Abstract
Introduction
Although affecting an estimated 35% of the population, Dry Eye is not well understood by patients and the medical community. As a result, both in research and clinical settings, diagnostic and treatment protocols tend to be non-specific, ad hoc, and inadequate, with a narrow industry-driven focus. The purpose of this convening was to propose a research roadmap that orients Dry Eye researchers toward a comprehensive patient-centered approach to diagnosing and treating Dry Eye, Meibomian gland dysfunction (MGD), and related comorbidities with a goal of improving clinical outcomes for Dry Eye/MGD patients.
Methods
Sixteen participants, including Dry Eye/MGD patients, caregivers, and patient advocates together with a group of experts in Dry Eye, MGD and other fields identified gaps in research on Dry Eye and MGD diagnostic and treatment approaches (age range 20–80; male to female ratio of 7:11; patients: 7). During a 2-day virtual convening, participants were assigned to topic-specific focus-group sessions to discuss and develop research questions pertaining to Dry Eye and MGD. The research questions were compiled into a proposed patient-centered roadmap for Dry Eye and MGD research. Two additional participants contributed to the proposed roadmap following the convening.
Results
The focus groups identified over 80 patient-centered research questions important to patients and other stakeholders and compiled these into a proposed research roadmap.
Conclusion
The convened stakeholders aim to establish a cohesive and comprehensive patient-centered approach to treating Dry Eye, Meibomian Gland Dysfunction, and comorbidities. The research roadmap will serve as a reference for researchers, educational institutions, clinicians, and others evaluating diagnostic and treatment protocols in Dry Eye and MGD.
Introduction
Dry Eye is a complex, multifactorial disease that often involves numerous comorbidities. These can cause severe pain, mental distress, suicidal ideation, suicide, and applications for euthanasia (Matt Borcina, personal communication, November 15, 2023). There are two Dry Eye variants – aqueous deficient Dry Eye (AD DE; prevalence 20%) and evaporative Dry Eye (EDE; prevalence 85%).Citation1 Both often coexist as mixed Dry Eye. Although affecting an estimated 35% of the population, Dry Eye is not well understood.Citation2 Diagnostic and treatment protocols tend to be non-specific, ad hoc, and inadequate, with a narrow industry-driven focus that largely ignores patients’ actual symptoms and their etiology, the underlying cause of 90% of EDE (c), and other ocular surface comorbidities.Citation3
In three prior studies,Citation4–6 patient input on research priorities was either meager or nonexistent, a deficiency in study design given high prevalence.Citation2 In one of three studies, input was solicited from only one patient of 39 total participants.Citation4 In another study,Citation5 patients were asked to prioritize outcomes culled from a previous clinicians-only study.Citation6
For this project which aims to amplify the patient perspective, a team of Dry Eye/MGD patients, caregivers, and patient advocates gathered with a group of experts in Dry Eye, MGD and other fields to identify gaps in research on diagnostic and treatment approaches. These research opportunities were compiled into a patient-centered roadmap for Dry Eye and MGD.
Methods
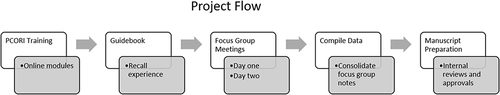
In December 2021, the Not A Dry Eye Foundation received a Stakeholder Convening Support grant from the Patient-Centered Outcomes Research Institute (PCORI) for a project titled “Engaging Stakeholders to Develop a Roadmap for Dry Eye and MGD-PCORI-Funded Research”. [EASCS-23147]. The flow of the project is described in .
Figure 1 Phases and Project Flow. The phases of the project (white rectangles) and primary activity (grey rectangles).
Core Team
To assist in the design, development, and production of the event, the Project Lead (PL) assembled a core team with complimentary skills, engaging the services of an Instructional Systems Designer (ISD) and a Production Manager (PM) who would also serve as a Communication Manager (CM). The ISD’s primary role was to ensure all participants were sufficiently familiar with the subject matter so that project goals would be met. This included: review and consultation on original and PCORI-provided training, developing background materials such as a guidebook on Dry Eye and MGD provided to participants prior to the convening, designing templates for guided activities during focus group sessions, pre- and post-convening communication with the participants, focus group assignments and roles. The PM managed both technical and non-technical aspects of the production, maintained participant lists, the pre-event and convening schedules, scheduled pre-convening video conferencing (Zoom) training, developed and maintained the pre-convening document lists, hosted and managed all Zoom general and focus group sessions during the convening, and identified technical equipment needs and requirements. The CM handled all participant pre-convening email communication and electronic signing of participant agreements.
