ABSTRACT
Internalized homonegativity results from the acceptance of negative attitudes about one’s same-sex orientation, which has negative consequences for the health of gay, bisexual and other men who have sex with men (GBM). We translated the 7-item Reactions to Homosexuality Scale (RHS) to Brazilian Portuguese and assessed its factor structure, validity and reliability. The first step included the translation, back-translation, evaluation, peer review, and pre-testing of the scale. Then, we piloted the scale in two convenience samples of adult Brazilians recruited online during October 2019 and February to March 2020 through advertisements on Grindr and Hornet, respectively. The largest sample was randomly split into two groups for exploratory factor analysis (EFA) then confirmatory factor analysis (CFA). Criterion and construct validity were assessed via correlations between scale scores and study variables. A total of 5573 GBM (sample 1: 218; sample 2: 5355) completed the RHS. EFA (N = 2652) yielded two eigenvalues greater than one (Factor 1: 3.5 and Factor 2: 1.1). A one-factor solution provided the most interpretable model based on examination of scree plot and item factor loadings (χ2(14) = 1373.1, p < 0.001; CFI = 0.89; TLI = 0.84; RMSEA = 0.19; SRMS = 0.09). Though one-factor CFA showed moderate fit, freeing errors terms to covary, based on item content and interpretation, significantly improved model fit (χ2(12) = 309.1, p < .001; CFI = 0.97; TLI = 0.96; RMSEA = 0.09; SRMR = 0.02). As hypothesized, men who did not self-identify as gay (mean score 17.9 compared to those self-identifying as gay: 11.8) and men who reported no sex with men in the past 6 months (mean score 12.6 compared to those who reported sex with men: 10.6) scored higher reflecting higher internalized homonegativity. The RHS was effectively translated and validated in Brazilian Portuguese and can be used to evaluate the role of internalized homonegativity on GBM’s health, as well as its impact on the uptake of HIV prevention technologies.
Introduction
Internalized homonegativity (or internalized homophobia; IH) results from the acceptance of negative attitudes about one’s same-sex orientation (Shidlo, Citation1994). Its origin is understood through the framework of social stigma as proposed by Goffman (Goffman, Citation1990), which posits that stigma is an attribute that is socially discrediting and can cause an individual to be mentally classified by others as undesirable or rejected rather than accepted or normal. Within cultural and social environments, individuals learn at an early age the negative attitudes associated with stigmatized groups. Once individuals identify as sexual and gender minority (SGM), they may internalize the societal negative messages toward gender and sexuality as part of their own image (Meyer, Citation1995), resulting in negative feelings about themselves (Herek, Citation2000). This creates a psychological dichotomy between romantic or sexual desire and negative beliefs, leading to guilt, shame, low self-esteem and self-deprecating attitudes (Berg et al., Citation2016; Herek, Citation2007; Shidlo, Citation1994).
IH has been shown to be associated with substance use (Jeffries & Johnson, Citation2018; Turpin et al., Citation2020) and other mental health problems, such as depression and anxiety, as verified in a meta-analytic review (Newcomb & Mustanski, Citation2010). In another meta-analysis, Newcomb and Mustanski evaluated the positive association of IH with high-risk sexual behavior and showed that it was small and that it has possibly decreased over time. However, the authors noted that these results should be contextualized and evaluated with caution, as the study populations were comprised mostly of white gay, bisexual and other men who have sex with men (GBM) from major metropolitan areas in the US, where societal tolerance with SGM has significantly increased over the past decades (Newcomb & Mustanski, Citation2011).
IH has also been linked with reduced access to health services, including HIV treatment and prevention, and is a barrier to developing strategies on how to best address the needs of SGM (Altman et al., Citation2012). Previous use of HIV prevention tools such as preexposure prophylaxis (PrEP) and postexposure prophylaxis (PEP) were found to be significantly lower in regions with high levels of homonegativity (Melendez-Torres et al., Citation2020). The positive association of IH and never testing for HIV has been shown among Black GBM from the US (Matthews et al., Citation2019), GBM from China (Sun et al., Citation2020) as well as European GBM in a large web-based survey conducted in 38 countries (M W Ross et al., Citation2013). In the European study, positive associations of non-gay identity and younger age (Berg et al., Citation2015) as well as engagement in high-risk sexual behavior (M W Ross et al., Citation2013) with IH were also observed. In Uganda, one of the most homophobic countries according to Homophobic Climate Index (Lamontagne et al., Citation2018), GBM reporting condomless anal sex had higher IH (M W Ross et al., Citation2013). In the US, IH was identified as a barrier to PrEP use in a sample of young GBM (Meanley et al., Citation2020).
