ABSTRACT
The present study used a cross-sectional survey design to explore the role of ego-depletion in the relationship between self-control and health-promoting behaviors in patients with coronary heart disease (CHD). This study recruited 277 patients with CHD to measure the levels of ego-depletion, self-control and health-promotion (HP) behavior using Self-Regulatory Fatigue Scale (SRF-s), Dual-Mode of Self-Control Scale (DMSD-s) and Health Promotion Lifestyle Profile-II (HPLP-II) to examine the relationship between the three. Study found that self-control improved the patients’ HP behaviors to some extent. Self-control in patients with CHD uses ego-depletion as the mediating variable to indirectly and positively predict the level of HP behavior, and the mediating effects account for 47.76% (impulsive system) and 15.6% (control system) of the total effects, respectively.
Introduction
Coronary Heart Disease (CHD) has become an important risk factor that threatens the health of Chinese residents. The 2019ACC/AHA guidelines for primary prevention of cardiovascular diseases also pointed out that the total number of deaths from cardiovascular diseases accounted for the first place in the total number of deaths in China every year (Dai et al., Citation2019). Consequently, CHD prevention and control are of utmost importance. Poor lifestyle choices, such as smoking, drinking, lack of exercise and so on, are responsible for the increasing prevalence of CHD. Some researchers believe that the establishment of health-promotion (HP) behavior in patients with CHD is even more significant than clinical treatment (Cheng & Li, Citation2018; Gao et al., Citation2015; Nes Lise et al., Citation2013). HP behavior is a process of enhancing people’s ability to control their health so as to improve individual health status. In this process, people actively take some specific behaviors in order to maintain and improve their health (Hamarneh et al., Citation2012). According to the theory of self-control resource, after a period of tasks requiring self-control in individuals, self-control resources will be consumed. When self-control resources are seriously consumed, individuals will experience temporary depletion of self-control resources, which is named ‘ego-depletion’ (Baumeister & Vohs, Citation2007; Muraven & Baumeister, Citation2000). Previous study has revealed that ego-depletion is a common psychological experience of most patients with chronic diseases. Undergoing serious physiological and psychological stress, patients need to endure the pain caused by physical diseases, as well as regulate emotions, which rapidly depletes the patients’ self-control resources. As a result, patients often do not have enough self-control resources to manage their own health, and are unable to perform better HP behaviors (Detweiler-Bedell et al., Citation2008). Therefore, ego-depletion emerges as the principal cause of self-control failure and an important antecedent variable affecting HP behaviors. Other studies have found that self-control and ego-depletion are mutual cause and effect and influence each other (Martin et al., Citation2010; Yuan & Li, Citation2009). At the same time, some studies have also confirmed that relevant methods of improving self-control can be carried out from ‘open source’ and ‘throttling’, which can slow down or supplement the ego-depletion, such as supplementing glucose, constructing positive psychological resources and improving motivation (Bodenheimer et al., Citation2009; Fredrickson & Branigan, Citation2003; Gailliot, Citation2007; Hu et al., Citation2008).
In conclusion, this study hypothesized that the health promotion behavior of patients with CHD is not only affected by the self-control ability, but also by the ego-depletion mediating effect. This hypothesis was verified by the bootstrap method of AMOS21.0 statistical software. Our ultimate aim was to open up a new way for the prevention and treatment of CHD from the psychological and behavioral perspective, and to provide a new direction for disease behavior management. We also wanted to expand the application and development of ego-depletion theory in chronic disease groups.
Materials and methods
Participants
The study participants were patients with CHD which recruited from the department of cardiology of a grade III class A hospital in Chengde city, Hebei province, China, from February to July 2018 by convenient sampling. The inclusion criteria were as follows: (1) Conform to the 2015 ACC/AHA diagnostic criteria for CHD (Guang & Dai, Citation2016), (2) Patients who were diagnosed for the first time and their hospitalization time did not exceed 7 days (based on the requirements of the turnover rate of beds in tertiary hospitals in China), (3) Clear consciousness, accurate expression and barrier-free communication. The exclusion criteria were as follows: patients with neurological or psychiatric disorders and severe diseases of the digestive, respiratory, circulatory and endocrine systems. A total of 300 questionnaires were distributed, of which 277 were effective, and the effective rate was 92.33%.