Training
Project Training: Prior to the convening, each participant was individually briefed by the PL on the goals and methodology of the project. In addition, the PL reviewed the project objectives and its methodology during the required Zoom training sessions. Each convening participant was required to attend at least one training session hosted by the PM/CM on Zoom.
Zoom: To minimize technical issues that might interfere with the convening, Zoom training sessions were held several weeks prior to the convening. Participants were required to attend at least one Zoom training session, and several participants requested additional one-on-one training.
PCORI/PCOR: All participants were required to complete PCORI online training modules.Citation7–10 For participants regularly conducting research two PCORI training modules were optional.Citation9,Citation10
Guidebook: All convening participants received a guidebookCitation11 prior to the convening covering a variety of topics from an overview of the purpose of the project to links to PCORI online training modulesCitation7–10 and information about Dry Eye and MGD. (See Guidebook.)
Guidebook
The PL and ISD prepared a GuidebookCitation11 that covered a variety of topics pertinent to the convening and work product. A PDF version of the Guidebook was distributed to the participants several days before the convening along with instructions to review the contents and complete the included exercises. The exercises were designed to help participants recall prior to the convening their experience(s) with Dry Eye, MGD and common comorbidities via reflection, individual brainstorming, or other grounding methods. An introduction to PCORI principles and links to online PCORI training modulesCitation7–10 were included as were instructions on how to pronounce medical terms such as Meibomian and conjunctivochalasis that may have been unfamiliar to some participants. (See Guidebook Table of Contents for a complete list of topics covered.)
The topics in the Guidebook largely mirrored the topics discussed in the convening focus group sessions. (See Focus Group Sessions Topics.) The Guidebook was also designed as a reference to be used by participants during the convening and later, during reviews of the work product.
Guidebook Table of Contents
Introduction
Goal of the project
Not A Dry Eye Foundation
PCORI
PCORI online training
The PCORI approach to patient-centered outcomes research
Engaging in stakeholder-driven research
Developing research questions
Designing the research study
The research framework at a glance
What is a research roadmap?
How do I pronounce?
Terms
Acronyms
Eye anatomy
Definitions of Dry Eye
Pathophysiology/causes of disease
Symptoms
Factors contributing to disease and symptoms
Diagnosis
Patient questionnaires
At-home/OTC therapies
Physician-prescribed and administered therapies
Patient, provider, regulatory agency awareness/education
Convening Participants
Each participating stakeholder was invited based on their professional expertise or personal experience with DE, MGD, and comorbidities, or, other relevant professional expertise; eg, information technology.
Convening participants: n = 16
Additional stakeholders: n = 2
Age range: 20 < n < 80
Gender female: n = 11; male: n = 7
The following stakeholder groups were represented. In some cases, one participant represented more than one group (+ indicates post-convening contribution to roadmap).
Patient: n = 7
Patient advocate: n = 5
Caregiver: n = 3
Ophthalmic technician: n = 1
Administration: n = 2
Ophthalmology: n = 1 (+1)
Optometry: n = 1 (+1)
Other medical specialty: n = 1 (Internal medicine)
Research: n = 4 (+1)
Information Technology: n = 1
Instructional Systems Design: n = 1
Convening
The convening was held via Zoom video conferencing. Each focus group session lasted 1 hour followed by a 10- to 15-minute report-out to all participants and a 10- to 15-minute break.
Focus groups identified gaps in research and drafted proposed research questions to mitigate those gaps. Focus group topics included: comorbidities, factors contributing to disease and/or symptoms, diagnosis, patient questionnaires, disease definition and pathophysiology, psycho-social impact of disease on patients, training/education, OTC treatments, and prescribed treatments.
Participant Assignments
Generally, no less than 4 and no more than 7 participants were assigned to a single focus group session ensuring a high level of engagement by all. Patients were represented in each focus group. Three concurrent focus group sessions were held simultaneously throughout both days.
One member of each focus group was assigned the role of room leader. The room leader was tasked with facilitating the session process (eg, reading instructions out loud, maintaining the group’s focus on its assignments) and ensuring the group completed its assignments on time. One other individual was assigned the role of scribe. This individual recorded video of the session, downloaded a discussion guide and template for taking notes, shared their screen, took notes, and filled out the templates provided (). Scribes were trained in using the note-taking and screen share tasks in the days prior to the convening.
Table 1 Research Question Template
Throughout both days, the PL and Host were available for content-related or technical questions respectively.
Focus Groups: Method
Through Zoom chat, the assigned scribe received a unique link to a document that outlined that focus group’s assignments. The document included instructions for the Room Leader (driving discussion and time keeping), the Scribe (recording the session and taking notes), and all participants (prompts to identify gaps in research and developing research questions) as well as a template for note taking.
