Abstract
Objective: To report a case of recurrent unilateral presumed ocular toxocariasis after treatment of hepatitis C. Design: Case study. Methods: Clinical findings, ultrasonography, computed tomography, and serological tests were performed. Once diagnosis was made, effective treatment was administered.
Results: A 46-year-old woman with a long history of decreased unilateral visual acuity presented with anterior uveitis after the use of interferon alpha and ribavirin for treatment of hepatitis C. A biomicroscopic examination revealed active anterior uveitis, with ultrasonography and computed tomography demonstrating a central granuloma due to partially calcified toxocariasis. After treatment with corticosteroids and cycloplegics, the symptoms were alleviated. Conclusion: immunostimulation could cause a relapse of the inflammatory reaction found in uveitis due to toxocariasis.
Ocular toxocariasis involving the posterior segment is commonly presented in four forms: mobile subretinal larvae, diffuse unilateral subacute neuroretinitis (DUSN), chronic endophthalmitis, and retinal granuloma.Citation1 The most frequent subtypes are peripheral or polar granulomas.Citation2 In this case study, we describe a possible reactivation of toxocariasis, which initially presented as unilateral posterior-pole granuloma. After the use of interferon alpha and ribavirin for treatment of hepatitis C, the patient developed anterior uveitis and choroidal detachment.
A 46-year-old black woman reported ocular pain and hyperemia of the right eye for 20 days. She had a history of poor vision in this eye for 30 years. The patient began treatment for hepatitis C 3 months prior to her visit with a weekly use of interferon alpha and ribavirin. She had tested negative for co-infections, such as HIV or hepatitis B.
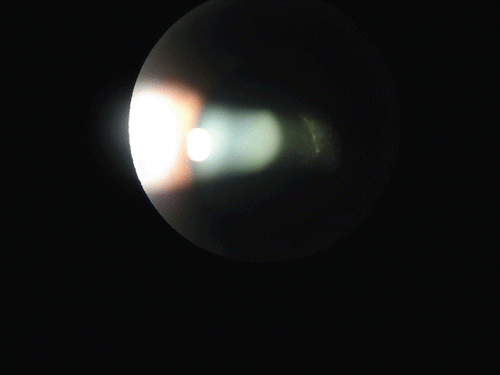
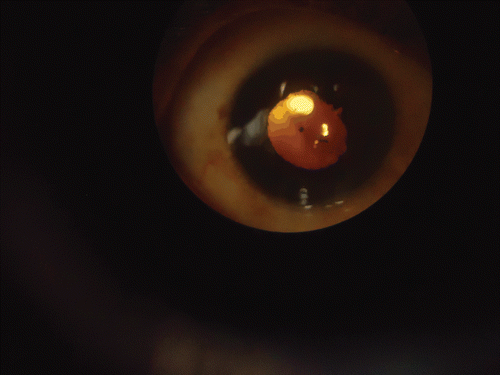
Examination of the eye revealed diminished visual acuity that improved with correction. Biomicroscopy of the anterior segment of the eye revealed cells and +2/+4 positive flares, iridolenticular synechiae, and +2/+4 posterior subcapsular cataracts ( and ). The patient presented with an intraocular pressure of 12.0 mmHg. Indirect ophthalmoscopic evaluation revealed the presence of extensive choroidal detachment () and extensive retinal fibrosis, which limited observation of the posterior pole.
