Abstract
Trastuzumab deruxtecan (DS-8201) is an antibody–drug conjugate composed of a humanized monoclonal anti-HER2 antibody, a cleavable tetrapeptide-based linker and a potent topoisomerase I inhibitor. The drug’s efficacy has been proven in HER2-positive breast and gastric cancers. The rate of HER2 positivity in biliary tract cancer (BTC) has been reported to be 5–20%, and case reports and clinical trials have suggested that HER2 inhibitors might be active in HER2-positive BTC. Here we describe the rationale and design of the phase II HERB trial that will evaluate the efficacy and safety of trastuzumab deruxtecan in patients with HER2-expressing unresectable or recurrent BTC. The primary end point will be the centrally assessed objective response rate in HER2-positive patients.
Plain language summary
Trastuzumab deruxtecan (DS-8201) is a new drug against HER2, a receptor on cell membranes that has sensitivity to targeted inhibitors. The drug’s efficacy has been proven in HER2-positive breast and gastric cancers. Some studies have suggested that HER2 inhibitors might be active in HER2-positive biliary tract cancers. This article describes the design of a new clinical trial. The HERB trial is designed to evaluate the efficacy and safety of trastuzumab deruxtecan in patients with HER2-expressing biliary tract cancers.
Clinical trial registration: JMA-IIA00423.
Biliary tract cancers (BTCs) include intrahepatic and extrahepatic cholangiocarcinoma, gallbladder cancer and cancer of the ampulla of Vater. Although the prevalence and mortality of BTC vary based on the primary site and geographical region, its incidence is increasing worldwide [Citation1]. Complete surgical resection is the gold-standard treatment modality, but only 10–40% of patients have resectable disease [Citation2]. Most patients with BTC present with locally advanced or metastatic disease and have poor prognoses, with 5-year survival rates of less than 5–10% [Citation3].
Chemotherapy is the standard-of-care for locally advanced or metastatic BTC, and cisplatin plus gemcitabine was established as the standard first-line regimen [Citation4]. The efficacy of second-line chemotherapy after progression with cisplatin plus gemcitabine is limited. Although the ABC-06 phase III trial showed a survival advantage with fluorouracil, leucovorin and oxaliplatin (FOLFOX) plus active symptom control (ASC) over ASC alone, FOLFOX plus ASC conferred a median overall survival (OS) of 6.2 months, median progression-free survival (PFS) of 4.0 months and objective response rate (ORR) of only 5% [Citation5]. Other second-line chemotherapy options include fluorouracil, leucovorin and irinotecan (FOLFIRI), but this is based on several small retrospective studies, and its efficacy is also modest [Citation6]. Recently, NIFTY, an open-label, randomized, phase IIb study, reported that liposomal irinotecan (nal-IRI) in combination with fluorouracil and leucovorin (5-FU/LV) significantly improved PFS compared with 5-FU/LV alone [Citation7], but nal-IRI has not been approved for BTC. Because oxaliplatin and irinotecan are not covered by insurance in Japan, S-1 (an oral fluoropyrimidine) is often used as an alternative based on the results of phase II trials that showed an ORR of 7.5–22.7% [Citation8–10].
Novel molecular targets such as FGFR2 fusions, IDH1 mutation and BRAFV600E mutation were found to be attractive for BTC in phase II or phase III trials, although EGFR-targeted therapies failed to demonstrate efficacy [Citation11]. Pemigatinib achieved an ORR of 35.5% in patients with BTC harboring FGFR2 fusions or rearrangements [Citation12], infigratinib achieved an ORR of 18.8% in FGFR2 fusions [Citation13], dabrafenib plus trametinib showed an ORR of 51% in BRAFV600E mutations [Citation14] and ivosidenib was superior to placebo in PFS in IDH1 mutations [Citation15]. While these are important discoveries, there are still issues to be addressed, such as resistance mechanisms and the need for effective biomarkers [Citation16].
HER2 is a tyrosine kinase transmembrane receptor, and its overexpression and gene amplification are involved in tumor growth and progression. HER2-targeted therapy is effective in treating advanced breast and gastric cancers [Citation17–25]. In BTC, HER2 overexpression and/or gene amplification have been reported in several studies, and the HER2 positivity rates in extrahepatic and intrahepatic cholangiocarcinoma are estimated to be 10–20% and 5%, respectively [Citation26–40]. Although lapatinib, a HER2-targeted dual tyrosine kinase inhibitor, did not show efficacy in small clinical trials for unselected BTC patients [Citation41,Citation42], responses were observed among HER2-positive BTC patients treated with trastuzumab, trastuzumab emtansine or neratinib in case reports and case series [Citation43–47], suggesting that HER2-targeted therapy might be effective in patients with HER2-positive BTC. Recently, the results of the BTC cohort of MyPathway, a nonrandomized, multicenter, open-label, phase IIa multiple basket study, were reported, showing an ORR of 23% in 39 HER2-positive patients treated with a dual anti-HER2 regimen, pertuzumab plus trastuzumab [Citation48].