Documents were stored on a secure Google share drive where files were saved automatically and continuously, that is, as soon as a change was made to the file. All documents were also backed up automatically. The scribe typed notes on a continuous and ongoing basis directly into each template () while sharing their screen so all participants could review and comment on the notes taken. Thereafter, at the close of each focus group session, the PL revoked access to the files so they could not be intentionally or accidentally altered, thus ensuring integrity of the work product.
Results
Focus Groups: Comorbidities
Focus groups developed the following list of comorbidities. Proposed related research questions are listed in . An additional research question, “How can MGD, ATD, conjunctivochalasis and other associated comorbidities be prevented?” was discussed but not included in .
Table 2 Research Questions on Comorbidities, Symptoms, and Factors
Conjunctivochalasis
ATD (Aqueous Tear Deficiency)
Allergies (ie, environmental, drug- or preservative-induced)
Autoimmune disease
Bacterial infections (anterior blepharitis)
Blepharitis
Eyelash crusting, eyelashes stick together
Demodex mite overpopulation
Depression, psychiatric issues or mental health issues
Dermatologic disease
Distichiasis
Epiphora
Hormonal imbalances
Lagophthalmos
Lagophthalmos, nocturnal and blink
Lashes getting stuck in eye
Lid abnormalities, eg, Bell’s palsy, ptosis
Lid wiper epitheliopathy (added during review process)
Map-dot-fingerprint dystrophy/anterior basement membrane dystrophy (ABMD)
MGD
Ocular immune disease/Grave’s disease
Post-viral Dry Eye/Post-COVID Dry Eye
Prior ophthalmic surgeries where cornea is involved
Reflex tearing
Rosacea
Sjogren’s syndrome
Superior limbic keratoconjunctivitis (SLK)
Spontaneous corneal abrasion
Systemic autoimmune disease
Thyroid disease, causes and/or contributing factors
Trauma history
Trichiasis
Focus Groups: Symptoms
Focus groups developed the following list of symptoms. Proposed related research questions are listed in .
Awareness of eyes
Blinking frequently
Blurred vision
Burning
Constant unrelenting discomfort in the eyes
Crawling on eye lashes
Crusting
Debris in eyes
Debris in eye lashes
Difficulty opening eyes
Drippy eyes
Dry eyes
Epiphora (overflowing of tears)
Eye pain
Eyes feel exposed
Eyes feel like open wounds
Eyes feel like they are made out of wood (due to medications including steroids)
Feels like crushed glass in the eyes
Foreign body sensation
Gritty, scratchy, or sandy
Headache
Heavy eyes, heavy eye lids
Inflammation
Itching
Lashes falling out frequently, sticking to eyeball
Lids stick to eyes
Sensation of menthol, acid, or gasoline in the eyes
Misdirected lashes
Mucous discharge
Pain or other discomfort when reading, driving, or doing other activities that requires focus
Puffy eyelids
Raw
Red eyes and lid margins
Redness
Saponification, frothy tears
Screwdriver in eye at waking
Sensitivity to fumes and perfumes
Sensitivity to light (photophobia)
Sensitivity to many environmental factors
Sensitivity to temperature
Sensitivity to wind
Sticky eyes
Stinging
Swollen eyes
Tearing
Tired eyes
Tissues under eye lids
Twitching eye lids
Unable to take focus away from eyes, meaning that cognitive awareness is constantly on the eyes instead of no awareness of eyes.
Watery eyes
Wetness
Participants recognized the following as symptoms of interests, though did not propose related research questions
Blurred vision
Burning
Debris in eye lashes
Difficulty opening eyes
Feeling of crushed glass in eyes
Foreign body sensation
Heavy eyes/eyelids
Lids stick to eyes
Menthol/acid/gasoline
Misdirected lashes
Mucous discharge
Redness
Stinging
Tearing (when exposed to wind/environment)
Tired/heavy eyes
Focus Groups: Factors
Focus groups developed the following list of factors that contribute to Dry Eye, MGD, and comorbidities, and proposed the research questions listed in : age and stage of life (eg, pregnancy, menopause, andropause), binge-eating, climate, decreased/no social interaction leading to isolation and poor quality of life, environment, screen time, gender, genetics/heredity, sun exposure, hygiene (eg, cleansing methods and substances used), stress, use of cosmetics, exposure to particulate matter (eg, dust, smoke), exposure to toxins (eg, swimming in chlorinated pools without goggles, exposure to chemicals, occupational exposure), race, ethnicity, religion, diet and nutrition, blinking pattern, drying side effects due to medications/drugs (OTC or prescription), iatrogenic - exposure to medications (eg, anticholinergics, antihistamines, isotretinoin (ie, Accutane), retin-A cream), iatrogenic - surgeries/procedures (eg, LASIK, photorefractive keratectomy (PRK), cataract, pterygium, Botox injections, ptosis repair), eyelid tattoo.