Globally, different scales have been proposed and developed to measure IH (Berg et al., Citation2016). The first scale to operationalize the construct, based on theoretical and clinical components, was the Reactions to Homosexuality Scale (RHS) developed by Ross and Rosser (Citation1996). It was a 26-item scale that measured four dimensions of IH: (1) public identification as gay, (2) perceptions of stigma associated with being gay, (3) social comfort with gay men, and (4) moral and religious acceptability of being gay (Ross & Rosser, Citation1996). This original scale was translated and validated in European Portuguese (Pereira & Leal, Citation2005). Currie et al. (Citation2004) developed a 12-item version of the scale that omitted the perceptions of stigma dimension, which was thought to not address the construct of IH but instead a broader social acceptability of the gay identity.
A 7-item RHS (Smolenski et al., Citation2010) was later developed with the intent to address the limitations associated with previous versions. The scale was first validated using an online sample of GBM from the US in English and Spanish. Later, the scale’s measurement and structural invariance was assessed in Europe (Tran et al., Citation2018; M W Ross et al., Citation2013) and Uganda (M W Ross et al., Citation2013). In these studies, three of the original dimensions were evaluated: (1) social comfort with gay men (2-items), which measures comfort in social situations with other gay men and in gay venues, such as gay bars; (2) public identification as gay (2-items), which measures comfort discussing homosexuality in public or to be seen with someone who is obviously gay, and (3) personal comfort with a gay identity (3-items), which measures comfort with one’s own sexuality and the belief that homosexuality is as natural as heterosexuality. Limitations of this short version include an inconclusive evaluation of whether the scale can be used unidimensionally given the existence of three proposed dimensions and two factors that each only had two indicators (Supplementary Table 1 provides an overview of past publications that have reported on the RHS’s factor structure).
Table 1. The seven items of the Reaction to Homosexuality Scale translated in Brazilian Portuguese
Brazil is a country of deep social inequalities that have great consequences for health access, use, and outcomes (Bilal et al., Citation2019). Despite recent advances on SGM rights, such as same-sex marriage in 2013 and criminalization of homophobia in 2019, the violence rate is shocking; in 2019, one SGM Brazilian was murdered or committed suicide every 26 hours (Grupo Gay Bahia, Citation2020). GBM are highly affected by the HIV epidemic in the country; HIV prevalence is estimated at 18.4% among GBM, while it is below 0.5% in the general population (Kerr et al., Citation2018; Luz et al., Citation2019). This context of prejudice, fear, stigma, and discrimination creates a hostile and stressful social environment impacting the perception and acceptability of one’s sexuality (Meyer, Citation2003; Sabidó et al., Citation2015). Previous studies have observed high engagement of high-risk sexual behavior among Brazilian GBM, such as condomless anal sex (Torres, Luz et al., Citation2019; Torres, Marins et al., Citation2019) and ‘chemsex’ (Torres et al., Citation2020) but, to the best of our knowledge, associations of these behaviors with IH have not been evaluated. To adequately study IH in the Brazilian context, a valid and reliable instrument is needed.
In the present study, we translated the 7-item RHS to Brazilian Portuguese and initially assessed its factor structure with exploratory factor analysis. We then conducted a confirmatory factor analysis in a separate sample and assessed internal reliability, and criterion and construct validity using a series of hypothesized correlates.
Materials and methods
Study design and location
The 7-item RHS was translated to Brazilian Portuguese and its factor structure, validity and reliability were assessed among GBM recruited online in Brazil using a cross-sectional design.
