Abstract
In recent years, there has been an increase in the number of cases of certain immunopreventable diseases in our country. A high proportion of these have been recorded among the young adult population. The aim of this study was to determine the seroprevalence of antibodies against immunopreventable diseases with the greatest health impacts on the young adult population (19–39 y of age) in Madrid. We collected a total of 1,153 serum samples from healthy volunteers undergoing routine medical visits and used ELISA to determine the presence of IgG antibodies against measles, rubella, mumps, and varicella zoster, as well as Bordetella pertussis. The Pearson’s χ2 test was used to compare prevalences, the Mann-Whitney U test was used to compare means, and the Kruskal-Wallis test was applied for variables with more than 2 categories. Statistical significance was achieved with p values of < 0.05.
The global prevalence of antibodies was 92.1% for measles, 94.4% for rubella, 88.3% for mumps, 92.8% for varicella zoster, and 70.2% for B. pertussis. No statistically significant differences were found between genders. The prevalence of antibodies against measles was more than 95% in the group of individuals born after 1986, and the percentage of individuals susceptible to rubella was less than 5% in women born after 1986. In spite of adequate vaccination coverage, in our region, a population of young adults exists who have not achieved the objectives of the WHO for the elimination of measles and congenital rubella syndrome.
Introduction
Since 1998, the WHO has developed different successive plans for the elimination of measles, interrupt the transmission of mumps and control of congenital rubella infection in the European Region.Citation1,Citation2 To meet these objectives, it is essential to achieve vaccination coverage above 95% among susceptible groups and to establish surveillance systems that, among other things, permit the identification of groups that are at risk for these immunopreventable diseases.
In Madrid, routine immunisation against measles, mumps, and rubella (MMR) with a single dose at 15 mo of age was initiated in 1981. In 1996, the rubella vaccine, which was administered only to girls at 11 y of age, was substituted for a second dose of vaccine for both sexes. Subsequently, in 1999, this second dose was moved up to 4 y of age, and dosing was maintained at 11 y of age in a transient form for those not vaccinated at age 4. This dosing was enacted to raise the levels of immunity to measles and mumps to those proposed by the WHO for the elimination of indigenous measles and to gain control of mumps, rubella and rubella congenital syndrome in the European RegionCitation2-Citation4
In recent years and despite adequate vaccination programs, an increased number of cases of certain of these vaccine-preventable diseases, including measles, rubella and mumps, has been recorded in Madrid.Citation5,Citation6 Migratory movements from countries with low vaccination coverage rates, a lack of adherence of certain population groups to vaccination programmes, and the existence of cohorts of young adults who were not vaccinated or who lived where no adequate vaccination coverage was achieved during childhood have largely been responsible for this rise.Citation7,Citation8
With regard to surveillance systems, seroprevalence studies are notably useful because they allow the levels of protective immunity in a population to be investigated and therefore allow the planning and evaluation of immunisation programmes, as well as the identification of at-risk groups for whom such precautionary measures can be implemented.Citation9
To date, various seroprevalence surveys conducted both nationally and in MadridCitation10,Citation11 indicate that infection with the varicella-zoster virus (VZV) is acquired during infancy such that more than 90% of the population is seropositive for VZV by adolescence. Despite the low proportion of chickenpox cases in registered adults in our country, the severity of the clinical picture and the complications that occur, primarily in young adults, are high.Citation12
Pertussis is a pediatric disease caused by the bacterium B. pertussis that occurs in epidemic cycles and is notifiable. Although the incidence of pertussis in our country decreased significantly after the introduction of vaccination, in recent years, there has been an increase in the number of cases, both nationally and in Madrid, particularly in adolescents and young adults, which is most likely due to the limited duration of vaccine immunity.Citation2,Citation13 This phenomenon has caused these population groups to become the main reservoirs and sources of disease transmission to the susceptible population composed of children less than one year of age, for whom the risk of complications and mortality is higher.
Seroprevalence data for immunopreventable diseases that present the greatest health impacts for any age group have not been published in Spain in the past 10 y. Because the young adult population plays a fundamental role in the transmission of these diseases and because these infections used are more severe in this group of age, the aim of this study was to determine the prevalence of IgG antibodies against B. pertussis and the measles, mumps, rubella, and varicella-zoster viruses in the young adult population of Madrid.
Results
During the study period, serum samples were collected for 1,153 healthy volunteers with a mean age of 27.67 y (± 5.9); 82.3% of the volunteers were female, and 17.7% were male. Of these samples, a total of 1,129 serum samples for VZV, 1,147 for measles and mumps, and 1,153 for rubella and B. pertussis were viable for the seroprevalence study.
Global prevalences of 92.8% for IgG antibodies specific for VZV (CI 95%: 91.3–94.3), 92.1% (CI 95%: 90.5–93.7) for measles, 94.4% (CI 95%: 93.1–95.7) for rubella, 88.3% (CI 95%: 86.4–90.2) for mumps, and 70.2% (CI 95%: 67.6–72.8) for B. Pertussis were obtained.