Ethical considerations
The study was approved by the Ethical Committee of Chengde Medical University (Number: 2018007). The patients signed a written informed consent form before study.
Demographic and medical variables
We extracted the demographic information and medical variables of all of the patients from the hospital records, such as gender, age, medical payment methods, caregivers, complications and so on.
Ego-depletion questionnaire
Ego-depletion was measured by the Self-Regulatory Fatigue Scale (SRF-S). SRF-S consists of three dimensions: cognitive control, emotional control and behavior control, has 16 items, Likert rating (1 to 5 points) was used, with scores ranging from 16 to 80. The higher the score, the greater the degree of ego-depletion. Cronbach’s α = 0.84 (Nes Lise et al., Citation2013). In the present study, Cronbach’s α = 0.79.
Self-control questionnaire
Self-control was measured by the Dual-Mode of Self-Control Scale (DMSC-S). DMSC-S includes two systems, namely control system and impulse system. The control system consists of two dimensions: future time view, problem solving. The impulse system consists of three dimensions: easy distraction, low delay gratification, and impulsivity. Likert rating (1 to 5 points) was used. The higher the score, the better the self-control. The DMSC-S Cronbach’s α = 0.82. The control system and impulse system Cronbach’s α = 0.74 and 0.80 (Dvorak, Citation2009).
Health-promotion behavior questionnaire
Health-promotion behavior was measured by the Health Promotion Lifestyle Profile-II (Pender, Citation1987; Pender et al., Citation2006; Walker et al., Citation1987). The revised Chinese version was revised, which contains 6 dimensions and 48 items, namely: nutrition (NU), physical activity (PA), stress management (SM), interpersonal relationship (IR), spiritual growth (SG), and health responsibility (HR). Likert rating (1 to 4 points) was used, with scores ranging from 48 to 192. The higher the score, the better the HP behavior. The scoring criteria were: excellent 156–192 points, good 121–156 points, general 85–120 points, poor 48–84 points, Cronbach’s α = 0.93. (Meihan & Chung-Ngok, Citation2011). In this study, Cronbach’s α = 0.91, Cronbach’s range of each subscale was 0.72 ~ 0.84.
Statistical analysis
There were 23 missing data (7.67%) that were directly removed from the dataset. SPSS22.0 and AMOS21.0 statistical software were used for data analysis. Measurement data were represented by mean/standard deviation (±s). Numeric data were described in terms of frequency (n)/percentage (%). Pearson correlation analysis was used to analyze the correlation among variables. AMOS21.0 statistical software Bootstrap method was used to verify the model assumptions.
Results
Descriptive statistics
presents the demographics and medical characteristics of patients with CHD. A total of 277 patients were included in the final data analysis, the mean age was 62.4 ± 24.5 years (range,28–78). presents the total score and dimension score of SRF-S, DMSC-S and HPLP-II. presents the total score of SRF-S,DMSC-S and HPLP-II and the Correlation among variables. presents the multiple linear regression analysis of influencing factors of health promotion behavior in patient with CHD.
Table 1. The demographics and medical characteristics of participants
Table 2. Total score and dimension score of SRF-S, DMSC-S and HPLP-II (±s)
Table 3. Correlation among variables
Table 4. Mediating effect analysis results
Structural equation model
We analyzed the mechanisms of ego-depletion and self-control on HP behavior in patients with CHD, constructed a path analysis model based on relevant analysis results and research hypothesis, and validated the model hypothesis with AMOS 21.0 statistical software. The results of model fitting showed that:χ2/df = 1.08, RMSEA = 0.02 (P < 0.01), CFI = 0.99, GFI = 0.98, IFI = 0.97, TLI = 0.95, where all were >0.90, which in turn suggested that the model fit the data well. Effect relationships: ① Self-controlled impulse system and control system directly and negatively predicted ego-depletion. The standardized path coefficients were −0.81[95%CI(−0.57,-0.49)], −0.19[95%CI(−0.20,-0.13)]. ② ego-depletion directly and negatively predicted the levels of HP behavior. The standardized path coefficients were −0.39[95%CI(−0.39,-0.13)]. ③Self-control in patients with CHD indirectly and positively predicted the levels of HP behavior with ego-depletion as a mediation effect variable. The standardized path coefficients were −0.39*-0.81 = 0.32 (Impulsive system of self-control) and −0.39*-0.19 = 0.07 (Control system of self-control). The total effects of self-control on the level of HP behavior were as follows: 0.32 + 0.35 = 0.67 (Impulsive system of self-control) and 0.07 + 0.38 = 0.45 (Control system of self-control). The results showed that self-regulated fatigue had a mediating role in the effect of self-control on the level of health promotion behavior, and the mediating effect accounted for 47.76% and 15.6% of the total effect. The mediation model is shown in .