Focus Groups: Diagnosis
Focus groups developed the following list of tests and exams: single Schirmer’s with topical anesthetic; serial Schirmer’s test with topical anesthetic; slit lamp exam including eversion of the upper lid; stimulation inside the nose; fluorescein clearance test (FCT); tear break-up time (TBUT); Meibomian glands expressibility; meibum clarity, fluidity, color, presence of particulate matter, volume; lid tenderness; meibography; confocal microscopy; tear osmolarity; MMP-9 enzymes; Meibomian gland probing (findings during treatment); bacteria test; demodex test; lissamine green staining; fluorescein staining; tear meniscus height; lipid layer thickness; facial skin evaluation; corneal sensation. The proposed research questions are listed in .
Table 3 Research Questions on Diagnosis, Questionnaires, Definition and Pathophysiology, Impact, at-Home and Over-The-Counter (OTC) Therapies, Physician-Prescribed Treatments, and Awareness and Education
One focus group considered the accuracy of two Dry Eye questionnairesCitation12,Citation13 frequently administered to patients in both clinical and research settings. The group discussed potential issues with the questionnaires in severe cases or occult cases when signs and symptoms do not align, and developed an associated research question ().
Focus Group: Definition and Pathophysiology
Definition
One focus group with 7 participants discussed the definition of Dry Eye and disease pathophysiology.
First the group reviewed the DEWSII 2017 definition of Dry Eye:
Dry eye is a multifactorial disease of the ocular surface characterized by a loss of homeostasis of the tear film, and accompanied by ocular symptoms, in which tear film instability and hyperosmolarity, ocular surface inflammation and damage, and neurosensory abnormalities play etiological roles.Citation14
The group agreed that the disease is multifactorial but did not agree that a) osmolarity was specific to Dry Eye, b) patients are always symptomatic (they are often asymptomatic) and c) neurosensory abnormalities, being exceedingly rare, always play etiological roles.
Although the DEWSII Committee developed the 2017 definition of Dry Eye by consensus, the focus group believed there was a potential for bias due committee members’ reported conflicts of interestCitation14–16 as well as the fact that patients were sparsely represented on the project overall.Citation16
Pathophysiology: Inflammation
The focus group discussed the commonly aired commercials for RESTASIS 0.04%Citation17 which state, Dry Eye is caused by “reduced tear production due to inflammation”.
The group made the following comments:
The statement is too narrow
Lack of redness does not mean there is no inflammation or an organic cause
Pathophysiology: Ocular Neuropathic Pain
The focus group discussed ocular neuropathic pain, called “pain without stain” because patient symptoms are not indicated by clinical signs.
The focus group made the following comments:
Many conditions can lead to “pain without stain” including: uncorrected refracted error, sinusitis, migraine, occipital neuralgia, and diseases that are missed, misdiagnosed or incorrectly evaluated such as ATD, MGD, conjunctivochalasis, pinguecula, etc. In all cases, a specific diagnosis should be sought.
Doctors should not be satisfied if they find a single disease and make a single diagnosis because of the high prevalence of comorbidities that lead to ocular surface pain.
Even with an accurate diagnosis, if treatment is not targeted, patient symptoms will persist.
Pathophysiology: Models of MGD
The focus group discussed 5 models describing the proximate cause of MGD:
Hyperkeratinization: keratin covers the orifice and excretory duct
Thickened meibum: meibum does not flow out of the glands
Stress: leads to thickened meibum and hyperkeratinization
Solutes in tear film: flow onto the lid margin causing damage at the orifice that leads to inflammation
Periductal fibrosis: invades and disrupts the glands
The group made the following comments:
Models 1–4, hyperkeratinization, thickened meibum, stress, and solutes lead to model 5, periductal fibrosis
Periductal scar tissue chokes off the duct
The flow of oil is blocked increasing the pressure behind the blockage leading to atrophy of the glands
The underlying cause of obstructive MGD is not fully realized
Commercial interests of large entities impact the dissemination of information about the proximate cause of MGD.
More information is needed to validate the model; use of repeatable experiments can help
Study disease as it develops in young adults or teenagers
Comorbidities can lead to Meibomian gland disease
Proposed research questions are detailed in . Participants noted the importance of definitively determining the proximate cause of MGD.