There were no statistically significant gender differences in relation to the overall prevalence of antibodies against these pathogens ().
Table 1. Prevalence of antibodies against VZV, measles, rubella, mumps, and B. pertussis in the studied population
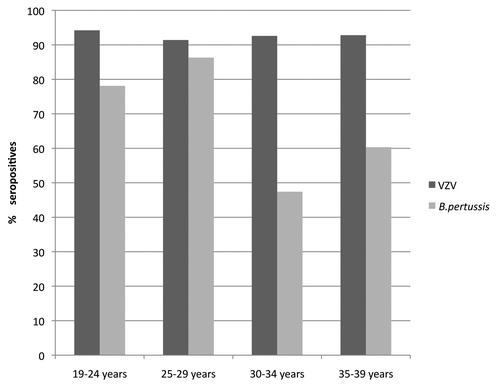
shows the numbers of individuals that were seroprevalent against VZV and B. pertussis by age. Significant differences (p < 0.001) were found between different age groups when comparing B. pertussis seropositivity, but this difference was not observed for VZV.
To analyze the results for measles, mumps, and rubella, these findings were grouped by age () and by cohort according to subject birth year () to allow for comparisons with other similar studies. To this end, figures were grouped into 3 different cohorts: percentages of seropositive individuals among those born before the year 1981 (period prior to initiation of MMR), between 1982–1986 (years with low vaccination coverage and less chance of contact with wild virus due to decreased circulation), and after 1986 (adequate vaccination coverage). Statistically significant differences were found between the different age groups for the prevalence of measles (p < 0.001) and mumps (p = 0.002). These differences persisted when the data were analyzed by cohort according to birth year (measles: p < 0.001; mumps: p = 0.026).
Figure 2. Percentage of individuals that are seropositive for measles, mumps, and rubella by age group (* includes indeterminate and positive results) (** women only).
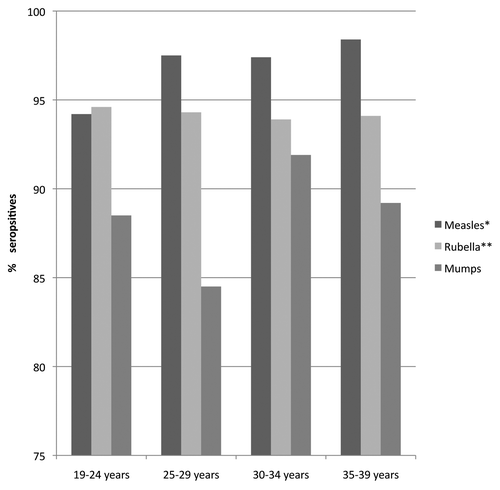
Figure 3. Percentage of individuals that are seropositive for measles, mumps, and rubella by cohort and year of birth (* includes indeterminate and positive results) (** women only).
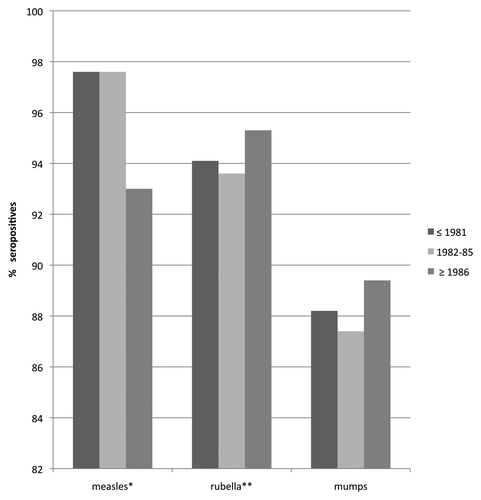
In the case of rubella, there were no statistically significant differences between different age groups or between the 3 cohorts with respect to gender.
A study of the correlation of the seroprevalence results for various diseases was conducted (data not shown) and demonstrated a statistically significant association between seronegativity for measles, mumps, and rubella. There was no correlation between the results for B. pertussis and VZV with these 3 viruses or with each other.
Discussion
Our results represent the biggest seroprevalence study performed in Spain among young adults since the national seroprevalence survey of 1996. The global prevalence of antibodies was 92.1% for measles, 94.4% for rubella, 88.3% for mumps, 92.8% for varicella zoster, and 70.2% for B. pertussis.
Measles
Of the serum samples tested for the presence of antibodies against the measles virus, 92.1% were found to be positive, 4.5% were classified as indeterminate, and 3.4% were negative. The Enzygnost ® Anti-Measles Virus/IgG ELISA test (Siemens) was used in this study. In the ESEN-2 study conducted in Europe,Citation14 in which the same ELISA test was used as a reference for all participating countries, it was proposed that indeterminate results obtained with this test be equated with positive results. Taking this finding into account, the overall seroprevalence data against measles in our study amounts to 96.6%.