Figure 1. Models of the mediation effect of ego-depletion on self-control and health-promotion behavior in patients with CHD.
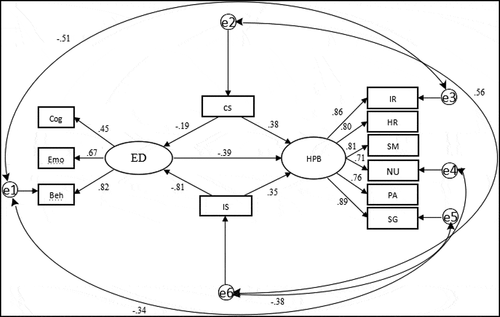
Cog, cognitive; Emo, emotion; Beh, behavior; ED, ego depletion; CS, control system; IS, impulsive system; HPB, health-promotion behavior; IR, interpersonal relationship; HR, health responsibility; SM, stress management; NU, nutrition; PA, physical activity; SG, spiritual growth.
Discussion
This study found that the level of HP in patients with CHD is at medium level, which is consistent with Wang’s study (Zou, Citation2020), lower than that of results reported by Percival et al. (Nikki et al., Citation2018). The establishment of individual HP behavior is crucial for reducing the incidence of CHD and improving the patient’s prognosis, whether from the perspective of patients’ own rehabilitation or from the perspective of the implementation of clinical nursing work (Nes Lise et al., Citation2013). More than 50% of the occurrence of CHD is closely related to people’s poor lifestyle such as diet, exercise, smoking, alcohol abuse, and so on (EVans, Citation2010). Seventy five percent of the risk factors of CHD can also be attributed to the fact that individuals choose the wrong way of life and behavior (Liu et al., Citation2014). For these unhealthy lifestyle choices, patients with CHD need to control themselves in order to avoid ego-depletion. (Inzlicht et al., Citation2014). As a personality trait, self-control is an individual’s ability to self-regulate while health promotion behavior is an individual’s perception and actively generated behavior in order to maintain and improve health and realize self-worth. Therefore, self-control affects the implementation of HP behavior. Self-control includes impulse system and control system, where impulse system is more likely to lead to the lack of self-control and to unhealthy habits such as smoking, alcohol and consumption of foods high in sugar. Conversely, control system helps to resist the bad temptation and insist on healthy behaviors to achieve self-control (Liu et al., Citation2014). Impulse system and control system are mutually restrictive and interrelated, thus affecting the execution level of HP behavior.
This study found that the direct path test showed that self-control directly predicts HP behavior, while ego-depletion negatively predicts HP behavior. Fleig et al. have found that the enhancement of individual self-control can successfully induce their own healthy behavior, and have pointed out that ego-depletion can predict the healthy behavior in patients (Fleig et al., Citation2013). This study also found that patients with CHD who have relatively poor self-control ability tend to be in a state of high ego-depletion, and their HP behavior level is low. According to the theory of self-control resources, the decline of individual self-control ability is caused by the insufficiency of self-control resources. The insufficiency of self-control resources leaves patients in a state of ego-depletion (Baumeister et al., Citation2018; Tan et al., Citation2012). Nes et al. have also pointed out that ego-depletion or excessive self-depletion are common in patients with chronic diseases, which seriously affect the patients’ quality of life (Nes Lise et al., Citation2010). Therefore, the low level of health-promotion behavior in patients with CHD may be related to long-term ego-depletion. Ego-depletion may be a negative state of individual mental resource shortage, which leads to the individual not having enough psychological resources to carry out health promotion behaviors, such as regular medication after discharge, regular review, long-term monitoring of heart rate, blood pressure and so on.
