison of efficacy and safety between NOAs and VKAs in cancer patients has been reported, but there are no guideline recommendations for women-specific cancer types or women-specific issues in the prevention and treatment of VTE.Citation38 Only a very minimal part of the studies comparing apixaban vs conventional therapy takes sex into consideration. In the ARISTOTLE study, 11,785 (64.7%) men and 6,416 (35.3%) women with AF or flutter were randomized to receive either warfarin or apixaban. Results showed that women had a similar rate of stroke or systemic embolism but a lower risk of mortality and less clinically relevant bleeding than men.Citation39 As for the previously cited RCTs on treatment of VTE, only one study provided data on separate analysis by sex of either efficacy or safety of apixaban.Citation14 Such a lack of data on sex subgroups is rather surprising. In fact, women are at higher risk of VTE, even though age plays crucial role. Results from an epidemiologic study on hospitalization for PE in a large population of Northwestern Italy (60,853 patients, 59.6% females, mean age 73±14 years) found an overall crude incidence rate significantly higher for women compared with men (55.4 and 40.6 events per year per 100,000 inhabitants, respectively; P<0.001), but this difference completely disappeared after standardization for age.Citation40 Again, women are at risk of VTE after total hip arthroplasty or total knee arthroplasty. A study on 14 retrospective case–control or prospective cohort studies, including 18,075 patients who developed VTE after total hip arthroplasty or total knee arthroplasty out of a total of 1,723,350 cases, found that three main risk factors were significantly associated with VTE: history of VTE, varicose vein, and congestive cardiac failure. However, authors recognized other six significant factors increasing VTE risk, such as female sex, age ≥80 years, hypertension, active cancer, obesity (BMI ≥30), and black race.Citation41 The outcome during the course of anticoagulant therapy may differ according to the patient’s sex, but available data are not always univocal. According to the Spanish data from the Registro Informatizado Enfermedad Trombo Embólica Registry on >47,000 patients, women (51% of total sample) were older, more likely presented with PE, and were more likely to have recent immobilization but less likely to have cancer than men. Compared with men, women had a lower rate of DVT recurrences, a higher rate of major bleeding, and higher mortality due to PE, although rate of PE recurrences was similar. However, on multivariable analysis, any influence of sex on the risk for recurrent DVT, major bleeding, or fatal PE was no longer statistically significant.Citation42 A subanalysis of the same registry focused on the outcome of cancer patients with acute VTE showed that, compared with men, women had a significantly lower rate of fatal bleeding and death, and a nonsignificantly lower rate of PE recurrences and major bleeding.Citation43 Also, the meta-analysis studies, mostly addressed to both AF and VTE patients, are not conclusive. A systematic review and meta-analysis was performed to determine if the risk of major bleeding may differ between men and women receiving anticoagulation for AF or VTE. Forty-two studies including >94,000 patients were analyzed: 83% had AF and 17% had VTE; 37,250 patients (40%) were women. The RR of major bleeding for men vs women was 1.02, in particular 1.02 in patients with AF and 0.80 in patients with VTE. Thus, the risk of major bleeding on anticoagulation seems to be the same in both sexes, especially in the case of AF, whereas in patients with VTE, the risk of bleeding may be marginally lower in men compared with women.Citation44 Again, another recent comprehensive systematic review and meta-analysis of 13 studies (>100,000 patients) showed that NOAs had a similar efficacy and safety compared with VKAs in female and male patients treated for nonvalvular AF and acute VTE. However, in the extended treatment of VTE, a trend toward an increased risk of bleeding in male patients as compared with female patients was observed for NOAs compared with placebo.Citation45