To achieve an interruption in the transmission of measles in the European region, the WHO has estimated that the proportion of susceptible individuals should not exceed 5% for young adults aged 14 y and older.Citation1 The overall number of seronegative subjects in our study (3.4%) is in line with the WHO requirements for the young adult population.
However, when analyzing the cohort results according to birth year, the percentage of susceptible individuals exceeded 5% for the cohort born after the year 1986 (); this result was also confirmed in the group of subjects aged 19 to 24 y (). These numbers contrast with those obtained in the last seroprevalence study conducted in MadridCitation14 and are surprising, given that from 1985 and adequate vaccination coverage was achieved in our region when all children born after that date received 2 doses of MMR vaccine.Citation5,Citation16
In the last nationwide seroprevalence survey, high levels of susceptibility were also obtained in the cohort of individuals born after 1986.Citation17 In the year that study was completed, the participants from this cohort were between 6 and 9 y old and had not yet received their second dose of MMR vaccine. These characteristics would explain the percentage of susceptible individuals found in that survey but not ours.
To date, several seroepidemiological studies published in other European countries with vaccination coverages similar to ours also found percentages of susceptible individuals greater than 5% among those over 20 y of age.Citation14,Citation18,Citation19 One possible explanation for these findings could be the diminished immune response generated by vaccination compared with natural exposure to the virus and the consequent loss of immunity in these subjects because they had no opportunity for repeated contact with the virus as a result of the poor circulation of wild strains in the environment.Citation17,Citation18 More than 30% of reported cases in recent measles outbreaks in Madrid and the rest of the country were among persons over the age of 20, most of whom were unvaccinated.Citation8,Citation15 The data obtained in this study corroborate the fact that this continues to be the case in Madrid, which contains a population susceptible to the disease for whom tighter surveillance and prevention measures should be established.
Rubella
According to the WHO recommendations for the elimination of rubella and the prevention of congenital rubella syndrome in the European Region, it is necessary for the percentage of women of childbearing age who are susceptible to the virus to be less than 5%.Citation2
The overall prevalence of antibodies to rubella virus in our study was 94.4% (). For the results obtained with women, the level of susceptible individuals proposed by the WHO was only reached in the cohort of women born since 1986 (). These data contrast with those published in our country over the last decade,Citation15,Citation17,Citation20 in which the percentage of women who were seropositive for rubella exceeded 95% in all age groups.
As proposed in the ESEN-2 study,Citation14 indeterminate results in our work were not included with the positive results. However, antibody titers > 15 IU/ml were considered to be protective.Citation14,Citation21 Both of these considerations could justify the lower seroprevalence figures obtained in this study compared with other studies.
In the case of MMR vaccination, it has been described that in situations where there is no “natural” viral circulation, antibody titers decrease 15 y after vaccination, although this decrease is less pronounced for the rubella vaccine, which has a vaccine component that generates a higher immune response.Citation22 The seropositivity values found for the cohort of women born after 1986 agree with this supposition.
The highest recorded percentage of susceptibility was among women over 30 y of age (). These numbers could be explained by the inclusion of women in this age group who were never vaccinated and who, after the introduction of rubella vaccination in 1979, have had no contact with the wild virus due to its decreased circulation. Another possible explanation could be the geographical origin of these women. In recent years, there has been a significant increase in the immigrant population in Madrid, mainly consisting of people from Latin America.Citation15 Seroprevalence studies conducted in Spain among immigrant women of childbearing age have indicated that the percentage of subjects who are susceptible to rubella is high among this population, primarily among older women.Citation23,Citation24 Because our study was conducted with human volunteers, and data on their country of origin was unknown, we cannot ensure that these hypotheses fully explain the results obtained in this study.
The numbers for rubella susceptibility found in this study indicate that it is still necessary to maintain selective immunisation strategies among the population of women of childbearing age in the Madrid region to prevent disease outbreaks and cases of congenital rubella syndrome.