Ethics statement
This study was part of a project to study GBM behaviors, mental health and well-being, and knowledge of HIV transmission, prevention and treatment in Brazil. The institutional review board of the National Institute of Infectious Diseases (INI-Fiocruz) approved this study (#CAAE 01777918.0.0000.5262) in accordance with all applicable regulations. Participants provided informed consent before completing the surveys.
Translation
We performed translation of RHS items to Brazilian Portuguese following established guidelines (Beaton et al., Citation2000). Details of translation procedures were described elsewhere (Luz et al., Citation2020; Torres et al., Citation2021). A qualitative pretesting of the translated items was conducted with a small convenience sample to ensure item comprehensibility before moving into the reliability and construct validity step. Participants were requested to judge the clarity of each item on a scale (from 0 to 10); for scores ≤7, an additional open text field was provided, and participants were asked to provide suggestions to improve clarity. A group meeting of the research team was held to discuss the suggestions and items were adjusted as needed.
Study population
Sample 1
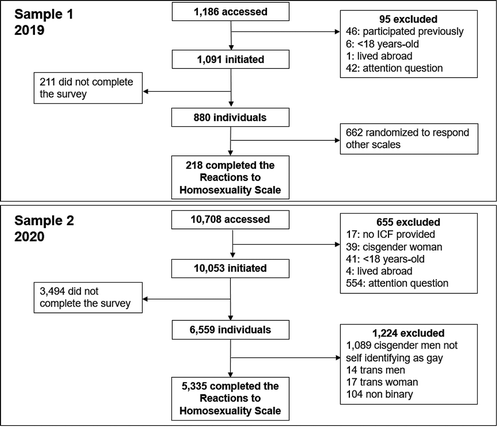
A first convenience sample was recruited during October-2019 to complete a web-based survey through advertisements on Grindr, a geospatial network app for GBM. Participant eligibility included (1) age ≥18 years, (2) identification as cisgender man, and (3) residency in Brazil. To decrease participant burden, random allocation of eligible participants to different instruments was performed such that each participant only responded to one instrument. Exclusion criteria were (1) an incorrect response to any of three attention questions included throughout the survey instrument at approximately every 15 items and (2) having responded to the survey previously ().
Sample 2
In order to provide more evidence of the scale’s validity and reliability, we recruited a second convenience sample during February and March 2020. The survey was launched through advertisements on a different app used by GBM (Hornet). We used the same inclusion and exclusion criteria as that for Sample 1 except for sexual orientation (only cisgender men self-identifying as gay were included).
Survey instrument
The survey instrument was divided into three sections. Section 1 included items on socio-demographic information and sexual orientation. Respondents had the possibility to choose ‘I don’t know’ or ‘I don’t want to answer’ to questions in Section 1, and these responses were considered missing. Section 2 included items referring to HIV testing and HIV test results. Section 3 included the items of the translated version of RHS.
As in prior studies, response options were on a 7-point Likert-type format ranging from strongly disagree (discordo fortemente, 0) to strongly agree (concordo fortemente, 6) (Berg et al., Citation2015; Tran et al., Citation2018; M W Ross et al., Citation2013). Six items were reversed scored (). IH total score was calculated by summing all scale items (maximum total score: 42). Higher scores indicate greater IH.
For Sample 2, a fourth section was included with items about prior PrEP use (yes/no), as well as two items addressing sexual behavior during the six months before the survey date: ‘did you have sex with men’ (yes/no) and ‘did you have condomless receptive anal sex’ (yes/no). Engagement in high-risk sexual behavior was defined as the report of condomless receptive anal sex in the previous 6 months.
Data analysis
Descriptive statistics were calculated as absolute number and percentages for categorical variables. Means and standard deviations (SDs) were calculated for each item of RHS, as well as for the total score.
Factor structure
The RHS’s factor structure was initially assessed with exploratory factor analysis (EFA) followed by confirmatory factor analysis (CFA). We randomly split Sample 2 and applied EFA to the first half and then CFA to the second half.