As for low adherence to anticoagulant therapy, there are no univocal data available. Previous findings reported that risk factors related to lower adherence of VKAs therapy included younger age, male sex, poor cognitive function, poverty, and higher educational attainment.Citation46 In a study on a total of 2,068 patients in Denmark, performing self-management of VKAs, males achieved a significantly better therapeutic INR control than females. In fact, females spent 71.1% of the time within therapeutic INR target range, whereas males spent 76.4% (P<0.0001), but the incidence of major complications was low and similar in both sexes.Citation47 Again, a Swedish study evaluated the persistence with presently available antithrombotic treatments in AF patients. The overall persistence with any oral anticoagulant was 88.2% at 1 year and 82.9% at 2 years. After 1 year, the crude persistence was 85.0% with warfarin, 85.9% with apixaban, 74.4% with dabigatran, and 77.4% with rivaroxaban. Multivariate analysis confirmed significantly higher persistence with warfarin and apixaban than with dabigatran or rivaroxaban, persistence at 1 year after initiations on warfarin, and that apixaban had higher odds for persistence than initiation on dabigatran and rivaroxaban. However, female sex was one of the factors significantly associated with lower persistence.Citation48 On the contrary, different results were reported by a recent study aimed to assess self-reported anticoagulation adherence in a tertiary center anticoagulation clinic. Main indications for anticoagulation were VTE (72%) and AF (18%); 74% of patients were on VKAs, and 26% on NOAs (rivaroxaban 79%, dabigatran 19%, apixaban 2%). Predictors of anticoagulation adherence were, in decreasing order, use of additional oral medications (odds ratio [OR] =2.78), retired employment status (OR =2.31), female sex (OR =1.58), and age (OR =1.02). In multivariate analyses, age, female sex, and use of other oral medications remained significantly associated with anticoagulation adherence.Citation49
In conclusion, in the patient’s perspective, apixaban could represent a good choice in the treatment of VTE, due to its pharmacological, economical, and safety profile. These positive aspects are probably present in both sexes, since the available studies include a correct percentage of women. Future clinical trials should include in their results on clinical impact and outcomes a stratification by sex, and studies aimed to evaluate possible sex-related differences for these drugs should be strongly encouraged.
Acknowledgments
This work has been supported, in part, by a research grant from the University of Ferrara (Fondo Ateneo Ricerca).
Disclosure
No conflicts of interest exist for any author.
References
- GoASMozaffarianDRogerVLAmerican Heart Association Statistics Committee and Stroke Statistics Subcommittee. Executive summary: heart disease and stroke statistics – 2014 update: a report from the American Heart AssociationCirculation2014129339941024446411
- SteinPDMattaFMusaniMHDiaczokBSilent pulmonary embolism in patients with deep venous thrombosis: a systematic reviewAm J Med2010123542643120399319
- ManfrediniRPortaluppiFGrandiEFersiniCGalleraniMOut-of-hospital sudden death referring to an emergency departmentJ Clin Epidemiol19964988658688699205
- FabbianFGalleraniMPalaMIn-hospital mortality for pulmonary embolism: relationship with chronic kidney disease and end-stage renal disease. The hospital admission and discharge database of the Emilia Romagna region of ItalyIntern Emerg Med20138873574023247683
- KonstantinidesSVTorbickiAAgnelliGTask Force for the Diagnosis and Management of Acute Pulmonary Embolism of the European Society of Cardiology (ESC)2014 ESC guidelines on the diagnosis and management of acute pulmonary embolismEur Heart J20143543303330693069a3069k25173341
- HuttenBAPrinsMHDuration of treatment with vitamin K antagonists in symptomatic venous thromboembolismCochrane Database Syst Rev20061CD00136716437432