Therefore, this study suggests that scientific and effective intervention measures can be taken to supplement their psychological resources, alleviate ego-depletion of patients, and enable patients have a high level of self-control ability to carry out health promotion behavior.
Conclusion
Patients with CHD are all in a state of ego-depletion. The interaction among ego-depletion, self-control and HP behavior is significant. Ego-depletion plays a mediating role between self-control and HP behavior.
Disclosure statement
No potential conflict of interest was reported by the authors.
Additional information
Funding
References
- Baumeister, R. F., Tice, D. M., & Vohs, K. D. (2018). The strength model of self-regulation: Conclusions from the second decade of willpower research. Perspectives on Psychological Science : A Journal of the Association for Psychological Science, 13(2), 141–145. https://doi.org/https://doi.org/10.1177/1745691617716946
- Baumeister, R. F., & Vohs, K. D. (2007). Self-regulation, ego depletion,and motivation. Social and Personality Psychology Compass, 1(1), 115–128. https://doi.org/https://doi.org/10.1111/j.1751-9004.2007.00001.x
- Bodenheimer, T., Chen, E., & Heather, D. B. (2009). Confronting the growing burden of chronic disease: Can the U.S. health care work-force do the job? Health Affairs, 28(1), 64–74. https://doi.org/https://doi.org/10.1377/hlthaff.28.1.64
- Cheng, S. H., & Li, L. (2018). Investigation and analysis of the needs for clinical health education of middle-aged and old-aged patients with coronary heart disease. Preventive Medicine in South China, 44 (2), 195–197. In Chinese. doi:https://doi.org/10.13217/j.scjpm.2018.0195
- Dai, T. T., Huang, J. H., Yin, T., Tang, H. Y., H, L., & Huang, Q., (2019). Key points from the 2019 ACC/AHA guidelines on the primary prevention of cardiovascular disease. Chinese Journal of Vascular Surgery, 4, 206-209. DOI:https://doi.org/10.3760/cma.j.issn.2096-1863.2019.04.004.
- Detweiler-Bedell, J. B., Friedman, M. A., Leventhal, H., Miller I. W., & Leventhal E. A. (2008). Integrating co-morbid depression and chronic physical disease management: Identifying and resolving failures in self-regulation. Clinical Psychology Review, 28(8), 1426–1446. https://doi.org/https://doi.org/10.1016/j.cpr.2008.09.002
- Dvorak, R. D., & Simons, J. S. . (2009). Moderation of resource depletion in the self-control strength model: differing effects of two modes of self-control. Personality & Social Psychology Bulletin, 35(5), 572. doi:https://doi.org/10.1177/0146167208330855
- Fleig, L., Pomp, S., Parschau, L., Barz, M., Lange, D., Schwarzer, R., & Lippke, S. (2013). From intentions via planning and behavior to physical exercise habits. Psychology of Sport &exercise, 14(5), 632–639. https://doi.org/https://doi.org/10.1016/j.psychsport.2013.03.006
- Fredrickson, B., & Branigan, C. (2003). Positive emotions broaden the scope of attention and thought‐action repertoires. Cognition & Emotion, 19(3), 313–332. https://doi.org/https://doi.org/10.1080/02699930441000238
- Gailliot, M. T. (2007). The physiology of willpower: Linking blood glucose to self-control. Personality and Social Psychology Review, 11(4), 303–327. https://doi.org/https://doi.org/10.1177/1088868307303030
- Gao, X. J., Yang, J. G., & Yang, Y. J. (2015). Analysis of cardiovascular risk factors in patients with acute myocardial infarction in China. Chinese Journal of Circulation, 30 (3), 206–210. In Chinese. DOI: https://doi.org/10.3969/j.issn.1000-3614.2015.03.003.
- Guang, X. F., & Dai, H. L. (2016).Chinese Journal of Practical Internal Medicine, 36 (4), 281–283. In Chinese. DOI:https://doi.org/10.7504/nk2016030201.
- Hagger, M. S., Wood, C., Stiff, C., & Chatzisarantis, N. L. D. (2010). Ego depletion and the strength model of self-control: A meta-analysis. Psychological Bulletin, 136(4), 495–525.