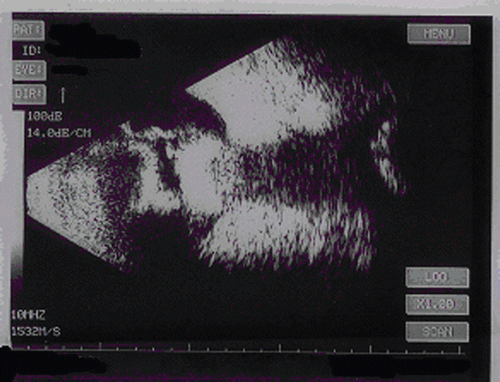
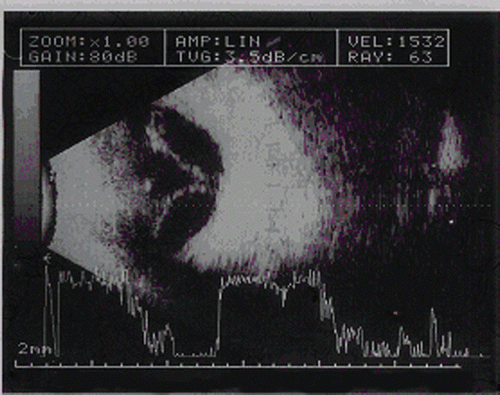
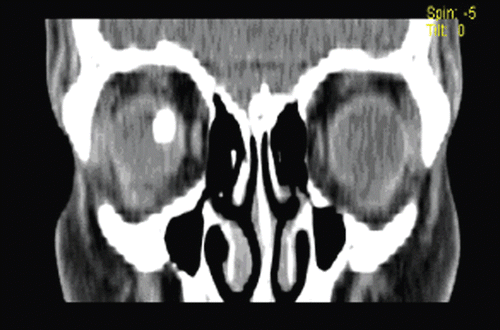
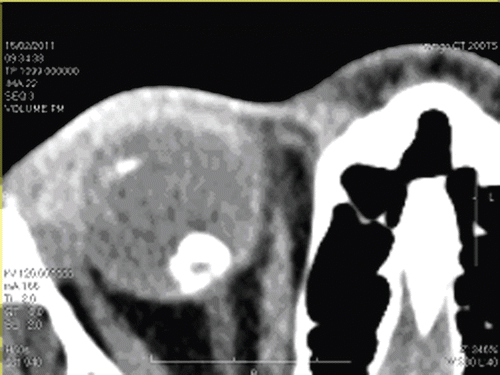
Under ultrasonography, a granuloma measuring 4.5 mm at its base and 7.8 mm in height with high echogenicity was observed over the optic disk. Choroidal detachment with mild vitritis and tractional retinal detachment were also observed ( and ). Sagittal and coronal computed tomography of the orbit revealed a rounded, partially calcified lesion along the posterior aspect of the ocular sphere and points of calcification of the ciliary bodyin the same eye ( and ). Immunological study with ELISA revealed plasma serology that was positive for Toxocara sp., with an IgG titer of 1:32. Blood eosinophil count was normal. Screening of the feces for parasites was negative, and serology for toxoplasmosis was negative for both IgG and IgM. The PPD test showed hypoactivity. In addition, tests such as VDRL and FTA ABS were negative. Finally, the patient’s chest radiograph was normal. Despite the immunological positive test for Toxocara, a presumed ocular toxocariasis could be considered more appropriate as a diagnosis, due to the lack of direct samples of the parasite.
DISCUSSION
Relapses of inflammatory processes due to interferon usage are not commonly related to infectious uveitis. The pathophysiological mechanism to explain the relapse of inflammatory process is not well known. It could be based on a possible process of Toxocara protein reconcilement through alpha interferon immunostimulation. Similar cases have been described with VKH uveitis and α-INF interactions.Citation3,Citation4
The rapid control of the inflammatory process with corticosteroids and aspects of the formation of choroidal detachment led us to consider the possibility of the relapse of anterior uveitis due to the reactivation of a toxocariasis. However, the coincidental effect cannot be ruled out as one of the differential diagnoses. The patient’s anterior uveitis was treated with cycloplegics, topical corticoids, and subtenon triamcinolone acetonide. There was successful control of the inflammation and ocular pain and a reduction of the choroidal detachment. The patient remains under observation with periodic ocular ultrasonographic and biomicroscopic evaluations. Treatment of hepatitis C was suspended, as suggested by experts at the hepatology clinic.
Declaration of interest: The authors report no conflicts of interest. The authors alone are responsible for the content and writing of the paper.
REFERENCES
- Shields JA. Ocular toxocariasi: a review. Surv Ophthalmol, 1984;28:361–368.
- Stewart JM, Cubillan LDP, Cunningham ET. Prevalence, clinical features and features and causes of visual loss among patients with ocular toxocariasis. Retina. 2005;25: 1005–1013.
- Soma M, Hirata A, Takahashi T, Okinami S. Relapse of Vogt-Koyanagi-Harada disease during interferon-α and ribavirin therapy in a case of chronic viral hepatitis C: case report. Ophthalmology. 2011 Jan 7;2(1):5–9.
- Al-Muammar AM, Al-Mudhaiyan TM, Al Otaibi M, Abdo A, Abu El-Asrar AM. Vogt-Koyanagi-Harada disease occurring during interferon-alpha and ribavirin therapy for chronic hepatitis C virus infection. Int Ophthalmol. 2010 Oct;30(5):611–613. Epub 2010 Feb 23.