- Di MinnoASpadarellaGTufanoAPriscoDDi MinnoGEnsuring medication adherence with direct oral anticoagulant drugs: lessons from adherence with vitamin K antagonists (VKASs)Thromb Res2014133569970424525314
- ChatterjeeSSardarPGiriJSGhoshJMukherjeeDTreatment discontinuations with new oral agents for long-term anticoagulation: insights from a meta-analysis of 18 randomized trials including 101,801 patientsMayo Clin Proc201489789690724996233
- KubitzaDBeckaMZuehlsdorfMMueckWBody weight has limited influence on the safety, tolerability, pharmacokinetics, or pharmacodynamics of rivaroxaban (BAY 59-7939) in healthy subjectsJ Clin Pharmacol200747221822617244773
- UpretiVVWangJBarrettYCEffect of extremes of body weight on the pharmacokinetics, pharmacodynamics, safety and tolerability of apixaban in healthy subjectsBr J Clin Pharmacol201376690891623488672
- VersoMAgnelliGPrandoniPPros and cons of new oral anticoagulants in the treatment of venous thromboembolism in patients with cancerIntern Emerg Med201510665165625840679
- HanemmjerSSodihardjoFHorikxATrends in antithrombotic drug use and adherence to non-vitamin K oral anticoagulants in the NetherlandsInt J Clin Pharm20153761128113526243531
- SantaluciaPFranchiCDjadeCDGender differences in drug use in hospitalized elderly patientsEur J Intern Med201526748349026209883
- AgnelliGBullerHRCohenAOral apixaban for the treatment of acute venous thromboembolismN Engl J Med2013369979980823808982
- AgnelliGBullerHRCohenAApixaban for extended treatment of venous thromboembolismN Engl J Med2013368869970823216615
- GoldhaberSZLeizoroviczAKakkarAKApixaban versus enoxaparin for thromboprophylaxis in medically ill patientsN Engl J Med2011365232167217722077144
- LassenMRRaskobGEGallusAPineoGChenDPortmanRJApixaban or enoxaparin for thromboprophylaxis after knee replacementN Engl J Med2009361659460419657123
- LassenMRGallusARaskobGEPineoGChenDRamirezLMADVANCE-3 InvestigatorsApixaban versus enoxaparin for thromboprophylaxis after hip replacementN Engl J Med2010363262487249821175312
- LevineMNGuCLiebmanHAA randomized phase II trial of apixaban for the prevention of thromboembolism in patients with metastatic cancerJ Thromb Haemost201210580781422409262
- LassenMRDavidsonBLGallusAPineoGAnsellJDeitchmanDThe efficacy and safety of apixaban, an oral, direct factor Xa inhibitor, as thromboprophylaxis in patients following total knee replacementJ Thromb Haemost20075122368237517868430
- Botticelli Investigators, Writing CommitteeBullerHDeitchmanDPrinsMSegersAEfficacy and safety of the oral direct factor Xa inhibitor apixaban for symptomatic deep vein thrombosis. The Botticelli DVT dose-ranging studyJ Thromb Haemost2008681313131818541000
- LassenMRRaskobGEGallusAPineoGChenDHornickPADVANCE-2 investigatorsApixaban versus enoxaparin for thromboprophylaxis after knee replacement (ADVANCE-2): a randomised double-blind trialLancet2010375971780781520206776
- NakamuraMNishikawaMKomuroIApixaban for the treatment of Japanese subjects with acute venous thromboembolism (AMPLIFY-J Study)Circ J20157961230123625912695
- BarrettYCWangJKnabbRMohanPApixaban decreases coagulation activity in patients with acute deep-vein thrombosisThromb Haemost2011105118118920941459
- JiangXCrainEJLuettgenJMSchumacherWAWongPCApixaban, an oral direct factor Xa inhibitor, inhibits human clot-bound factor Xa activity in vitroThromb Haemost2009101478078219350128
- RaghavanNFrostCEYuZApixaban metabolism and pharmacokinetics after oral administration to humansDrug Metab Dispos2009371748118832478
- SardarPChatterjeeSLavieCJRisk of major bleeding in different indications for new oral anticoagulants: insights from a meta-analysis of approved dosages from 50 randomized trialsInt J Cardiol201517927928725464465
- ImbertiDGalleraniMManfrediniRTherapeutic potential of apixaban in the prevention of venous thromboembolism in patients undergoing total knee replacement surgeryJ Thromb Thrombolysis201234220821322466929