EFA was used to identify the number of factors and assess item factor loadings. It was done using robust-weighted least-squares estimator given the ordinal nature of the survey items, chi-square test statistic, and geomin oblique rotation (DeVellis, Citation2016). Cattell’s scree test on the sedimentation graph was examined. The number of factors was chosen based on the scree plot (eigenvalues), model adequacy, and overall interpretability. One to three factors structures were tested given that the original factor structure included three correlated factors as reported in (Smolenski et al., Citation2010). However, as highlighted by authors in their discussion, additional items would need to be added to the two factors that have only two items each. In the present study, we did not attempt to include new items, meaning that artificial restrictions would need to be placed on the structure to avoid identification problems in CFA.
CFA was performed to confirm the factor structure of the RHS using the second half of Sample 2 and Sample 1. The CFA used a weighted least-squares estimator with a diagonal weight matrix, robust standard errors, and a mean- and variance-adjusted chi-square statistic with delta parameterization (Muthen & Muthen, Citation2020). Modification indices were used to identify pairs of items for which model fit would improve if error estimates were freed to covary. Error terms were only freed to covary if there were theoretical reasons to believe they would covary (McDonald & Ho, Citation2002).
To assess model fit, the chi-square test, Tucker–Lewis Index (TLI) (Tucker & Lewis, Citation1973), Comparative Fit Index (CFI) (Bentler, Citation1990), Root Mean Square Error of Approximation (RMSEA) (Steiger, Citation1990) and Standardized Root Mean Residual (SRMR) (Bentler, Citation1990) were used. Since the chi-square test is highly sensitive to sample size, it can lead to the rejection of well-fitting models (Reise et al., Citation1993). Therefore, the TLI, CFI and RMSEA fit indices were emphasized. Good fitting models are indicated by a TLI and CFI≥0.95, RMSEA≤0.06 and SRMR<0.08 (Hu & Bentler, Citation1999).
Reliability
We assessed internal consistency using Cronbach’s alpha. Values ≥0.7 were considered acceptable, although Cronbach’s values are very sensitive to the number of items in the scale (Pallant, Citation2011).
Validity
We used independent samples t-tests to assess the criterion validity via associations between the RHS scores and study variables. As evidence for criterion validity, we hypothesized that men with higher IH would be less likely to identify as gay and to report having had sex with men in the past six months (Smolenski et al., Citation2010). As evidence for construct validity, based on prior studies, we hypothesized that men scoring higher in IH would be less likely to have tested for HIV (Matthews et al., Citation2019; Sun et al., Citation2020; M W Ross et al., Citation2013), and to have used PrEP (Meanley et al., Citation2020; Melendez-Melendez-Torres et al., Citation2020). With regard to sexual behavior, studies have shown that IH was associated with a set of health problems among gay and bisexual men including sexual compulsivity (Herrick et al., Citation2013), the co-occurrence of negative psychosocial health conditions that included sexual compulsivity (Dew & Chaney, Citation2005), and HIV infection (Shoptaw et al., Citation2009). Nevertheless, a systematic review of the published and gray literature suggested that although engagement in high-risk sexual behavior has been associated with higher IH in the past, this bivariate association has likely diminished over time (Newcomb & Mustanski, Citation2011). As such, we hypothesized that IH would be uncorrelated with engagement in condomless receptive anal sex. Furthermore, other studies have explored possible moderators of the association between engagement high-risk behavior and IH and found that year of data collection was a significant moderator suggesting, at least in some countries, increased acceptance of SGM identities over the past decades. This line of reasoning could suggest a cohort effect with younger generations having lower IH. Thus, we hypothesized GBM ≤24 years of age would have lower IH scores compared to those aged >24 years.
The EFA and CFA were carried out in Mplus version 8.4 (Muthen & Muthen, Citation2020), and all other analyses were performed in R version 4.0.1 (https://www.r-project.org/).
Results
Translation
The qualitative pretesting of the final translated version was conducted with a small convenience sample of GBM (N = 80); most were aged ≥25 years (79%), had finished college or higher education (74%), and lived in the city of Rio de Janeiro (69%). Between 87% and 95% of participants rated the clarity of each item as 7 or higher, with mean clarity scores ranging from 9.3 for items 3 and 7 to 9.7 for item 1. Items 3 and 7 were slightly modified as a function of the suggestions made by participants. The post-pretesting version of the translated scale is provided in .