Focus Group: Impact
One focus group discussed the impact Dry Eye, MGD, and related comorbidities had on patient quality-of-life (QOL). The group was presented with a list of emotions experienced and behaviors displayed by Dry Eye patients (), instructed to identify gaps in the list, and develop associated research questions ().
Table 4 Impact
The group noted that although the lists they developed were long, if given more time, they might be even longer. Regardless of length, the group agreed that the reported impact of disease on Dry Eye patients illustrates the importance of early treatment, before psychological impact becomes severe and the patient’s QOL declines.
While brainstorming possible research questions, the focus group noted that many items listed merit both further discussion and dedicated research projects, such as assessing incidence and impact on QOL. Three proposed research questions are listed in .
Focus Groups: At-Home and OTC Therapies
Three concurrent focus groups discussed at-home and OTC therapies typically used by patients with or without medical supervision.
Participants were presented with a list of at-home and OTC therapies organized by disease, and life-style changes, asked to list any additional OTC or at home treatments, and write associated research questions ().
Following is a list of at-home and OTC therapies for various conditions (*indicates added by Focus Group):
ATD
Lubricating eye drops, with preservatives
Lubricating eye drops, preservative-free
Lubricating eye drops with varying degrees of viscosity
Lubricating eye drops, emulsions*
Lubricating sprays and mists
Lubricating gels
Lubricating ointments
Wrap-around glasses
Nocturnal lagophthalmos
Lubricating ointments
Moisture-chamber goggles
Taping eyes closed: SleepTite/SleepRite*, amblyopia patch*, EyeLocc patch*
MGD
Warm compresses
Lid scrubs and washes
Lid expression
Lid/lash hygiene
Demodex Mites
Tea tree oil wipes: Cliradex, Blephadex, Eyeeco products*, lip balm with tea tree oil*
Zocular
OcuSOFT cleanser*
Supportive Nutritional Therapy
Omega-3 fatty acids
Various oral supplements
Eliminating caffeine
Treating food sensitivities
Water and hydration
Limiting/eliminating alcohol*
Allergies
Topical allergy drops
Oral allergy medications
Cold compresses or ice
Life-Style Changes
Reduce gazing activity
Avoid winds and drafts
Avoid dry environments
Avoid cold
Avoid fumes
Limit exposure to allergens, toxins, and other potential irritants
Sleeping
Other Therapies
Blinking exercises
Blink reminder app
Irrigation with sterile preservative free saline or buffered saline solution*
Focus Groups: Physician-Prescribed Treatments
Three concurrent focus groups discussed physician-prescribed treatments. Participants were presented with a list of treatments organized by disease, and life-style changes, asked to identify any gaps, and write associated research questions ().
Following is a list of physician-prescribed therapies for various conditions (* indicates added by Focus Group):
Allergies
Prescription eye drops
Prescription oral medications
Desensitization therapy
Irrigation with sterile preservative-free saline or buffered saline solution*
ATD
Amniotic membrane transplant surgery
Autologous serum tears
Cevimeline (Evoxac®) and Pilocarpine (Salagen®)
Cyclosporine-based treatments: RESTASIS® 0.04%, Cequa 0.09%
Contact lenses that are very wet, eg, Dailies Total1 One-Day Contact Lenses (Alcon)
LACRISERT inserts (if aqueous tear volume is sufficient for dissolving plugs)
Narrowing the opening between the eye lids
Punctal cautery (thermal and other methods)
Punctal plugs
Scleral lenses
Nasal spray that triggers tear production (Tyrvaya)
Weights or springs in eye lids
Wet contact lenses
Lifitegrast ophthalmic solution 5% (Xiidra™)
Blepharospasm
Botulinum toxin (Botox)
Conjunctivochalasis/SLK
Amniotic membrane transplant (AMT)
Other ocular surface reconstruction methods
Prokera*
Delayed Tear Clearance
0.9% sterile saline wash
Demodex
Ivermectin, oral
Ivermectin, topical
Exfoliation
Infections
Antibiotic drops and ointments
Antifungal medications
Inflammation/Inflammation Unspecified Source
Cyclosporine-based treatments
Corticosteroid drops and ointments
Doxycycline, minocycline
Lifitegrast ophthalmic solution 5% (Xiidra)
Lateral Canthal Crowding (a common cluster of comorbidities that includes dermatochalasis, entropion, trichiasis, and conjunctivochalasis.)