- Hamarneh, A. Y., Agus, A., & Campbell, D. (2012). Public perceptions of coronary events risk factors: A discrete choice experiment. BMJ Open, 2(5), 1–6. https://doi.org/https://doi.org/10.1136/bmjopen-2012-001560
- Hu, S. N., Chen, Z. J., & Dou, D. H. (2008). Alternative recovery and mechanism of other people’s positive emotions on self-control resources. Psychology and Behavior Research, 16(1), 45–50. http://www.cnki.com.cn/Article/CJFDTotal-CLXW201801006.htm
- Inzlicht, M., Schmeichel, B. J., & Macrae, C. N. (2014). Why self-control seems (but may not be) limited. Trends in Cognitive Sciences, 18(3), 127–133. https://doi.org/https://doi.org/10.1016/j.tics.2013.12.009
- Liu, Z. X., Li, Q. Y., Gan, Y. Q., Miao, M. Feng, Y., Nie, H. Y., & Chen, W. Y., (2014). Consistency between health attitude and health behavior: A regulated regulating model. Chinese Journal of Mental Health, 28 (8), 586–591. DOI:10. 3969 /j. issn. 1000-6729. 2014. 08.006.
- Meihan, L., & Chung-Ngok, W. (2011). Validation of the psychometric properties of the health-promoting lifestyle profile in a sample of Taiwanese women. Quality of Life Research : An International Journal of Quality of Life Aspects of Treatment, Care and Rehabilitation, 20(4), 523–528. https://doi.org/https://doi.org/10.1007/s11136-010-9790-6
- Muraven, M., & Baumeister, R. F. (2000). Self-regulation and depletion of limited resources: Does self-control resemble a muscle? Psychological Bulletin, 126(2), 247–259. https://doi.org/https://doi.org/10.1037/0033-2909.126.2.247
- Nes Lise, S., Carlson, C.R., Crofford, L.J., de Leeuw, R. & Segerstrom, S.C. (2010). Self-regulatory deficits in fibromyalgia and temporomandibular disorders. Pain, 151(1), 37–44. https://doi.org/https://doi.org/10.1016/j.pain.2010.05.009
- Nes Lise, S., Ehlers, S. L., Whipple, M.O., & Vincent, A. (2013). Self-regulatory fatigue in chronic multisymptom illnesses: Scale development, fatigue, and self-control. Journal of Pain Research, 6, 181–188. https://doi.org/https://doi.org/10.2147/JPR.S40014
- Nikki, A., Janya, M., Christine, A., Lynette, O., Roxanne, B., Kevin, R., & Joyce, D. (2018). Implementing health promotion tools in Australian indigenous primary health care. Health Promotion International, 33(1), 92–106. https://doi.org/https://doi.org/10.1093/heapro/daw049
- Pender, N. (1987). Health promotion in nursing practice. APPleton & Lange.
- Pender, N., Murdau, C., & Parsons, M. (2006). Health promotion in nursing practice. Pearson Prentice Hall.
- Tan, S. H., Xu, Y., & Wang, F. (2012). Ego depletion: Theory, influencing factors and research trend. Advances in Psychological Science, 20 (5), 715–725. In Chinese. https://doi.org/https://doi.org/10.3724/SP.J.1042.2012.00715.
- Vans, L. (2010). Because we don’t take better care of ourselves: Rural black women’s explanatory models of heart disease. Women Aging, 22(2), 94–108. https://doi.org/https://doi.org/10.1080/08952841003716121
- Walker, S., Sechrist, K., & Pender, N. (1987). The health promoting lifestyle profile: Development and psychometric characteristics. Nursing Research, 36(2), 77–81. https://doi.org/https://doi.org/10.1097/00006199-198703000-00002
- Yuan, D. H., & Li, X. D. (2009). Ego-depletion: An energy model for self-regulation. Journal of South China Normal University: Social Science Edition. (01), 137–144. http://www.cnki.com.cn/Article/CJFDTotal-HNSB200901027.htm
- Zou, B. L., Zheng, M., (2020). Correlation between health promotion behaviors, coping styles and levels of hope in the elderly patients with coronary heart disease complicated with hypertension and diabetes mellitus. Chinese General Practice nursing,18(2),135-138. doi:https://doi.org/10.12104/j.issn.1674-4748.2020.02.002