Trastuzumab deruxtecan (DS-8201)
Trastuzumab deruxtecan (DS-8201) is an antibody–drug conjugate composed of a humanized monoclonal anti-HER2 antibody with the same amino acid sequence as trastuzumab, a cleavable tetrapeptide-based linker, and a potent topoisomerase I inhibitor as the cytotoxic drug (drug payload); it has a drug-to-antibody ratio of approximately 8:1. Although the linker is stable in plasma, it is selectively cleaved after internalization by lysosomal enzymes such as cathepsins, which are overexpressed in the tumor microenvironment, releasing the topoisomerase I inhibitor payload [Citation49]. The released payload has a bystander effect that readily crosses the cell membrane [Citation50], allowing for a potent cytotoxic effect on HER2-low-expressing tumors and those with heterogeneous HER2 expression, such as gastric cancer and BTC.
In a dose-escalation phase I trial in patients with advanced breast and gastric cancers, although the maximum tolerated dose of trastuzumab deruxtecan was not reached, the most likely recommended phase II dosing was selected to be 5.4 or 6.4 mg/kg, based on safety and activity [Citation51]. As for breast cancer, a subsequent dose-expansion phase I trial reported that trastuzumab deruxtecan had preliminary activity with an ORR of 59.5% in patients with advanced HER2-positive (immunohistochemistry [IHC] 3+ or IHC 2+/in situ hybridization [ISH]-positive) breast cancer previously treated with trastuzumab emtansine and a manageable safety profile [Citation52]. Another cohort of dose-escalation phase I trials in patients with breast cancer assessed the activity of trastuzumab deruxtecan against HER2-low-expressing tumors (IHC 1+ or IHC 2+/ISH negative) and showed an ORR of 37.0% in 54 patients [Citation53]. In a single-group multicenter phase II study that confirmed the efficacy of trastuzumab deruxtecan in patients with HER2-positive metastatic breast cancer previously treated with trastuzumab emtansine (DESTINY-Breast01), 184 patients received the recommended dose of 5.4 mg/kg, and 112 (60.9%) achieved an objective response; the median response duration was 14.8 months and the median PFS was 16.4 months. The most common adverse events of grade 3 or higher were a decreased neutrophil count (20.7%), anemia (8.7%) and nausea (7.6%), but more attention should be paid to interstitial lung disease (2.7%, including 2.2% of grade 5 severity), an occasionally fatal adverse event [Citation21].
As for gastric cancer, in a dose-expansion phase I trial that assessed the safety and activity of trastuzumab deruxtecan in patients with advanced HER2-positive gastric cancer previously treated with trastuzumab, 19/44 patients (43.2%) had a confirmed objective response. In a subsequent randomized multicenter phase II study that evaluated trastuzumab deruxtecan at 6.4 mg/kg compared with chemotherapy in 187 patients with HER2-positive advanced gastric cancer who had progressed after receiving at least two previous regimens including trastuzumab (DESTINY-Gastric01), an ORR of 51% was achieved in the trastuzumab deruxtecan group, compared with 14% in the chemotherapy group (p < 0.001); the median OS times were 12.5 and 8.4 months, respectively (hazard ratio: 0.59; p = 0.01). Interstitial lung diseases were observed in 12 patients (9.6%), and the most common adverse events of grade 3 or higher in the deruxtecan group were decreased neutrophil count (51%), anemia (38%) and decreased white cell count (21%) [Citation25]. Based on this evidence, trastuzumab deruxtecan was approved for metastatic, HER2-positive breast and gastric cancer in the USA and Japan and for metastatic, HER2-positive breast cancer in the UK and the EU.
As for colorectal cancer, in a single-group multicenter phase II study, 24/53 (45.3%) patients with HER2-positive tumors achieved a confirmed objective response [Citation54]. For HER2-positive uterine carcinosarcoma, an investigator-initiated registration-directed phase II trial (UMIN000029506) is ongoing. In addition, in the aforementioned dose-expansion phase I trial, confirmed objective responses were observed in HER2-expressing (IHC ≥1+) non-small-cell lung cancer, salivary gland cancer, BTC and endometrial cancer [Citation55].
Collectively, these data suggest that trastuzumab deruxtecan has a potent HER2 inhibitory effect even after multiple treatments, including anti-HER2 therapy, activity in HER2-low-expressing tumors, and promising efficacy in many HER2-positive cancer types, including BTC. However, careful attention should be paid to the development of interstitial lung disease.
HERB trial
The HERB trial (NCCH1805, JMA-IIA00423), an investigator-initiated registration-directed trial funded by the Japan Agency for Medical Research and Development and Daiichi Sankyo, is being conducted to evaluate the efficacy and safety of trastuzumab deruxtecan in patients with HER2-expressing unresectable or recurrent BTC refractory or intolerant to treatment including gemcitabine. An investigator-initiated registration-directed trial means that the trial follows the Pharmaceuticals and Medical Devices Agency Act and Japanese good clinical practice for a new drug application [Citation56].
Objectives
The primary objective of this trial was to assess the benefit of trastuzumab deruxtecan on the ORR in HER2-positive (defined as IHC 3+ or IHC 2+/ISH+; ISH+ defined as HER2/chromosome 17 copy number ≥2.0) BTC patients by central imaging review. The secondary objectives included assessment of the following: ORR in all HER2-expressing patients by central imaging review, ORR in HER2-low-expressing (defined as IHC/ISH status of 0/+, 1+/−, 1+/+ or 2+/−) patients by central imaging review, ORR by local investigator review, disease control rate (DCR) by central imaging and local investigator review, PFS by central imaging and local investigator review, OS in two cohorts (HER2-positive and HER2-low-expressing) and the total population (all HER2-expressing) and incidence of adverse events. Exploratory objectives include investigating the pharmacokinetic profiles of trastuzumab deruxtecan, total antibody and MAAA-1181a (topoisomerase I inhibitor payload) in serum concentrations, estimating the incidence of human anti-human antibodies, assessing responses and survivals in registry data as an external control group, and performing ctDNA analyses.