Treatments as noted elsewhere
Ocular Neuropathic Pain
Autologous serum tears
Pain medications
Scleral lenses
Gabapentin, pregabalin
Antidepressants
MGD
Antibiotic drops and ointments
Azithromycin ophthalmic (Azasite)
Expressing Meibomian glands
Heat (MiBoFlo®)
Heat and lid massage (LipiFlow®)
Intraductal Meibomian gland probing (Maskin® Probing)
Intense Pulsed Light (IPL)
Lid margin debridement (manual, Blephex)
Lid massage
LLLT photobiomodulation (low level light therapy)*
Other devices that apply heat and massage to eyelids
Stem cell therapy (currently experimental)
Heating lids with radio frequency waves generated by electrical currents*
TearCare*
Trichiasis
Epilation
Focus Group: Awareness and Education
One focus group considered research focused on raising awareness and educating patients, providers, and other stakeholder groups. Participants were asked to share their personal experience with patient or personnel training materials provided by treating physicians, pharmaceutical and medical device companies, government or regulatory agencies, medical-focused websites, or other sources where they have sought information on Dry Eye, MGD, or related comorbidities.
The focus group then brainstormed feasible ideas for improving awareness/education among the various stakeholder groups, and projects or research questions associated with these ideas ().
Discussion
Dry Eye/MGD patients, caregivers, patient advocates, clinicians managing Dry Eye and MGD cases, researchers, and other stakeholders convened to identify gaps in Dry Eye and MGD research. One prior study prioritizing aspects of Dry Eye research had almost no patient representation.Citation4 A second study solicited patient input,Citation5 but only from a list of priorities previously generated by clinicians.Citation6 In contrast, this convening incorporated the patient perspective from its inception through the preparation of this manuscript. We considered gaps in Dry Eye and MGD research and propose here research questions to fill those gaps. This extensive list of research questions can serve as a guide, or roadmap, for researchers considering the current status of Dry Eye and MGD care. Our overarching goal is to motivate independent researchers to undertake studies that incorporate Dry Eye and MGD patient-centered outcomes.
Over the course of two days, 16 participants, including 7 patients, 5 patient advocates, and 3 caregivers (some participants belonged to more than one group, eg, patient and patient advocate) identified gaps in research and produced ideas for research questions important to Dry Eye patients and stakeholder groups. During the convening held via Zoom, participants were assigned to focus groups that considered one of the following topics: comorbidities, factors contributing to disease and/or symptoms, diagnosis, patient questionnaires, disease definition and pathophysiology, physical and psycho-social impact of disease on patients, training/education, OTC and at-home treatments, and physician-prescribed treatments. Each group discussed the current state of research on that topic and potential research questions. One member of each focus group served as a scribe and another as a group leader and time keeper. Scribes shared their screens while taking notes in Microsoft Word, and notes were saved to a secure Google drive.
In total, the focus groups produced over 80 research questions that were compiled into a list, or proposed research roadmap ( and ). The expansive roadmap illustrates the many gaps in current research and offers a rich source of potential topics for future research important to improvement in patient care. The focus groups found that commonly used questionnaires did not appear to reliably identify patients with severe symptoms and did not capture the episodic nature of symptoms.Citation12,Citation13 One participant noted that even less-than-severe symptoms that last for a long time can be extremely debilitating, potentially leading to suicidal ideation, but the questionnaires do not provide a mechanism for the collection of information about this type of physical distress. Furthermore, because the questionnaires are often used in research studies, the groups expressed concern that countless Dry Eye and MGD-related studies may be flawed because they drew conclusions based on data collected from flawed questionnaires.
One focus group considered the definition of Dry Eye as proposed by the Tear Film and Ocular Surface society in its Dry Eye Workshop II (DEWS II) report:Citation14
Dry eye is a multifactorial disease of the ocular surface characterized by a loss of homeostasis of the tear film, and accompanied by ocular symptoms, in which tear film instability and hyperosmolarity, ocular surface inflammation and damage, and neurosensory abnormalities play etiological roles.
Although participants generally agreed that Dry Eye is multifactorial, they noted that hyperosmolarity is non-specific, and that patients may be asymptomatic. They recommended further work on the definition while also disagreeing with the focus on neurosensory abnormalities, noting that severe symptoms are to be expected in highly innervated and chronically irritated tissues.
Research questions for comorbidities, symptoms, and other factors contributing to Dry Eye and MGD, focused on allergies, ATD, blepharitis, and conjunctivochalasis individually as well as their comorbid effect on disease status. One focus group proposed a study to standardize ocular surface examinations so all comorbidities, including conjunctivochalasis, are evaluated and correctly diagnosed noting too often patients are not properly evaluated for many comorbidities, leading to diagnoses of ocular neuropathic pain. Other research question topics ranged from the roles of screen time and genetics to diet and inflammation on disease pathophysiology.