- van der HulleTKooimanJden ExterPLDekkersOMKlokFAHuismanMVEffectiveness and safety of novel oral anticoagulants as compared with vitamin K antagonists in the treatment of acute symptomatic venous thromboembolism: a systematic review and meta-analysisJ Thromb Haemost201412332032824330006
- KakkosSKKirkilesisGITsolakisIAEditor’s choice – efficacy and safety of the new oral anticoagulants dabigatran, rivaroxaban, apixaban, and edoxaban in the treatment and secondary prevention of venous thromboembolism: a systematic review and meta-analysis of phase III trialsEur J Vasc Endovasc Surg201448556557524951377
- ManthaSAnsellJIndirect comparison of dabigatran, rivaroxaban, apixaban and edoxaban for the treatment of acute venous thromboembolismJ Thromb Thrombolysis201539215516524989022
- KangNSobierajDMIndirect treatment comparison of new oral anticoagulants for the treatment of acute venous thromboembolismThromb Res201413361145115124713109
- AlotaibiGAlsalehKWuCMcmurtryMSDabigatran, rivaroxaban and apixaban for extended venous thromboembolism treatment: network meta-analysisInt Angiol201433430130825056161
- SobierajDMColemanCIPasupuletiVDeshpandeAKawRHernandezAVComparative efficacy and safety of anticoagulants and aspirin for extended treatment of venous thromboembolism: a network meta-analysisThromb Res2015135588889625795564
- PathakRPanditAKarmacharyaPMeta-analysis on risk of bleeding with apixaban in patients with renal impairmentAm J Cardiol2015115332332725527282
- MahmoudiMSobierajDMThe cost-effectiveness of oral direct factor Xa inhibitors compared with low-molecular-weight heparin for the prevention of venous thromboembolism prophylaxis in total hip or knee replacement surgeryPharmacotherapy201333121333134023625693
- AminAJingYTrocioJLinJLingohr-SmithMGrahamJEvaluation of medical costs associated with use of new oral anticoagulants compared with standard therapy among venous thromboembolism patientsJ Med Econ2014171176377025078794
- BauersachsRMGuidelines for the management of cancer and thrombosis – special aspects in womenThromb Res2015135Suppl 1S13S22
- VinereanuDStevensSRAlexanderJHClinical outcomes in patients with atrial fibrillation according to sex during anticoagulation with apixaban or warfarin: a secondary analysis of a randomized controlled trialEur Heart J201536463268327526371113
- DentaliFAgenoWPomeroFFenoglioLSquizzatoABonziniMTime trends and case fatality rate of in-hospital treated pulmonary embolism during 11 years of observation in Northwestern ItalyThromb Haemost Epub2015917
- ZhangJChenZZhengJBreuschSJTianJRisk factors for venous thromboembolism after total hip and total knee arthroplasty: a meta-analysisArch Orthop Trauma Surg2015135675977225854654
- Blanco-MolinaAEneaIGadelhaTSex differences in patients receiving anticoagulant therapy for venous thromboembolismMedicine (Baltimore)2014931730931725398066
- Martín-MartosFTrujillo-SantosJBarrónMGender differences in cancer patients with acute venous thromboembolismThromb Res2015135Suppl 1S12S1525903526
- LapnerSCohenNKearonCInfluence of sex on risk of bleeding in anticoagulated patients: a systematic review and meta-analysisJ Thromb Haemost201412559560524977286
- DentaliFSironiAPGianniMGender difference in efficacy and safety of nonvitamin K antagonist oral anticoagulants in patients with nonvalvular atrial fibrillation or venous thromboembolism: a systematic review and a meta-analysis of the literatureSemin Thromb Hemost201541777478726408921
- KneelandPPFangMCCurrent issues in patient adherence and persistence: focus on anticoagulants for the treatment and prevention of thromboembolismPatient Prefer Adherence20104516020361065
- NilssonHGroveELLarsenTBSex differences in treatment quality of self-managed oral anticoagulant therapy: 6,900 patient-years of follow-upPLoS One2014911e11362725415603
- ForslundTEttermarkBHjiemdahlPComparison of treatment persistence with different oral anticoagulants in patients with atrial fibrillationEur J Clin Pharmacol Epub20151127
- CastellucciLAShawJvan der SalmKSelf-reported adherence to anticoagulation and its determinants using the Morisky medication adherence scaleThromb Res2015136472773126272305