Sample 1 characteristics
During October-2019, a total of 1186 participants accessed the questionnaire through Grindr, and 880(74%) cisgender GBM completed it. Of these, 218 were randomized to complete the translated version of the RHS (Sample 1, ). Median age was 33 years (interquartile range [IQR]:26–40) and most of respondents self-identified as gay (N = 158;73%); other sexual orientation including bisexual (N = 57;26%) and heterosexual (3;1%). The majority self-reported HIV negative status (N = 162;74%), and almost 20% had HIV unknown status ().
Table 2. Characteristics of study population: sample 1 from October 2019 and sample 2 from February to March 2020
Sample 2 characteristics
During February and March 2020, a total of 10,708 participants accessed the questionnaire through Hornet. Of these, 5355 cisgender men who self-identified as gay completed the questionnaire (Sample 2, ). Median age was 34 years (IQR:28–41), 30% (N = 1587) self-reported HIV positive status. Among those self-reporting negative or unknown status, 86% (N = 3212) had never used PrEP. Of these, the majority reported sex with men (N = 3029; 94%), and 39% (N = 1264) reported condomless receptive anal sex, both in the prior 6 months ().
Exploratory factor analysis
Random splitting of Sample 2 yielded two halves of size N = 2652 (Development) and N = 2683 (Validation) which were used, respectively, for the EFA and CFA. Mean (SD) of item scores ranged from 0.9 (1.6) to 1.8 (1.8) ().
Table 3. Exploratory and confirmatory factor analyses for the reactions to homosexuality scale
The EFA of the 7-items RHS yielded two eigenvalues greater than one (Factor 1 eigenvalue 3.5 and Factor 2 eigenvalue 1.1). Based on examination of the scree plot (Supplementary Figure 1) and item factor loadings, we judged that a one-factor solution provided the most interpretable model. The two-factor model grouped items 1 and 2 in one factor and all other items into a second factor (inter-factor correlation = 0.53). This grouping was not readily interpretable and included a factor measured by only two items. Model fit for the one-factor solution was suboptimal based on all indices (χ2(14) = 1373.1, p < 0.001; CFI = 0.89; TLI = 0.84; RMSEA = 0.19; SRMS = 0.09).
Confirmatory factor analysis
Initially, a one-factor structure showed moderate fit for the Sample 2 – Validation sample (): χ2(14) = 1130.3, p < 0.001; CFI = 0.91; TLI = 0.86; RMSEA = 0.17: SRMR = 0.05. The item loadings ranged from 0.553 (item 2) to 0.796 (item 5). Inspection of modification indices indicated that freeing error terms to covary could substantially improve model fit. While considering item’s content and interpretation, error terms for items 1 and 2 and for items 3 and 4 were allowed to covary and new model fit indices were good: χ2(12) = 309.1, p < .001; CFI = 0.98; TLI = 0.96; RMSEA = 0.09; SRMR = 0.02.
A one-factor structure showed good fit for Sample 1 (): χ2(14) = 66.8, p < .001; CFI = 0.96; TLI = 0.93; RMSEA = 0.13; SRMR = 0.03. Again, freeing errors terms for items 1 and 2 and for items 3 and 4 to covary improved model fit substantially: χ2(12) = 22.0, p = 0.037; CFI = 0.99; TLI = 0.98; RMSEA = 0.06; SRMR = 0.02.
Reliability
The internal consistency reliability of the total scale in the two-halves of Sample 2 and in Sample 1 were, respectively, 0.77, 0.76, and 0.81, which is in line with what was reported in the original publication (Smolenski et al., Citation2010).
Validity
Mean comparisons using t-tests () for the two dichotomous criterion variables were consistent with our hypotheses. Men who did not self-identify as gay and who reported not having sex with men in the past 6 months scored significantly higher, indicating higher IH.