While brainstorming research questions about symptoms, participants noted the episodic nature of symptoms. Proposed research questions focused on the meaning of specific symptoms (which specific disease a symptom indicates), the incidence of common symptoms, and the value of identifying a specific underlying cause of pain and treating the underlying cause of the symptom versus treatment that focuses only on pain regardless of cause.
Regarding factors contributing to disease, screen time among adults and children, was a common theme. Additionally, participants suggested conducting research on factors that patients can control themselves, like diet, screen time, and nutritional supplements, versus genetics and aging, or previous exposure to toxins or particulate matter, which are not controllable by the patients.
In addition to research on questionnaires, on the topic of diagnosis, participants suggested research questions about the Schirmer’s test and other tests for ATD, meibography, and Meibomian gland probing as a diagnostic approach in addition to treatment of MGD. Participants suggested a study to determine why doctors do not look for root causes of disease and a related study regarding the best approach to diagnosing asymptomatic or occult disease.
On the topic of impact on patients and their loved ones, research questions focused on the psycho-social aspects of disease. One focus group proposed a primary study to determine the incidence and prevalence of suicidal ideation among patients with Dry Eye with a secondary study evaluating directionality between suicidal ideation and disease. A second focus group suggested evaluating the association of patient outcomes with participation in peer support groups, professional counseling, and with psychological support as a control.
Over-the-counter or at home treatments topics focused on efficacy and included lubricating drops, warm compresses, moisture chamber goggles, lid and lash hygiene, topical allergy drops, supportive nutritional therapy, alcohol and coffee consumption, night-time treatments, and blinking exercises. Similarly, physician-prescribed treatment topics focused on efficacy of punctal plugs, punctal cautery, topical anti-inflammatory drops, a range of treatments for MGD, and several studies to evaluate Meibomian gland probing methods.
One focus group proposed research studies for raising awareness of disease and improving patient and physician education. The group suggested a study to evaluate cost-effectiveness of treatments and various payment models to improve access to care as well as a study to determine if primary care physician awareness of Dry Eye and MGD causes and treatments can improve patient outcomes.
There was general consensus among all participants that the term Dry Eye is wholly inadequate in describing a disease that can have devastating impacts. To illustrate the potential magnitude of the impact of Dry Eye, MGD, and comorbidities, patients expanded on a list 30 emotions or behaviors displayed by Dry Eye patients bringing the total to 64. The patients noted that had they had more than the one-hour allotted time to expand on the list, it would have become even longer. We present the list here to underscore the importance of the research topics suggested by participants (. Impact).
Overwhelmingly, stakeholders attending the convening and those who served as non-attendee reviewers expressed strong support for the project in post-convening surveys. Of particular note was a comment about increased awareness of the impact disease may have on patients, particularly in severe symptomatic cases.
This study has several limitations. Although participants were instructed to consider research gaps, the views are limited to those individuals participating in the convening rather than a larger group if the project had been conducted as a survey. More participants may have emphasized different research gaps and proposed different studies to address those gaps. However, research questions proposed by participants were not ranked or prioritized to minimize the potential for bias. Moreover, only 1.5 hours was allotted for each focus group session. More allotted time may have yielded additional questions.
Finally, because patient questionnaires underpin clinical and research activities and this convening revealed the potential inadequacies of two commonly used questionnaires, development of reliable and meaningful Dry Eye and MGD symptom and severity questionnaires may rise in priority.
Conclusion
Over the course of two days, Dry Eye and MGD patients, clinicians and others representing various stakeholder groups met virtually via Zoom to assess gaps in Dry Eye and MGD research and develop a list of research questions to fill those gaps with the aim of improving the care Dry Eye and MGD patients receive. Participants received training in Dry Eye and MGD prior to the meeting in the form of a guidebookCitation11 that included information about Dry Eye, MGD, and related comorbidities and questions designed to help participants recall their experiences via reflection, individual brainstorming, or other grounding methods. The participants also reviewed four PCORI on-line modulesCitation7–10 about research methods and the benefits of conducting clinical comparative effectiveness research that includes patient-centered outcomes. During the meeting, participants were divided into smaller focus groups where they discussed topics and brainstormed research questions. The research questions were recorded and compiled into a research roadmap ( and ) that can serve as a source of inspiration to independent researchers interested in conducting research in Dry Eye, MGD, and related topics. Participants identified over 80 research questions and noted that incorporating a better understanding of the patient experience with disease and developing less biased and more accurate questionnaires or other symptom and status assessment tools may rise in priority as these provide the raw data that underpins the clinician’s practice and drives the Dry Eye and MGD industry and research.
