The Problem
Overall, childhood immunizations rates are improving throughout the country,Citation1 which suggests current healthcare policies regarding childhood immunization are generally effective. However, children from 'hard to reach' groups require alternative approaches from the relevant healthcare professionals to enable immunization to occur.
People from the ‘hard to reach’ groups include members of the transient population, those with a lack of trust of healthcare professionals and of vaccines, those with low literacy levels or a lack of understanding about immunization and those experiencing cultural barriers. The UK National Institute of Clinical Excellence (NICE) has produced guidelines identifying those children most at risk of non-immunization ().Citation2
An example is the uptake rates for MMR immunization in recent years. There is some evidence that uptake of the MMR immunization has declined at a greater rate among children of more highly educated parents and among those living in more affluent areas.Citation6 Pearce et al. (2008) found that maternal education to degree level was a risk factor for not receiving the MMR triple vaccine.Citation7
Understanding the reasons a child does not attend clinic to receive immunization is crucial to finding the correct approach to achieve immunization. Parents may be experiencing a range of difficulties which result in immunization being a low priority for them. These may include language and cultural difficulties leading to misunderstanding of, for example, appointment times and the immunizations required, acute crises within the family that cause routine events to be reprioritized, the logistical difficulties of reaching the clinic with a large family, especially if they are a lone parent, or specific needs of the child which make immunization more difficult, e.g., autism or disability. Very few parents refuse immunization for their child when time is spent speaking to the parents in a one-to-one situation by specialist immunization nurses or health visitors for example, who may know the children and where there may be a trusting relationship already developed). This approach is costly but NICE guidelines state that it is cost effective to undertake a targeted model.Citation2
Who has Responsibility?
Health visitors (HVs) have the lead role in the delivery of the Healthy Child program, which means the health visiting team is responsible for working with parents and families to ensure children aged less than five years are offered, and are able to receive, all vaccinations as specified in the immunization schedule. There are a number of reasons why at risk groups are not being reached, including a lack of effective commissioning, parents wrongly perceiving the risk of the vaccines and a misconception by some health professionals that it is ‘not my responsibility’. In addition, HVs have heavy workloads; consequently they need to think innovatively about management of the process so as to ensure immunization is a priority for these hard to reach groups. This does not mean that they have to immunize children themselves but rather work with appropriate health professionals to ensure that immunization is offered at a time and place that is convenient for the parent and child even if this is within the home setting.
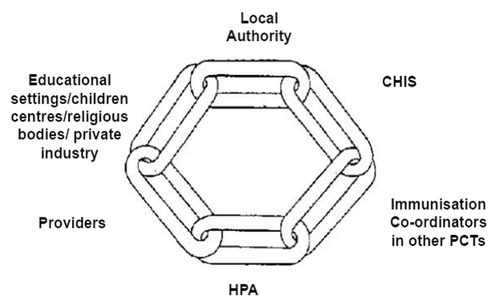
There are a number of key partners responsible for ensuring childhood immunization reaches all areas of society. details the agencies involved in this process. Reflecting this, the Department of Health states that “It is often easier to reach vulnerable groups and different communities by adopting a flexible approach to delivering services.”Citation8
The imminent changes to the NHS, which include the abolition of Primary Care Trusts and the changes in the immunization coordinators’ role, have the potential to disrupt the upward trend of childhood immunization rates. However, the need to continue improving rates and targeting hard to reach groups has been recognized by the UK Department of Health. The job description for the immunization/screening managers’ role devised by Public Health England states that they are required to:Citation8 “Establish links with relevant service user groups to elicit user feedback on commissioned services as required and in particular from vulnerable population groups such as travellers and offenders.” In addition the job description for the immunisation/screening co-ordinators’ role states that: “… monitor uptake and identify inequalities in screening and immunisation programme uptake particularly in relation to social class, ethnicity, special need, and develop and implement plans to reduce inequality and ensure that the unregistered (as well as the registered) population have access to high quality national screening and immunisation programmes.”