Key eligibility criteria
The key inclusion and exclusion criteria are presented in . In this trial we enroll patients with unresectable or recurrent BTC histologically diagnosed as adenocarcinoma or adenosquamous carcinoma, with confirmed HER2 expression by central pathological examination, who were refractory to or intolerant of treatment including gemcitabine and have adequate organ function. Eligible patients have an Eastern Cooperative Oncology Group performance status of 0 or 1, are aged 20 years or older, have one or more measurable lesions and a left ventricular ejection fraction >50%. Patients with interstitial lung disease, pneumonitis requiring steroid therapy, or lung diseases that could not be ruled out by imaging during the screening period are excluded.
Table 1. Key inclusion and exclusion criteria in the HERB trial.
Study design
HERB is an open-label, single-group, multicenter, phase II trial (). Patients will be screened at 30 screening study sites in Japan, and eligible patients will be enrolled in the trial at five trial sites out of the 30 sites. The first patient was enrolled on 21 June 2019.
*The primary cohort (n = 24) of HER2-positive patients(defined as lHC 3+ or lHC 2+/lSH +) and the exploratory cohort (n = <8) of HER2-low-expressing patients (defined as lHC/lSH status of 0/+, 1+/-, 1+/+, or 2+/-).
BTC: Biliary tract cancer; ECOG PS: Eastern Cooperative Oncology Group performance status; HERB preSCR: Screening study of HER2 expression for biliary tract cancer; IHC: Immunohistochemistry; ISH: In situ hybridization; i.v.: Intravenous; SCRUM-Japan: Cancer Genome Screening Project for Individualized Medicine in Japan.
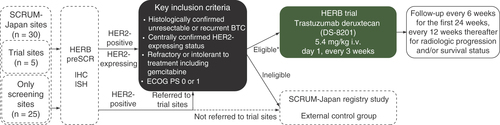
A screening study of HER2 expression for BTC (HERB preSCR, UMIN000036697) will be conducted to detect HER2-expressing BTC in the facilities of SCRUM-Japan, a nationwide cancer genome screening project in Japan. In this study, confirmation of HER2-expressing status will be obtained by central pathological examination using IHC and ISH on archival tissue. If HER2-positive BTC is detected at a site not conducting the trial, the patient will be referred to one of the five trial sites. HER2-positive patients not referred to the trial sites or who are ineligible for inclusion will be registered in the SCRUM-Japan registry study (UMIN000028058).
Patients will receive trastuzumab deruxtecan at a dose of 5.4 mg/kg, administered by intravenous infusion every 3 weeks. Study treatment will continue until radiological or clinical disease progression, unacceptable toxicity (including grade 2 or higher interstitial lung disease) or withdrawal of consent.
Evaluations
Tumor assessments using computed tomography (CT) scanning or MRI will be performed, based on the Response Evaluation Criteria in Solid Tumors version 1.1, by central imaging and local investigator review at weeks 6, 12, 18 and 24 and at every 12 weeks thereafter until radiological progression or the end of the study.
All toxicities experienced during the study will be recorded and graded according to the National Cancer Institute’s Common Terminology Criteria for Adverse Events version 5.0. Hematology and biochemistry monitoring will be performed at least once per treatment cycle and at the withdrawal visit before the initiation of sub-treatment. Chest CT for evaluating safety (i.e., assessing the development of interstitial lung disease) will be performed every 6 weeks. For cardiotoxicity assessment, echocardiography will be performed every four treatment cycles.
Mandatory plasma samples for ctDNA analysis will be collected at baseline, on day 1 of cycle 2 and at the withdrawal visit. In approximately six patients, serum will be collected for pharmacokinetic analysis at days 1, 8 and 15 of cycle 1 and day 1 of cycles 2, 3 and 4, and for human anti-human antibody analysis on days 1 and 8 of cycle 1 and day 1 of cycles 2 and 4, and at the withdrawal visit.
Statistical analysis methods
A total of 32 patients, including 24 with HER2-positive BTC and up to eight with HER2-low-expressing BTC, will be enrolled in this study. To analyze the ORR as the primary end point in patients with HER2-positive BTC, assuming a threshold response rate of 15% and an expected response rate of 40% with a one-sided significance level of α = 0.05 and β = 0.2 (80% power) for the entire study, the required number of patients is 22. The expected number of enrolled HER2-positive patients is 24, assuming that some patients are ineligible or receive no study treatment. In addition, up to eight patients (minimum six) with HER2-low-expressing BTC will be exploratively enrolled as eligible patients who will not be subject to the primary end point analysis. The purpose of this exploratory cohort is to explore whether signs of efficacy will be seen among HER2-low-expressing BTC patients.
All efficacy analyses will be performed for the full analysis set, defined as the population of all eligible patients, excluding those who receive no study treatment. Safety will be assessed for the safety analysis set, defined as the population of all registered patients, excluding those who receive no study treatment.