Ethics Approval and Informed Consent
This research has received a “Not Human Research Determination” from the Institutional Review Board at the University of Central Florida.
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Disclosure
All authors received honoraria from PCORI for their participation in this work. Natalia A. Warren, Diana Adelman, Deidre A. Rector, and Claire Toland reported receiving additional financial support for their extended contributions. Dr. Steven L. Maskin reported owning >5% of MGDinnovations, Inc, a corporation receiving patent-based royalties (patent numbers: 9510844, 10159599, and 11110003) from a licensing agreement with Katena Products. The authors report no other conflicts of interest in this work.
Acknowledgments
The authors acknowledge members of the Stakeholder Advisory Council who generously contributed their insights and expertise to this project. Special appreciation is extended to Roger Azevedo for his contributions to the refinement of this manuscript.
This project was funded through a Patient-Centered Outcomes Research Institute (PCORI) Eugene Washington PCORI Engagement Award [EASCS-23147].
The views, statements, and opinions presented in this work are solely the responsibility of the author(s) and do not necessarily represent the views of the Patient-Centered Outcomes Research Institute® (PCORI®), its Board of Governors, or Methodology Committee.
Natalia A. Warren, Diana Adelman, Susan Howell; John McAree; Ruthie Dibble; Celia Carlisano; David P. Maconi are patient authors for this study. Deidre A. Rector and Theresa Carlisano are caregiver authors for this study.
References
- Lemp MA, Crews LA, Bron AJ, Foulks GN, Sullivan BD. Distribution of aqueous-deficient and evaporative dry eye in a clinic-based patient cohort: a retrospective study. Cornea. 2012;31(5):472–478. doi:10.1097/ICO.0b013e318225415a
- Stapleton F, Alves M, Bunya VY, et al. TFOS DEWS II Epidemiology Report. Ocular Surf. 2017;15(3):334–365.
- Maskin SL, Warren NA. Your Dry Eye Mystery Solved: Reversing Meibomian Gland Dysfunction, Restoring Hope. Yale University Press; 2022.
- Saldanha IJ, Le JT, Solomon SD, et al. Choosing Core outcomes for use in clinical trials in ophthalmology: perspectives from three ophthalmology outcomes working groups. Ophthalmology. 2019;126(1):6–9. doi:10.1016/j.ophtha.2018.09.008
- Saldanha IJ, Petris R, Han G, Dickersin K, Akpek EK. Research questions and outcomes prioritized by patients with dry eye. JAMA Ophthalmol. 2018;136(10):1170–1179. doi:10.1001/jamaophthalmol.2018.3352
- Saldanha IJ, Dickersin K, Hutfless ST, Akpek EK. Gaps in current knowledge and priorities for future research in dry eye. Cornea. 2017;36(12):1584. doi:10.1097/ICO.0000000000001350
- The PCORI Approach to patient-centered outcomes research. Available from: https://www.pcori.org/engagement/research-fundamentals/pcoriapproach-pcor. Accessed September 12, 2021
- Engaging in stakeholder-driven research. Available from: https://www.pcori.org/engagement/researchfundamentals/engaging-stakeholder-driven-research. Accessed September 12, 2021.
- Developing Research Questions. Available from: https://www.pcori.org/engagement/researchfundamentals/developing-research-questions. Accessed September 12, 2021.
- Designing the Research Study. Available from: https://www.pcori.org/engagement/researchfundamentals/designing-research-study. Accessed September 12, 2021.
- Warren NA, Rector DA. Guidebook. Engaging stakeholders to develop a roadmap for dry eye and MGD PCORI-funded research; 2022.
- Dougherty B E, Nichols J J, Nichols K K. Rasch analysis of the ocular surface disease index (OSDI). Investigative ophthalmology & visual science. 2011;52(12):8630–8635.
- Pucker A D, et al. Psychometric analysis of the SPEED questionnaire and CLDEQ-8. Investigative ophthalmology & visual science. 2018;59(8):3307–3313.
- Craig JP, Nichols KK, Akpek EK, et al. TFOS DEWS II definition and classification report. Ocul Surf. 2017;15(3):276–283. doi:10.1016/j.jtos.2017.05.008
- Nelson JD, Craig JP, Akpek EK, et al. TFOS DEWS II Introduction. Ocul Surf. 2017;15(3):269–275. doi:10.1016/j.jtos.2017.05.005
- Table of Contents. Ocular Surf. 2017;15(3):i–ii.
- Restasis Multidose TV Spot, Reduced Tear Production iSpot.Tv 2017 Available from: www.ispot.tv/ad/wqnV/restasis-multidose-reduced-tear-production. Accessed 23 April, 2024.