Mumps
Since the introduction of the MMR vaccine in the Spanish immunisation schedule in 1981 and despite adequate vaccination coverage, the reduction in the number of mumps cases has not been as pronounced as might be expected, with major outbreaks occurring during the last decade in Madrid and nationally.Citation5
Immunity to the mumps virus is complex and not always easy to interpret because although it is known that a high population seropositivity rate against the virus is an important factor in outbreak prevention, the baseline or minimal titer considered to be protective is unknown; therefore, seronegativity for the virus does not always equal susceptibility.Citation19,Citation25
The overall prevalence of antibodies against the mumps virus was 88.3% and did not reach 90% in any of the age groups (). As described elsewhere, these seropositivity figures are lower than those obtained for measles and rubella. These data could be interpreted as a loss of immunity against the mumps virus over time as a result of reduced immunogenicity induced by the mumps vaccine component of the MMR in relation to the other two components (measles and rubella).Citation17,Citation18,Citation20,Citation25 This finding could also, however, be due to the lower sensitivities of different EIA tests that are used to detect anti-mumps antibodies compared with those detecting antibodies to measles or rubella.Citation14,Citation18 The overall seroprevalence values for young adults are similar to those obtained in studies from Madrid, Catalonia, and other surrounding countries.Citation15,Citation20,Citation25,Citation26
In contrast to the data presented in the latest national seroprevalence survey,Citation11 the highest seropositivity rates were found among subjects born after 1986 (89.4%) in our work (). According to the immunisation schedule of Madrid, these individuals would have received at least 1 dose of Jeryl Lynn vaccine,Citation15 which appears to induce lower seroconversion compared with individuals who receive 2 doses of this strain.Citation17 However, due to the mumps outbreak recorded in Madrid in 2007, a population-based intervention was conducted in which those individuals who had not been vaccinated with 2 doses of the Jeryl Lynn, Urabe, or RIT 4385 vaccine strains were re-vaccinated.Citation5 Among these subjects were those born between January 1985 and December 1989 and who were between 19 and 22 y of age at that time. The year 2007 was also when we began collecting sera for this study. Therefore, this vaccination strategy could be reflected in this work, thus justifying the somewhat higher number of seropositive individuals in this cohort.
Interestingly, the response to the three components of MMR vaccine was shown to be different in our study. On the one hand, the percentage of rubella or mumps susceptible individuals was lower in the cohort born after the 1986, suggesting that better protection was reached after the introduction of vaccination due to the already mentioned higher immune response of the rubella component of MMR and to the revaccination with MMR after the mumps outbreak in Madrid. But this revaccination did not increase measles seroprevalence and the percentage of measles susceptible individuals was higher in the cohort born after the 1986. This can be explained not only by the better protection of the natural infection, but also to the high infectivity rate of measles combined with the difficulty to reach unvaccinated individuals in re-vaccination programs.
VZV
VZV is a disease of benign prognosis when acquired during childhood, but prognosis is complicated if it occurs during adulthood. Young adults have a higher risk of mortality and complications from this disease, which include is possible transmission to the fetus when infection is acquired during pregnancy.Citation27,Citation28
In 2005, the VZV vaccine for children 11 y old with no history of disease or previous vaccination was included in the immunisation schedule of Madrid to prevent the development of this disease in the age group most at risk for complications. A year later, a dose at 15 mo of age was introduced for those born in the region. Unlike Madrid, there are other regions in our country where vaccination against VZV is not systematically conducted; this diversity could favor circulation of wild virus in these areas and between different regions of the country, facilitating the infection of susceptible populations.Citation29
In our study, the total percentage of VZV seropositive subjects was 92.8%. This figure is somewhat lower than those reported in other seroprevalence studies, both nationally and in other autonomous communities.Citation11,Citation30 The serosurveillance survey conducted in Madrid between 1999 and 2000 revealed an immunity percentage between 95.8% and 97.4% for individuals aged 21 to 40 y.Citation10
One possible explanation for our result is the use of a less-sensitive diagnostic method compared with other techniques for detecting antibodies against VZV. In addition, there is a lack of a “gold standard” method for detecting anti-VZV IgG, which is why it is difficult to compare results between different studies.Citation31 Furthermore, and unlike other studies,Citation32 indeterminate results were not been included with positive results in this study, which is why the rates of seropositivity may be lower.
Pertussis
IgG antibodies to Bordetella pertussis were detected in 70.2% of the sera tested. These seropositivity numbers are similar to those reported in a study that was performed in Catalonia in 1996Citation33 but are significantly higher than those obtained in other studies conducted nationally.Citation34,Citation35
With regard to age distribution (), the group with a lower seroprevalence for B. pertussis consists of subjects between 30 and 34 y of age followed by an increase in those 35–39 y. This increase could be related to differences in the kinetics of PTCitation36or to the waning immune response observed 10 to 20 y after natural infection potentially occurring during adolescence, once protection of primary vaccination was lost.37The 25 to 29 age group displayed the highest seroprevalence figures. These data coincide with that described in several studies conducted in other countries.Citation36-Citation38 As was reflected in these studies, the peak seroprevalence in this age group could be indicative of a recent B. pertussis reinfection, thereby allowing this population to become an important potential reservoir and transmit the disease to children.
In reference to this point, our study has limitations: the ELISA test we used has good sensitivityCitation39 but, compared with those that only use purified pertussis toxin as antigen, this test is not linearly correlated with WHO standards, making it difficult to quantify antibody titers and therefore difficult to identify recently infected subjectsCitation39,Citation40 who would exhibit higher IgG titers.
Beginning in 2011, there were a significant number of cases among adolescentsCitation13 due to different pertussis outbreaks in Madrid and, consistent with vaccination strategies followed by other countries around us,Citation41 a sixth dose of acellular pertussis vaccine (Tdap) at 14 y of age was introduced into the childhood immunisation schedule in Madrid. The main objective of this strategy was to reduce morbidity and mortality in risk groups by reducing the transmission and recirculation of this microorganism.