The binomial test will be performed for the null hypothesis of the true ORR in patients with HER2-positive BTC less than or equal to the threshold ORR of 15%. The 90 or 95% CIs for the ORR and DCR will be estimated using the Clopper and Pearson methods. The ORR is defined as the proportion of patients with a confirmed complete response or confirmed partial response as the best overall response, while the DCR is defined as the proportion of patients with a confirmed complete response or confirmed partial response and stable disease (confirmation requires at least 4 weeks of sustained effect) as the best overall response. PFS is defined as the time from the date of registration until disease progression or death from any cause or censor at the date of the last visit for patients without progression, and OS is defined as the time from the date of registration until death from any cause or censor or the final follow-up date for survivors. The median PFS and OS will be estimated using the Kaplan–Meier method, and the Brookmeyer and Crowley methods will be used to calculate the 95% CI. The probability of OS and PFS will be estimated using the Kaplan–Meier curve, and Greenwood’s formula will be used to calculate the 95% CI. The ORR, PFS and OS will also be estimated using the SCRUM-Japan registry data as an external control group.
Ethical considerations
The HERB trial is being conducted following the trial protocol approved by the institutional review boards of the participating institutions, with registration at JMA-IIA00423, and with the ethical principles of the Declaration of Helsinki, good clinical practice and applicable regulatory requirements. Informed consent will be obtained from all patients before enrollment in the study.
Discussion & future perspective
Although some benefit has been shown from standard regimens of FOLFOX or nal-IRI + 5-FU/LV (which demonstrated superiority of OS or PFS in a randomized trial) and alternative regimens of FOLFIRI or S-1 (which had modest activity in retrospective or phase II trials), the prognosis for patients with BTC who are refractory to cisplatin plus gemcitabine remains poor. For FOLFOX, the median OS was approximately 6 months, and the ORR was 5% [Citation5]. Thus more effective treatment strategies that improve response rates and extend survival in patients with BTC receiving second-line or later chemotherapy are needed.
Several molecular targets (e.g., FGFR2 fusion, IDH1 mutation and BRAFV600E) have been discovered in BTC, and targeted therapies for these have shown some efficacy [Citation12–15], but the prevalence of any of these genetic alterations is small: only a few percent. The rate of HER2 positivity in BTC has been reported to be 5–20%, which is relatively high, and case reports and clinical trials have suggested that HER2 inhibitors might be active in HER2-positive BTC as well as breast and gastric cancer [Citation48]. Based on the results of clinical trials to date, trastuzumab deruxtecan is more active than other existing HER2 inhibitors and has the characteristics of being effective in heavily treated and HER2-low-expressing cases [Citation21,Citation25,Citation52–54]. Against this background, trastuzumab deruxtecan is currently the most promising drug for HER2-expressing BTC, and the purpose of the HERB trial is to confirm whether trastuzumab deruxtecan is truly effective for HER2-positive BTC.
For this trial we established a HER2-expressing BTC screening study using the classical HER2 screening methods, IHC and ISH. Comprehensive genomic profiling (CGP) using tissue or blood samples is becoming the mainstream method to confirm HER2 amplification, but we noticed in our preliminary study that IHC and ISH have higher screening sensitivity than CGP using tissue samples (Ohba et al., [unpublished data]). Additionally, CGP reflects gene amplification, and classical screening methods such as IHC and ISH account for the cell membrane’s subsequent protein overexpression. Theoretically, the latter is more directly related to the drug efficacy, because trastuzumab deruxtecan binds to HER2 receptors on the cell membrane and is internalized in tumor cells. Because ctDNA will be measured in parallel in this study, the design allows us to compare the efficacy of the study treatment and the CGP findings using blood samples.
In terms of safety, interstitial lung disease is the most important adverse event associated with trastuzumab deruxtecan because of its potential fatality. Given that the gastrointestinal system mainly excretes this payload via bile, it is necessary to observe whether the frequency of interstitial lung disease increases in BTC with bile stasis and the subsequent increase in blood concentration due to bile duct obstruction. In this study the pharmacokinetics of trastuzumab deruxtecan will be analyzed for BTC.
In this study we set the threshold response rate at 15% and the expected response rate at 40%, which is exceptionally high, to show that this drug is more effective than any other existing cytotoxic drug or regimen. If this level of efficacy is demonstrated, it is expected that the mainstream secondary treatment for BTC will shift from cytotoxic therapy to molecular targeted therapy.
Immunotherapy with immune checkpoint inhibitors is emerging as a new treatment modality for BTC. Although the efficacy of immune checkpoint inhibitors as single agents is limited in BTC [Citation57,Citation58], several phase III trials of immune checkpoint inhibitors in combination with cisplatin plus gemcitabine as a first-line therapy are under way [Citation59,Citation60] In addition, there is growing interest in developing combinations of immunotherapy and molecularly targeted therapies for many cancer types. Therefore the combination of trastuzumab deruxtecan and immune checkpoint inhibitors is expected to be used in BTC. To supplement this rationale, we are observing the immune response during treatment with this drug as an extra-protocol study.
A limitation of this study is that it will be a cohort of a small number of Japanese patients. With a limited number of cases, there will be a risk of underestimating or overestimating the efficacy of the therapy. In addition, there are racial differences in the frequency of interstitial lung disease, meaning that the results should be interpreted with caution.
Taken together, this study has the potential to lead to the approval of a therapeutic agent for a novel target in BTC. If the agent is found to be highly effective, the treatment of BTC will not only move toward molecular targeted therapies, but also extend the approaches to first-line as well as second-line systemic therapy. Moreover, the combination of such agents with immunotherapy could bring dramatic advances to this area. In the future, it is envisioned that genuine precision medicine will be achieved in BTC.