Table 4. Mean (standard deviation) scores for the reactions to homosexuality scale as a function of characteristics of the study population
Similarly, when assessing construct validity, mean comparisons’ results for three of the four variables were consistent with our hypotheses. Younger respondents from Sample 2 scored lower than those aged >24 years indicating lower IH and respondents who never tested for HIV scored higher than who had tested for HIV indicating higher IH. Additionally, respondents who never used PrEP scored higher than those who used PrEP indicating higher IH. Contrary to our hypothesis of no correlation between engagement in high-risk sexual behavior and IH, results showed that those who did not engage in high-risk sexual behavior had higher scores indicating higher IH.
Discussion
In this study, we successfully performed the translation, validation and reliability of the RHS in Brazilian Portuguese. EFA and CFA results showed that the one-factor structure of the scale had adequate fit. Associations between scale scores and gay-only sexual orientation and sex with men in the past 6 months suggested criterion validity, whereas lower scores (lower IH) among those aged 18–24 years, who had tested for HIV or ever used PrEP suggest construct validity. Our results thus confirm the validity of the RHS and its applicability among Brazilian GBM.
Adequate fitting models, as indicated by TLI, CFI, RMSEA and SRMR indices, were obtained for the two samples after allowing some error terms to covary (Hu & Bentler, Citation1999). Internal consistency was suggested for the IH overall score. Adequate cut-off values for alpha are questionable (Lance et al., Citation2006), and may be influenced by the low number of items in the scale (Pallant, Citation2011). To allow for current and future comparisons, items in the Brazilian Portuguese version were maintained as proposed in the original version (Smolenski et al., Citation2010). In addition, factor loadings for all scale items were mostly acceptable (Matsunaga, Citation2010).
GBM self-identifying gay scored lower in comparison to GBM of other sexual orientations, as also observed in the scale validation study (Smolenski et al., Citation2010), in a multi-country survey using the same scale (Berg et al., Citation2015) and when a different scale to measure IH was used (Chard et al., Citation2015). We hypothesize that GBM using apps to find male sexual partners possibly self-identify as heterosexual or bisexual as a reflection of our conservative, paternalistic and homophobic society instead of real sexual attraction. Although this result is of importance for the concurrent validity of Brazilian Portuguese version of the RHS, this association should be confirmed by larger studies and be interpreted with caution to avoid stigmatization of other SGM.
Corroborating prior studies, GBM who never tested for HIV and never used PrEP had higher IH than those who previously tested for HIV or used PrEP (Matthews et al., Citation2019; Meanley et al., Citation2020; Sun et al., Citation2020; M W Ross et al., Citation2013). These results are important as they indicate that IH may prevent GBM from accessing HIV prevention technologies and may jeopardize PrEP scale up in this population (Golub, Citation2018). Decreasing social stigma and IH towards SGM is paramount to reach the WHO fast-track target to end HIV epidemic by 2030 in Brazil (UNAIDS, Citation2020).
Contrary to data from Europe and Uganda (M W Ross et al., Citation2013, Citation2013), our results showed that men engaging in condomless receptive anal sex had lower IH than those who did not report this behavior. In Uganda, where homophobia is likely higher than in Brazil, the authors hypothesized that anal sex may establish or enhance a view of oneself as homosexual, and the individual would be more likely to internalize anti-homosexual attitudes (M W Ross et al., Citation2013). Here, it is important to highlight some characteristics of our sample population: gay man, mostly white, educated and from South/Southeast Brazil. Indeed, 36% of them resided in São Paulo, a city that has held the Guinness title for having the largest gay parade in the world (between 2006 and 2016) (Wikipedia, Citation2020). Thus, though not reflective of contemporary Brazil as a whole, acceptability of SGM populations is high in large urban centers despite the current conservative government (Poushter et al., Citation2020). Nevertheless, additional analyses are necessary to draw final conclusions, as prior multivariate analyses have failed to find a direct bivariate relationship between IH and engagement in high-risk sexual behavior (Newcomb & Mustanski, Citation2011).