This work was performed during the 2 y prior to the introduction of the sixth vaccine dose. Thus, the possible effects of the sixth dose on the seroprevalence of the disease would not be reflected in the current study. Future studies will be needed to determine a possible change in the seroprevalence of young adults, as well as a regional decrease in pertussis cases.
Limitations
The main limitation of the study is the use of a convenience sample of young healthy volunteers undergoing routine medical visits at a hospital in Madrid. As this cannot considered a random sample of Madrid population, extrapolation of the study findings to other settings require careful consideration.
Although more than 80% of our sample were women, gender differences in the studied diseases are not to be expected because seroprevalence is driven i) by the routine vaccination schedule ii) by natural infections. Gender differences in the seroprevalence status of young adults in Spain in the past were mainly attributed to the vaccination of males during the compulsory military service that ceased to be obligatory in 2001.
Patients and Methods
Study population
Serum samples from healthy volunteers between 19 and 39 y of age undergoing routine medical visits at Fuenlabrada University Hospital (Madrid), were collected between July 2007 and June 2010. Sera were stored at -20°C until different serological determinations were completed. For each sample, the date of collection, gender, and date of birth were recorded. Informed consent was obtained from each participant.
The study was approved by the Ethics Committee of the Fuenlabrada University Hospital and met the Harmonised Tripartite Guidelines for Good Clinical Practice (ICH/CPMP/135/95), local regulations (including the European Directive 2001/20/EC), and the ethical principles outlined in the Declaration of Helsinki.
Sample size
Given the young adult population (19–39 y) living in Madrid and the seroprevalences of the various immunopreventable diseases being studied, which range between 31% and 95%, it was decided to assume a seroprevalence of 50% to maximise the sample size. With an accuracy of 3% and a confidence level of 95%, we calculated a minimum sample size of 1,067 serum samples. Overestimating to account for possible missing values in the serological analysis, 1,153 participants were included in the study.
Serological analysis
The presence of IgG antibodies against the measles virus was determined by indirect ELISA (Enzygnost® Anti-Measles Virus/IgG; Siemens, Marburg, Germany) according to the manufacturer's instructions. Serum samples with absorbance values < 0.100 were considered negative, absorbance values > 0.200 were considered positive, and absorbance values situated between these two figures were classified as indeterminate.
IgG antibodies specific for VZV, mumps, and rubella virus were quantified by ELFA (VIDAS; bioMeriuex, Inc., Marcy l’Etoile, France). The test value (TV) for each sample was obtained by calculating the ratio of the relative fluorescence value (RFV) of each sample to a standard. IgG antibody levels were considered to confer immunity if the value of the test (TV) was ≥ 0.90 for VZV and ≥ 0.50 for mumps virus. In the case of IgG antibodies specific for rubella virus, results were calculated as IU/ml according to the standards of the WHO, which considers values <10 IU/ml to be negative and values ≥ 15 UI/ml to be positive.
IgG antibodies against B. pertussis and the pertussis toxin (PT) of B. pertussis were determined using a commercial qualitative ELISA method (Novagnost® Bordetella pertussis IgG, Siemens). Following the manufacturer's recommendations, all sera were tested in duplicate, and results were considered positive when absorbance values were greater than 15% above the cut-off value and negative when absorbance values were less than 15% of the cut-off value.
Statistical analysis
The collected data were entered into a database using the double-entry validation method. The database was then refined. A descriptive analysis was performed on the total valid data using measures of central tendency and dispersion (mean or median if the distribution was asymmetric) together with their corresponding 95% confidence intervals for quantitative variables and frequency distribution (prevalences and proportions with 95% confidence intervals) for qualitative variables.
Age variable normality was confirmed by the Kolmogorov-Smirnov test.
Pearson’s χ2 test was employed to compare prevalences (if the expected frequency was less than 5, Fisher’s test was used).
The Mann-Whitney U test was used to compare means, and the Kruskal-Wallis test was applied for variables with more than 2 categories. For all hypothesis tests used to estimate differences, associations, and relationships, p values less than 0.05 were considered significant.
The software PASW (IBM SPSS Statistics, Armonk, NY, USA) version 18.0 was used for statistical analysis of the data.
| Abbreviations: | ||
| EIA | = | enzyme immunossay |
| ELISA | = | enzyme- linked Immuno sorbent Assay |
| ELFA | = | enzyme linked fluorescent assay |
| ESEN | = | European Sero-Epidemiology Network |
| ICH/CPMP/135/95 | = | Harmonised Tripartite Guidelines for Good Clinical Practice |
| IgG | = | immunoglobulin G |
| IU/ml | = | international units per milliliter |
| MMR | = | immunisation against measles, mumps, and rubella |
| PT | = | pertussis toxin |
| RFV | = | relative fluorescence value |
| Tdap | = | acellular pertussis vaccine |
| TV | = | test value |
| WHO | = | World Health Organization |
| VZV | = | varicella-zoster virus |
Acknowledgments
This project was funded by “Fondo de Investigaciones Sanitarias” grant PS09/02331.Ministerio de Sanidad, Instituto de Salud Carlos III. Spain
Disclosure of Potential Conflicts of Interest
No potential conflicts of interest were disclosed.