Conclusion
The HERB trial will assess the benefit of trastuzumab deruxtecan in patients with HER2-positive unresectable or recurrent BTC. The results of HERB have the potential to enrich the treatment options in second-line settings or beyond and to improve the response and survival of these patients. The first report on the primary end point of the trial is expected in 2022.
Background
The prognosis for patients with biliary tract cancer (BTC) refractory to cisplatin plus gemcitabine remains poor, with a median overall survival (OS) of approximately 6 months and an objective response rate (ORR) of 5%.
The rate of HER2 positivity in BTC has been reported to be 5–20%, and case reports and clinical trials have suggested that HER2 inhibitors might be active in HER2-positive BTC.
Trastuzumab deruxtecan is an antibody–drug conjugate composed of a humanized monoclonal anti-HER2 antibody, a cleavable tetrapeptide-based linker and a potent topoisomerase I inhibitor; it is the most promising drug among the various HER2 inhibitors.
HERB trial
The multicenter, phase II HERB trial was designed to investigate the efficacy and safety of trastuzumab deruxtecan in patients with HER2-expressing unresectable or recurrent BTC who were refractory or intolerant to treatment including gemcitabine.
A total of 32 patients, including 24 with HER2-positive BTC and up to eight with HER2-low-expressing BTC, will be enrolled in this study.
Enrolled patients will receive trastuzumab deruxtecan at a 5.4 mg/kg dose, and this will be administered by intravenous infusion every 3 weeks.
The primary end point is the centrally assessed ORR in HER2-positive patients.
The secondary end points are ORR in all HER2-expressing patients, ORR in HER2-low-expressing patients, disease control rate, progression-free survival, OS and the incidence of adverse events.
Exploratory end points are the pharmacokinetics of trastuzumab deruxtecan, total antibody and drug payload; incidence of human anti-human antibodies; responses and survivals in registry data as an external control group; and serial ctDNA analyses.
The study had 80% power for the primary end point in HER2-positive BTC patients, with a one-sided α error of 5%, threshold ORR of 15% and expected ORR of 40%.
The first patient was enrolled on 21 June 2019, and the first report of the primary end point result is expected in 2022.
Financial & competing interests disclosure
The HERB trial is funded by Japan Agency for Medical Research and Development and Daiichi Sankyo. A Ohba has received research funding from Ono and Cugai, and honoraria from Yakult, Ono and Taiho. C Morizane has received research funding from Ono, Yakult, Eisai, J-Pharma, AstraZeneca, Merck and Daiichi Sankyo; honoraria from Yakult, Eisai, MSD, Teijin, Taiho and Novartis; and fees for advisory roles from Yakult, MSD, J-Pharma, AstraZeneca, Teijin, Taiho and Novartis. M Ueno has received research funding from Taiho, AstraZeneca, Merck, MSD, Daiichi Sankyo, Atrellas, Eisai, Ono, Dainippon Sumitomo, Incyte and Chugai, and honoraria from Taiho, AstraZeneca, Merck, MSD, Daiichi Sankyo, Servier, Ono and Chugai. S Kobayashi has received honoraria from Bayer, Chugai, Eli Lilly, Taiho, Takeda and Yakult, and fees for advisory roles from Bayer and GSK. Y Komatsu has received research funding from Taiho, Chugai, Bayer, Sanofi-aventis, Ono, MSD, Yakult, NanoCarrier, QuintilesIMS, SYSMEX, MEDISCIENCE PLANNING, Dainippon Sumitomo, Nippon Zoki, A2 Healthcare, Daiichi Sankyo, Eisai, Parexel International, Astellas, Incyte, Syneos health clinical, Shionogi and ShiftZero, and honoraria from Yakult, Mediscience Planning, Kyowa Kirin, Asahi Kasei, Daiichi Sankyo, Eli Lilly, Nipro, Bristol-Myers, Moroo, Pfizer, Merck, Medical Review, Mitsubishi Tanabe, Nippon Kayaku, Shire, Novartis, Otsuka and 3H Medi Solution. M Ikeda has received research funding from Merck, Eli Lilly, Yakult, Ono, ASLAN, J-Pharma, AstraZeneca, EA Pharma, Pfizer, Merus N.V., Servier, Delta-Fly, Chiome Bioscience, Chugai, Bristol-Myers Squibb, Novartis, Bayer and Takeda; honoraria from Eisai, MSD, Eli Lilly, Yakult, Teijin, Atrellas, Dainippon Sumitomo, Otsuka, Servier, Taiho, Chugai, Bristol-Myers Squibb, Novartis, Bayer and Takeda; and fees for advisory roles from Eisai, Eli Lilly, ASLAN, GSK, Servier, Chugai, Bristol-Myers Squibb, Novartis, Bayer and Takeda. N Okano has received honoraria from Taiho, Eli Lilly, Kyowa Kirin, Eisai, Bayer, Chugai, Takeda and Ono, and fees for advisory role from GSK. K Nakamura has received research funding from Daiichi Sankyo and honoraria from Taiho. C Nakamura has received research funding from Roche Diagnostics, Genomedia, Guardant Health, Chugai, Daiichi Sankyo, Taiho and Seagen. W Okamoto has received honoraria from Chugai, Bristol-Myers Squibb, Thermo Fisher, Taiho, Ono, Eli Lilly, Takeda and Novartis. T Yoshino has received research funding from Taiho, Dainippon Sumitomo, Ono, Chugai, Amgen, Parexel International, MSD, Daiichi Sankyo and Sanofi. T Okusaka has received research funding from Novartis, Pfizer, Ono, Kyowa Kirin, Dainippon Sumitomo, Eisai, Eli Lilly, AstraZeneca, Chugai, Bristol-Myers Squibb, MSD, Syneos Health, Nano Carrier, Baxter and Taiho; honoraria from AstraZeneca, AbbVie, Eisai, Ono, Yakult, Daiichi Sankyo, Taiho, Takeda, Chugai, Teijin, Eli Lilly, Servier and Novartis; and fees for advisory roles from AstraZeneca, Incyte, Eisai, Ono, Daiichi Sankyo, Takara, Takeda, Chugai, Eli Lilly, Servier, Novartis, Bayer, Pfizer, Bristol-Myers Squibb and Mundipharma. The authors have no other relevant affiliations or financial involvement with any organization or entity with a financial interest in or financial conflict with the subject matter or materials discussed in the manuscript apart from those disclosed.