Different from prior studies, younger GBM had lower IH than older peers (Berg et al., Citation2015; Cox et al., Citation2010). According to some authors, the effects of IH may be more intensely felt early in the coming-out process, and this may explain the previous findings (Huebner et al., Citation2002; Meyer, Citation1995). However, with higher acceptability of SGM identities, coming-out processes are happening earlier, before 18 years-old. This is an important result with regard to the current trends in the HIV epidemic in Brazil. HIV prevalence among young MSM has been rising in Brazil (Coelho et al., Citation2020) and this may be related to higher engagement in high-risk behavior, lower risk perception and lower awareness of PrEP among young GBM (Torres, Luz et al., Citation2019). Our findings thus suggest that lower IH among young GBM could mean greater receptivity to receive information about HIV prevention, indicating that HIV prevention campaigns could be tailored specifically for this population.
This study has limitations. Although our sample is restricted to users of apps, we were able to reach a plurality of Brazilian GBM. In the present analysis, we defined engagement in high-risk behavior solely by the report of condomless receptive anal sex in prior six months though other definitions are possible and the association of IH with sexual behavior may differ depending on definition. A good proportion of recruited GBM had lower education and lower income, a reflection of the availability of cellphones and internet connection in all socioeconomic strata of the Brazilian population (CGIBR, Citation2020) Additionally, the inclusion of participants with different HIV self-reported status and having or not a steady partner corroborates the applicability of RHS to GBM with different characteristics and perceptions.
The RHS was effectively translated and validated to Brazilian Portuguese. This instrument has shown to be practical and easy to administer. Future studies should evaluate the role of IH on GBM’s physical and mental health and well-being, as well as its impact on the uptake of HIV prevention technologies.
Conflicts of interest
No potential conflict of interest was reported by the author(s).
Supplemental Material
Download MS Word (51 KB)Supplementary material
Supplemental data for this article can be accessed here.
Additional information
Funding
References
- Altman, D., Aggleton, P., Williams, M., Kong, T., Reddy, V., Harrad, D., Reis, T., & Parker, R. (2012). Men who have sex with men: Stigma and discrimination. The Lancet, 380(9839), 439–445. https://doi.org/10.1016/S0140-6736(12)60920-9
- Beaton, D. E., Bombardier, C., Guillemin, F., & Ferraz, M. B. (2000). Guidelines for the process of Cross-Cultural adaptation of Self-Report measures. Spine, 25(24), 3186–3191. https://doi.org/10.1097/00007632-200012150-00014
- Bentler, P. M. (1990). Comparative fit indexes in structural models. Psychological Bulletin, 107(2), 238–246. https://doi.org/10.1037/0033-2909.107.2.238
- Berg, R. C., Munthe-Kaas, H. M., & Ross, M. W. (2016). Internalized homonegativity: A systematic mapping review of empirical research. Journal of Homosexuality, 63(4), 541–558. https://doi.org/10.1080/00918369.2015.1083788
- Berg, R. C., Weatherburn, P., Ross, M. W., & Schmidt, A. J. (2015). The relationship of internalized homonegativity to sexual health and well-being among men in 38 European Countries who have sex with men. Journal of Gay & Lesbian Mental Health, 19(3), 285–302. https://doi.org/10.1080/19359705.2015.1024375
- Bilal, U., Alazraqui, M., Caiaffa, W. T., Lopez-Olmedo, N., Martinez-Folgar, K., Miranda, J. J., Rodriguez, D. A., Vives, A., & Diez-Roux, A. V. (2019). Inequalities in life expectancy in six large Latin American cities from the SALURBAL study: An ecological analysis. The Lancet Planetary Health, 3(12), e503–e510. https://doi.org/10.1016/S2542-5196(19)30235-9
- Chard, A. N., Finneran, C., Sullivan, P. S., & Stephenson, R. (2015). Experiences of homophobia among gay and bisexual men: Results from a cross-sectional study in seven countries. Culture, Health & Sexuality, 17(10), 1174–1189. https://doi.org/10.1080/13691058.2015.1042917
- Comitê Gestor da Internet no Brasil (CGIBR). (2020, June 4). J2—INDIVÍDUOS QUE POSSUEM TELEFONE CELULAR 2019. https://cetic.br/pt/tics/domicilios/2019/individuos/J2
- Cox, N., Dewaele, A., Van Houtte, M., & Vincke, J. (2010). Stress-Related growth, coming out, and internalized homonegativity in lesbian, gay, and bisexual youth. An examination of Stress-Related growth within the minority stress model. Journal of Homosexuality, 58(1), 117–137. https://doi.org/10.1080/00918369.2011.533631
- Currie, M. R., Cunningham, E. G., & Findlay, B. M. (2004). The Short Internalized Homonegativity Scale: Examination of the Factorial Structure of a New Measure of Internalized Homophobia. Educational and Psychological Measurement, 64(6), 1053–1067. https://doi.org/10.1177/0013164404264845
- DeVellis, R. F. (2016). Scale Development. Theory and Applications (4th ed.). Leonard Bickman and Debra J. Rog.