References
- Measles WHO. A strategic framework for the elimination of measles in the European Region. The Expanded Programme on Immunization in the European Region of WHO (1999) Copenhagen. http://www.euro.who.int/__data/assets/pdf_file/0003/119802/E68405.pdf. Accessed 12 October 2012.
- World Health Organization. Eliminating measles and rubella and preventing congenital rubella infection. WHO European Region strategic plan 2005-2010 (2005) Copenhagen: WHO Regional Office For Europe. http://www.euro.who.int/document/E87772.pdf. Accessed 12 October 2012.
- Nardone A, Pebody RG, van den Hof S, Levy-Bruhl D, Plesner AM, Rota MC, et al. Sero-epidemiology of mumps in western Europe. Epidemiol Infect 2003; 131:691 - 701; http://dx.doi.org/10.1017/S0950268803008768; PMID: 12948369
- de Madrid C. Dirección General de Salud Pública y Alimentación. Vacunación frente a rubeola en mujeres en edad fértil. Control del síndrome de rubeola congénita. http://www.madrid.org/cs/Satellite?blobcol=urldata&blobheader=application%2Fpdf&blobheadername1=Content-disposition&blobheadername2=cadena&blobheadervalue1=filename%3DDOCUMENTO_TECNICO_RUBEOLA.pdf&blobheadervalue2=language%3Des%26site%3DPortalSalud&blobkey=id&blobtable=MungoBlobs&blobwhere=1271649994128&ssbinary=true.Accessed 10 September 2012.
- Community of Madrid. Report on the health status of the population of the Community of Madrid 2009. http://www.madrid.org/cs/Satellite?cid=1142588809240&language=es&pagename=PortalSalud%2FPage%2FPTSA_pintarContenidoFinal&vest=1161769238915. Accessed 14 April 2013.
- Tagarro García A, Jiménez Bueno S, Herreros Fernández ML, Santiago García B, González Gil I, Baquero-Artigao F, et al. [Outbreak of measles in the population of Spanish origin in North Madrid]. An Pediatr (Barc) 2012; 76:350 - 4; PMID: 22265376
- EUVAC. Net. ECDC measles and rubella monitoring (EMMO) http://ecdc.europa.eu/en/publications/Publications/2012June13_SUR_measles_rubella_report.pdf. Accessed 24 March 2013.
- National Epidemiology Center. Health Institute Carlos III. Annual report of the plan for eliminating measles, rubella, and congenital rubella syndrome in Spain 2010.http://www.isciii.es/ISCIII/es/contenidos/fd-servicios-cientifico-tecnicos/fd-vigilancias-alertas/fd-enfermedades/fd-enfermedades-prevenibles-vacunacion/Informe-Anual-Plan-Eliminacion-del-Sarampion-Rubeola-y-Sindrome-de-Rubeola-Congenita-Espana-2010.pdf.Accessed 10 april 2013.
- Cardeñosa Marín N. [Seroepidemiologic studies]. Rev Esp Salud Publica 2009; 83:607 - 10; http://dx.doi.org/10.1590/S1135-57272009000500017; PMID: 20111809
- III Serosurveillance Survey of the community of Madrid (2002). Bol Epidemiol Comunidad Madrid; 8:3-41 http://www.madrid.org/cs/Satellite?blobtable=MungoBlobs&blobcol=urldata&blobkey=id&blobheadervalue1=filename%3Dmayo2002.pdf&blobwhere=1119142927576&blobheadername1=Content-Disposition&ssbinary=true&blobheader=application%2Fpdf. Accessed 22 April 2013.
- National Epidemiology Center. Health Institute Carlos III (2000) Seroepidemiological Study: Status of vaccine-preventable diseases in Spain. Health Institute Carlos III. http://www.isciii.es/ISCIII/es/contenidos/fd-servicios-cientifico-tecnicos/fd-vigilancias-alertas/fd-enfermedades/SEROEPIDEMIOLOGICO.pdf. Accessed 22 April 2013.
- Guillen JM, Gil-Prieto R, Alvaro A, Gil A. Burden of adult varicella hospitalizations in Spain (2001-2007). Hum Vaccin 2010; 6:659 - 63; http://dx.doi.org/10.4161/hv.6.8.12014; PMID: 20523119
- Tos ferina [Pertussis]. Bol Epidemiol Comunidad de Madrid. 2008; 11:39-49. http://www.madrid.org/cs/Satellite?blobcol=urldata&blobheader=application%2Fpdf&blobheadername1=Content-disposition&blobheadername2=cadena&blobheadervalue1=filename%3DNoviembre2008.pdf&blobheadervalue2=language%3Des%26site%3DPortalSalud&blobkey=id&blobtable=MungoBlobs&blobwhere=1220585963986&ssbinary=true Accessed 22 April 2013.