No writing assistance was utilized in the production of this manuscript.
Ethical conduct of research
The HERB trial is being conducted following the trial protocol approved by the institutional review boards of the participating institutions, with registration at JMA-IIA00423, and with the ethical principles of the Declaration of Helsinki, good clinical practice and applicable regulatory requirements. Informed consent will be obtained from all patients before enrollment in the study.
Additional information
Funding
References
- Valle JW , KelleyRK, NerviB, OhDY, ZhuAX. Biliary tract cancer. Lancet397(10272), 428–444 (2021).
- Banales JM , CardinaleV, CarpinoGet al. Cholangiocarcinoma: current knowledge and future perspectives consensus statement from the European Network for the Study of Cholangiocarcinoma (ENS-CCA). Nat. Rev. Gastroenterol.13(5), 261–280 (2016).
- Razumilava N , GoresGJ. Cholangiocarcinoma. Lancet383(9935), 2168–2179 (2014).
- Valle J , WasanH, PalmerDHet al. Cisplatin plus gemcitabine versus gemcitabine for biliary tract cancer. N. Engl. J. Med.362(14), 1273–1281 (2010).
- Lamarca A , PalmerDH, WasanHSet al. Second-line FOLFOX chemotherapy versus active symptom control for advanced biliary tract cancer (ABC-06): a phase 3, open-label, randomised, controlled trial. Lancet Oncol.22(5), 690–701 (2021).
- Caparica R , LengeléA, BekoloW, HendliszA. FOLFIRI as second-line treatment of metastatic biliary tract cancer patients. Autops. Case Rep.9(2), e2019087 (2019).
- Yoo C , KimK, JeongJHet al. Liposomal irinotecan plus fluorouracil and leucovorin versus fluorouracil and leucovorin for metastatic biliary tract cancer after progression on gemcitabine plus cisplatin (NIFTY): a multicentre, open-label, randomised, phase 2b study. Lancet Oncol.22(11), 1560–1572 (2021).
- Sasaki T , IsayamaH, YashimaYet al. S-1 Monotherapy in patients with advanced biliary tract cancer. Oncology77(1), 71–74 (2009).
- Sasaki T , IsayamaH, NakaiYet al. Multicenter phase II study of S-1 monotherapy as second-line chemotherapy for advanced biliary tract cancer refractory to gemcitabine. Invest. New Drugs30(2), 708–713 (2012).
- Suzuki E , IkedaM, OkusakaTet al. A multicenter phase II study of S-1 for gemcitabine-refractory biliary tract cancer. Cancer Chemother. Pharmacol.71(5), 1141–1146 (2013).
- Rizzo A , FregaG, RicciADet al. Anti-EGFR monoclonal antibodies in advanced biliary tract cancer: a systematic review and meta-analysis. In Vivo34(2), 479–488 (2020).
- Abou-Alfa GK , SahaiV, HollebecqueAet al. Pemigatinib for previously treated, locally advanced or metastatic cholangiocarcinoma: a multicentre, open-label, phase 2 study. Lancet Oncol.21(5), 671–684 (2020).
- Javle M , LoweryM, ShroffRTet al. Phase II study of BGJ398 in patients with FGFR-altered advanced cholangiocarcinoma. J. Clin. Oncol.36(3), 276–282 (2017).
- Subbiah V , LassenU, ÉlezEet al. Dabrafenib plus trametinib in patients with BRAF V600E-mutated biliary tract cancer (ROAR): a phase 2, open-label, single-arm, multicentre basket trial. Lancet Oncol.21(9), 1234–1243 (2020).
- Abou-Alfa GK , MacarullaT, JavleMMet al. Ivosidenib in IDH1-mutant, chemotherapy-refractory cholangiocarcinoma (ClarIDHy): a multicentre, randomised, double-blind, placebo-controlled, phase 3 study. Lancet Oncol.21(6), 796–807 (2020).
- Rizzo A , RicciAD, BrandiG. Pemigatinib: hot topics behind the first approval of a targeted therapy in cholangiocarcinoma. Cancer Treat. Res. Commun.27, 100337 (2021).