The Way Forward
NICE guidelines state that: ‘… economic modeling suggested that home visits (likely to be the most expensive means of increasing coverage by one percentage point) would be a cost effective use of NHS resources. The implication is that almost any method of increasing coverage would be cost effective’.Citation2
There are a number of steps that can be taken to help in reducing the number of unimmunized children. First, it is important for healthcare providers (HCPs) to have knowledge of the unimmunized population; this will enable them to offer appropriate access to services so they can then tailor information to suit the recipient. HCPs can provide opportunistic immunizations, recognize the importance of accurate documentation and create strong links with stakeholders. All these steps will be facilitated by a well informed and trained workforce.
The following are some examples of immunization initiatives undertaken within Central Lancashire PCT (in the UK), showing effective partnership working in action:
A bespoke HCP team worked with the Local Authority Gypsy/ Roma representative to immunize children on the local Gypsy/Roma traveler site.
HCPs worked with a local “Sure Start” center and its support workers to encourage parents of children with outstanding immunizations to attend a session in the center. The centers have Ofsted visits and are required to provide information of immunization uptake within the center’s catchment area.
Working in alliance with a local supermarket and a local radio station to put on an immunization session using the radio station’s mobile bus was organized within the supermarket car park during the school holidays.
There are many more such initiatives that are undertaken across the country. It is important that HCPs understand that it is not as a case of expecting the parent to come at a time to suit the HCP but rather the HCP reaching out to the parents and children and making it easier for them. If the implementation program is performed by a well-trained, knowledgeable and enthusiastic workforce then high immunization rates can be achieved.
Is it Worth it?
Immunization of children, including those in hard to reach groups, helps protect them from disease; it also protects the wider population and reduces hospital admissions. The approach outlined here, of reaching out to identified risk groups, helps build parental confidence not only with immunization but also with other health services. It also builds relationships between health professionals and other stakeholders and agencies.
References
- Report HP. (HPA). Immunisation Weekly Report. March 2013;7(12). Available from URL: http://www.hpa.org.uk/hpr/infections/immunisation.htm#coverQ4 (Accessed March 2013).
- NICE public health guidance PH21 Reducing differences in the uptake of immunisations. Issued: September 2009. Available from URL: http://publications.nice.org.uk/reducing-differences-in-the-uptake-of-immunisations-ph21. (Accessed March 2013).
- Hill CM, Mather M, Goddard J. Cross sectional survey of meningococcal C immunisation in children looked after by local authorities and those living at home. BMJ 2003; 326:364 - 5; http://dx.doi.org/10.1136/bmj.326.7385.364; PMID: 12586668
- Peckham C, Bedford H. Towards better immunisation rates. Practitioner 1989; 233:1343 - 4; PMID: 2616499
- Samad L, Butler N, Peckham C, Bedford H, Millennium Cohort Study Child Health Group. Incomplete immunisation uptake in infancy: maternal reasons. Vaccine 2006; 24:6823 - 9; http://dx.doi.org/10.1016/j.vaccine.2006.06.039; PMID: 17050048
- Wright JA, Polack C. Understanding variation in measles-mumps-rubella immunization coverage--a population-based study. Eur J Public Health 2006; 16:137 - 42; http://dx.doi.org/10.1093/eurpub/cki194; PMID: 16207728
- Pearce A, Law C, Elliman D, Cole TJ, Bedford H, Millennium Cohort Study Child Health Group. Factors associated with uptake of measles, mumps, and rubella vaccine (MMR) and use of single antigen vaccines in a contemporary UK cohort: prospective cohort study. BMJ 2008; 336:754 - 7; http://dx.doi.org/10.1136/bmj.39489.590671.25; PMID: 18309964
- Vaccination services. reducing inequalities in uptake, Department of Health, 2005. Available from URL: http://www.dh.gov.uk/prod_consum_dh/groups/dh_digitalassets/@dh/@en/documents/digitalasset/dh_4108046.pdf (Accessed March 2013).