- Tischer A, Andrews N, Kafatos G, Nardone A, Berbers G, Davidkin I, et al. Standardization of measles, mumps and rubella assays to enable comparisons of seroprevalence data across 21 European countries and Australia. Epidemiol Infect 2007; 135:787 - 97; http://dx.doi.org/10.1017/S0950268807008266; PMID: 17394675
- Sanz Moreno JC, García Comas L, Ramírez Fernández R, Ramos Blázquez B, Ordobás Gavín M. [Evolution of measles, rubella and mumps from the third seroepidemiological survey in the autonomous region of Madrid, Spain]. Rev Esp Salud Publica 2009; 83:625 - 37; PMID: 20111811
- Community of Madrid. Report on epidemiological surveillance 2007-2010. Measles, rubella and congenital rubella syndrome. http://www.madrid.org/cs/Satellite?blobcol=urldata&blobheader=application%2Fpdf&blobheadername1=Contentdisposition&blobheadername2=cadena&blobheadervalue1=filename%3DSAR_RUB_2007_10.pdf&blobheadervalue2=language%3Des%26site%3DPortalSalud&blobkey=id&blobtable=MungoBlobs&blobwhere=1310786570627&ssbinary=true. Accessed 22 April 2013.
- Amela C, Pachón I, de Ory F. Evaluation of the measles, mumps and rubella immunisation programme in Spain by using a sero-epidemiological survey. Eur J Epidemiol 2003; 18:71 - 9; http://dx.doi.org/10.1023/A:1022567811765; PMID: 12705626
- Mossong J, Putz L, Schneider F. Seroprevalence of measles, mumps and rubella antibodies in Luxembourg: results from a national cross-sectional study. Epidemiol Infect 2004; 132:11 - 8; http://dx.doi.org/10.1017/S0950268803001584; PMID: 14979584
- Theeten H, Hutse V, Hens N, Yavuz Y, Hoppenbrouwers K, Beutels P, et al. Are we hitting immunity targets? The 2006 age-specific seroprevalence of measles, mumps, rubella, diphtheria and tetanus in Belgium. Epidemiol Infect 2011; 139:494 - 504; http://dx.doi.org/10.1017/S0950268810001536; PMID: 20587123
- Domínguez A, Plans P, Costa J, Torner N, Cardenosa N, Batalla J, et al. Seroprevalence of measles, rubella, and mumps antibodies in Catalonia, Spain: results of a cross-sectional study. Eur J Clin Microbiol Infect Dis 2006; 25:310 - 7; http://dx.doi.org/10.1007/s10096-006-0133-z; PMID: 16786377
- Matter L, Kogelschatz K, Germann D. Serum levels of rubella virus antibodies indicating immunity: response to vaccination of subjects with low or undetectable antibody concentrations. J Infect Dis 1997; 175:749 - 55; http://dx.doi.org/10.1086/513967; PMID: 9086126
- Nardone A, Tischer A, Andrews N, Backhouse J, Theeten H, Gatcheva N, et al. Comparison of rubella seroepidemiology in 17 countries: progress towards international disease control targets. Bull World Health Organ 2008; 86:118 - 25; http://dx.doi.org/10.2471/BLT.07.042010; PMID: 18297166
- Hernández Díaz R, Rodrigo Val MP, Misiego Peral A, Roc Alfaro ML, Adiego Sancho MB. [Seroepidemiologic study of rubella in childbearing women in Aragon, Spain (2003-2007)]. Gac Sanit 2011; 25:20 - 2; PMID: 21074904
- Garrido Álvarez E, Álvarez Pasquín MJ, Gómez Marco J, Martín Martín S, Kloppe Villegas P, Hernando López T. Seroprevalence of antibodies against rubella in female immigrants of childbearing age in two health centres in Madrid. Vacunas 2004; 5:75 - 8
- Eriksen J, Davidkin I, Kafatos G, Andrews N, Barbara C, Cohen D, et al. Seroepidemiology of mumps in Europe (1996-2008): why do outbreaks occur in highly vaccinated populations?. Epidemiol Infect 2012; 12:1 - 16; PMID: 22687578
- Gabutti G, Guido M, Rota MC, De Donno A, Ciofi Degli Atti ML, Crovari P, Seroepidemiology Group. The epidemiology of mumps in Italy. Vaccine 2008; 26:2906 - 11; http://dx.doi.org/10.1016/j.vaccine.2008.03.040; PMID: 18439732
- National Epidemiology Center. Institute of Health Carlos III. (2006) Status of varicella in Spain (2006). http://www.isciii.es/ISCIII/es/contenidos/fd-servicios-cientifico-tecnicos/fd-vigilancias-alertas/fd-enfermedades/fd-enfermedades-prevenibles-vacunacion/InformevaricelaCNE.pdf. Accessed 17 April 20123.