- Baselga J , CortésJ, KimSBet al. Pertuzumab plus trastuzumab plus docetaxel for metastatic breast cancer. N. Engl. J. Med.366(2), 109–119 (2012).
- Swain SM , BaselgaJ, KimSBet al. Pertuzumab, trastuzumab, and docetaxel in HER2-positive metastatic breast cancer. N. Engl. J. Med.372(8), 724–734 (2015).
- Verma S , MilesD, GianniLet al. Trastuzumab emtansine for HER2-positive advanced breast cancer. N. Engl. J. Med.367(19), 1783–1791 (2012).
- Geyer CE , ForsterJ, LindquistDet al. Lapatinib plus capecitabine for HER2-positive advanced breast cancer. N. Engl. J. Med.355(26), 2733–2743 (2006).
- Modi S , SauraC, YamashitaTet al. Trastuzumab deruxtecan in previously treated HER2-positive breast cancer. N. Engl. J. Med.382(7), 610–621 (2019).
- Murthy RK , LoiS, OkinesAet al. Tucatinib, trastuzumab, and capecitabine for HER2-positive metastatic breast cancer. N. Engl. J. Med.382(7), 597–609 (2019).
- Saura C , OliveiraM, FengYHet al. Neratinib plus capecitabine versus lapatinib plus capecitabine in HER2-positive metastatic breast cancer previously treated with ≥2 HER2-directed regimens: phase III NALA Trial. J. Clin. Oncol.38(27), 3138–3149 (2020).
- Bang YJ , CutsemEV, FeyereislovaAet al. Trastuzumab in combination with chemotherapy versus chemotherapy alone for treatment of HER2-positive advanced gastric or gastro-oesophageal junction cancer (ToGA): a phase 3, open-label, randomised controlled trial. Lancet376(9742), 687–697 (2010).
- Shitara K , BangYJ, IwasaSet al. Trastuzumab deruxtecan in previously treated HER2-positive gastric cancer. N. Engl. J. Med.382(25), 2419–2430 (2020).
- Ito Y , ItoY, TakedaTet al. Expression and clinical significance of the erbB family in intrahepatic cholangiocellular carcinoma. Pathol. Res. Pract.197(2), 95–101 (2001).
- Aishima S , TaguchiK, SugimachiK, ShimadaM, SugimachiK, TsuneyoshiM. c-erbB-2 and c-Met expression relates to cholangiocarcinogenesis and progression of intrahepatic cholangiocarcinoma. Histopathology40(3), 269–278 (2002).
- Ukita Y , KatoM, TeradaT. Gene amplification and mRNA and protein overexpression of c-erbB-2 (HER-2/neu) in human intrahepatic cholangiocarcinoma as detected by fluorescence in situ hybridization, in situ hybridization, and immunohistochemistry. J. Hepatol.36(6), 780–785 (2002).
- Puhalla H , WrbaF, KandiolerDet al. Expression of p21(Wafl/Cip1), p57(Kip2) and HER2/neu in patients with gallbladder cancer. Anticancer Res.27(3B), 1679–1684 (2007).
- Yoshikawa D , OjimaH, IwasakiMet al. Clinicopathological and prognostic significance of EGFR, VEGF, and HER2 expression in cholangiocarcinoma. Br. J. Cancer98(2), 418–425 (2008).
- Harder J , WaizO, OttoFet al. EGFR and HER2 expression in advanced biliary tract cancer. World J. Gastroenterol.15(36), 4511–4517 (2009).
- Shafizadeh N , GrenertJP, SahaiV, KakarS. Epidermal growth factor receptor and HER-2/neu status by immunohistochemistry and fluorescence in situ hybridization in adenocarcinomas of the biliary tree and gallbladder. Hum. Pathol.41(4), 485–492 (2010).
- Pignochino Y , SarottoI, Peraldo-NeiaCet al. Targeting EGFR/HER2 pathways enhances the antiproliferative effect of gemcitabine in biliary tract and gallbladder carcinomas. BMC Cancer10(1), 631 (2010).
- Toledo C , MatusCE, BarrazaXet al. Expression of HER2 and bradykinin B1 receptors in precursor lesions of gallbladder carcinoma. World J. Gastroenterol.18(11), 1208–1215 (2012).
- Roa I , ToroG, de SchalperK, AretxabalaX, de ChuriC, JavleM. Overexpression of the HER2/neu gene: a new therapeutic possibility for patients with advanced gallbladder cancer. Gastrointest. Cancer Res.7(2), 42–48 (2014).
- Kawamoto T , IshigeK, ThomasMet al. Overexpression and gene amplification of EGFR, HER2, and HER3 in biliary tract carcinomas, and the possibility for therapy with the HER2-targeting antibody pertuzumab. J. Gastroenterol.50(4), 467–479 (2015).
- Hechtman JF , LiuW, SadowskaJet al. Sequencing of 279 cancer genes in ampullary carcinoma reveals trends relating to histologic subtypes and frequent amplification and overexpression of ERBB2 (HER2). Modern Pathol.28(8), 1123–1129 (2015).
- Javle M , Bekaii-SaabT, JainAet al. Biliary cancer: utility of next-generation sequencing for clinical management. Cancer122(24), 3838–3847 (2016).
- Yoshida H , ShimadaK, KosugeT, HiraokaN. A significant subgroup of resectable gallbladder cancer patients has an HER2 positive status. Virchows Arch.468(4), 431–439 (2016).