- Peña-Rey I, Martínez de Aragón MV, Villaverde Hueso A, Terres Arellano M, Alcalde Cabero E, Suárez Rodríguez B. [Epidemiology of varicella in spain pre-and post-vaccination periods]. Rev Esp Salud Publica 2009; 83:711 - 24; PMID: 20111819
- Clements DA, Zaref JI, Bland CL, Walter EB, Coplan PM. Partial uptake of varicella vaccine and the epidemiological effect on varicella disease in 11 day-care centers in North Carolina. Arch Pediatr Adolesc Med 2001; 155:455 - 61; PMID: 11296072
- Salleras L, Domínguez A, Plans P, Costa J, Cardeñosa N, Torner N, et al. Seroprevalence of varicella zoster virus infection in child and adult population of Catalonia (Spain). Med Microbiol Immunol 2008; 197:329 - 33; http://dx.doi.org/10.1007/s00430-007-0064-z; PMID: 18004592
- Chris Maple PA, Gunn A, Sellwood J, Brown DW, Gray JJ. Comparison of fifteen commercial assays for detecting Varicella Zoster virus IgG with reference to a time resolved fluorescence immunoassay (TRFIA) and the performance of two commercial assays for screening sera from immunocompromised individuals. J Virol Methods 2009; 155:143 - 9; http://dx.doi.org/10.1016/j.jviromet.2008.09.032; PMID: 18996415
- Nardone A, de Ory F, Carton M, Cohen D, van Damme P, Davidkin I, et al. The comparative sero-epidemiology of varicella zoster virus in 11 countries in the European region. Vaccine 2007; 25:7866 - 72; http://dx.doi.org/10.1016/j.vaccine.2007.07.036; PMID: 17919788
- Domínguez A, Vidal J, Plans P, Salleras L. The seroepidemiology of B. pertussis infection in Catalonia, Spain. Epidemiol Infect 2001; 126:205 - 10; http://dx.doi.org/10.1017/S0950268801005325; PMID: 11349970
- García-Corbeira P, Dal-Ré R, Aguilar L, García-de-Lomas J. Seroepidemiology of Bordetella pertussis infections in the Spanish population: a cross-sectional study. Vaccine 2000; 18:2173 - 6; http://dx.doi.org/10.1016/S0264-410X(00)00029-3; PMID: 10717335
- de Juanes JR, Gil A, González A, Arrazola MP, San-Martín M, Esteban J. Seroprevalence of pertussis antibody among health care personnel in Spain. Eur J Epidemiol 2004; 19:69 - 72; http://dx.doi.org/10.1023/B:EJEP.0000013270.63515.e6; PMID: 15012025
- Cattaneo LA, Reed GW, Haase DH, Wills MJ, Edwards KM. The seroepidemiology of Bordetella pertussis infections: a study of persons ages 1-65 years. J Infect Dis 1996; 173:1256 - 9; http://dx.doi.org/10.1093/infdis/173.5.1256; PMID: 8627081
- Rendi-Wagner P, Tobias J, Moerman L, Goren S, Bassal R, Green M, et al. The seroepidemiology of Bordetella pertussis in Israel--Estimate of incidence of infection. Vaccine 2010; 28:3285 - 90; http://dx.doi.org/10.1016/j.vaccine.2010.02.104; PMID: 20226250
- Quinn HE, McIntyre PB, Backhouse JL, Gidding HF, Brotherton J, Gilbert GL. The utility of seroepidemiology for tracking trends in pertussis infection. Epidemiol Infect 2010; 138:426 - 33; http://dx.doi.org/10.1017/S0950268809990707; PMID: 19719902
- Riffelmann M, Thiel K, Schmetz J, Wirsing von Koenig CH. Performance of commercial enzyme-linked immunosorbent assays for detection of antibodies to Bordetella pertussis. J Clin Microbiol 2010; 48:4459 - 63; http://dx.doi.org/10.1128/JCM.01371-10; PMID: 20943873
- Xing D, Markey K, Newland P, Rigsby P, Hockley J, He Q. EUVAC.NET collaborative study: evaluation and standardisation of serology for diagnosis of pertussis. J Immunol Methods 2011; 372:137 - 45; http://dx.doi.org/10.1016/j.jim.2011.07.005; PMID: 21782823
- Wirsing von König CH, Campins-Marti M, Finn A, Guiso N, Mertsola J, Liese J. Pertussis immunization in the global pertussis initiative European region: recommended strategies and implementation considerations. Pediatr Infect Dis J 2005; 24:Suppl S87 - 92; http://dx.doi.org/10.1097/01.inf.0000160920.75623.a3; PMID: 15876934