- Valle JW , LamarcaA, GoyalL, BarriusoJ, ZhuAX. New horizons for precision medicine in biliary tract cancers. Cancer Discov.7(9), 943–962 (2017).
- Ramanathan RK , BelaniCP, SinghDAet al. A phase II study of lapatinib in patients with advanced biliary tree and hepatocellular cancer. Cancer Chemother. Pharmacol.64(4), 777 (2009).
- Peck J , WeiL, ZalupskiM, O'NeilB, CaleroMV, Bekaii-SaabT. HER2/neu may not be an interesting target in biliary cancers: results of an early phase II study with lapatinib. Oncology82(3), 175–179 (2012).
- Law LY . Dramatic response to trastuzumab and paclitaxel in a patient with human epidermal growth factor receptor 2-positive metastatic cholangiocarcinoma. J. Clin. Oncol.30(27), e271–e273 (2012).
- Sorscher SS . Marked radiographic response of a HER-2-overexpressing biliary cancer to trastuzumab. Cancer Manag. Res.6, 1–3 (2013).
- Nam AR , KimJW, ChaYet al. Therapeutic implication of HER2 in advanced biliary tract cancer. Oncotarget7(36), 58007–58021 (2016).
- Hyman DM , Piha-PaulSA, WonHet al. HER kinase inhibition in patients with HER2- and HER3-mutant cancers. Nature554(7691), 189–194 (2018).
- Mondaca S , RazaviP, XuCet al. Genomic characterization of ERBB2-driven biliary cancer and a case of response to ado-trastuzumab emtansine. JCO Precis. Oncol.3(3), 1–9 (2019).
- Javle M , BoradMJ, AzadNSet al. Pertuzumab and trastuzumab for HER2-positive, metastatic biliary tract cancer (MyPathway): a multicentre, open-label, phase 2a, multiple basket study. Lancet Oncol.22(9), 1290–1300 (2021).
- Ogitani Y , AidaT, HagiharaKet al. DS-8201a, A novel HER2-targeting ADC with a novel DNA topoisomerase I inhibitor, demonstrates a promising antitumor efficacy with differentiation from T-DM1. Clin. Cancer Res.22(20), 5097–5108 (2016).
- Ogitani Y , HagiharaK, OitateM, NaitoH, AgatsumaT. Bystander killing effect of DS-8201a, a novel anti-human epidermal growth factor receptor 2 antibody–drug conjugate, in tumors with human epidermal growth factor receptor 2 heterogeneity. Cancer Sci.107(7), 1039–1046 (2016).
- Doi T , ShitaraK, NaitoYet al. Safety, pharmacokinetics, and antitumour activity of trastuzumab deruxtecan (DS-8201), a HER2-targeting antibody–drug conjugate, in patients with advanced breast and gastric or gastro-oesophageal tumours: a phase 1 dose-escalation study. Lancet Oncol.18(11), 1512–1522 (2017).
- Tamura K , TsurutaniJ, TakahashiSet al. Trastuzumab deruxtecan (DS-8201a) in patients with advanced HER2-positive breast cancer previously treated with trastuzumab emtansine: a dose-expansion, phase 1 study. Lancet Oncol.20(6), 816–826 (2019).
- Modi S , ParkH, MurthyRKet al. Antitumor activity and safety of trastuzumab deruxtecan in patients with HER2-low–expressing advanced breast cancer: results from a phase Ib study. J. Clin. Oncol.38(17), 1887–1896 (2020).
- Siena S , BartolomeoMD, RaghavKet al. Trastuzumab deruxtecan (DS-8201) in patients with HER2-expressing metastatic colorectal cancer (DESTINY-CRC01): a multicentre, open-label, phase 2 trial. Lancet Oncol.22(6), 779–789 (2021).
- Tsurutani J , IwataH, KropIet al. Targeting HER2 with trastuzumab deruxtecan: a dose-expansion, phase I study in multiple advanced solid tumors. Cancer Discov.10(5), 688–701 (2020).
- Nakamura K , ShibataT. Regulatory changes after the enforcement of the new Clinical Trials Act in Japan. Jpn. J. Clin. Oncol.50(4), 399–404 (2020).
- Ueno M , IkedaM, MorizaneCet al. Nivolumab alone or in combination with cisplatin plus gemcitabine in Japanese patients with unresectable or recurrent biliary tract cancer: a non-randomised, multicentre, open-label, phase 1 study. Lancet Gastroenterol. Hepatol.4(8), 611–621 (2019).
- Piha-Paul SA , OhD, UenoMet al. Efficacy and safety of pembrolizumab for the treatment of advanced biliary cancer: results from the KEYNOTE-158 and KEYNOTE-028 studies. Int. J. Cancer147(8), 2190–2198 (2020).
- Clinical Trials.gov . Durvalumab or placebo in combination with gemcitabine/cisplatin in patients with 1st line advanced biliary tract cancer (TOPAZ-1) (TOPAZ-1) (2022). https://clinicaltrials.gov/ct2/show/NCT03875235
- Clinical Trials.gov . Pembrolizumab (MK-3475) plus gemcitabine/cisplatin versus placebo plus gemcitabine/cisplatin for first-line advanced and/or unresectable biliary tract carcinoma (BTC) (MK-3475-966/KEYNOTE-966) (KEYNOTE-966) (2021). https://clinicaltrials.gov/ct2/show/NCT04003636