- Dew, B. J., & Chaney, M. P. (2005). The relationship among sexual compulsivity, internalized homophobia, and HIV At-Risk sexual behavior in gay and bisexual male users of internet chat rooms. Sexual Addiction & Compulsivity, 12(4), 259–273. https://doi.org/10.1080/10720160500362306
- Goffman, E. (1990). Stigma: Notes on the management of spoiled identity. Penguin.
- Golub, S. A. (2018). PrEP Stigma: Implicit and explicit drivers of disparity. Current HIV/AIDS Reports, 15(2), 190–197. https://doi.org/10.1007/s11904-018-0385-0
- Grupo Gay Bahia. (2020). RELATÓRIOS ANUAIS DE MORTES LGBTI+. Retrieved May 4, 2020, from https://grupogaydabahia.com.br/relatorios-anuais-de-morte-de-lgbti/
- Coelho, L.E., Torres, T.S., Veloso, V.G., Grinsztejn, B., Jalil, E.M., Wilson, E.C., McFarland, W. The Prevalence of HIV Among Men Who Have Sex With Men (MSM) and Young MSM in Latin America and the Caribbean: A Systematic Review. AIDS Behav. 2021 Feb 15. doi: 10.1007/s10461-021-03180-5. Epub ahead of print.
- Herek, G. M. (2000). The Psychology of Sexual Prejudice. Current Directions in Psychological Science, 9(1), 19–22. https://doi.org/10.1111/1467-8721.00051
- Herek, G. M. (2007). Confronting sexual stigma and prejudice: Theory and Practice: Confronting sexual stigma and prejudice. Journal of Social Issues, 63(4), 905–925. https://doi.org/10.1111/j.1540-4560.2007.00544.x
- Herrick, A. L., Lim, S. H., Plankey, M. W., Chmiel, J. S., Guadamuz, T. T., Kao, U., Shoptaw, S., Carrico, A., Ostrow, D., & Stall, R. (2013). Adversity and syndemic production among men participating in the multicenter AIDS cohort study: A Life-Course approach. American Journal of Public Health, 103(1), 79–85. https://doi.org/10.2105/AJPH.2012.300810
- Hu, L., & Bentler, P. M. (1999). Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Structural Equation Modeling: A Multidisciplinary Journal, 6(1), 1–55. https://doi.org/10.1080/10705519909540118
- Huebner, D. M., Davis, M. C., Nemeroff, C. J., & Aiken, L. S. The impact of internalized homophobia on HIV preventive interventions. (2002). American Journal of Community Psychology, 30(3), 327–348. https://doi.org/10.1023/A:1015325303002
- Jeffries, W. L., & Johnson, O. D. (2018). Internalized homonegativity and substance use among U.S. Men Who Have Sex with Men Only (MSMO) and Men who Have sex with men and Women (MSMW). Substance Use & Misuse, 53(4), 559–564. https://doi.org/10.1080/10826084.2017.1347185
- Kerr, L., Kendall, C., Guimarães, M. D. C., Salani Mota, R., Veras, M. A., Dourado, I., De Brito, M., Merchan-Hamann, A., Pontes, E., Leal, A. K., Knauth, A. F., Castro, D., Macena, A. R. C. M., Lima, R. H. M., Oliveira, L. N. C., Cavalcantee, L. C., Do S., M., Benzaken, A. S., Pereira, G., Pimenta, C., & Johnston, L. G. (2018). HIV prevalence among men who have sex with men in Brazil: Results of the 2nd national survey using respondent-driven sampling. Medicine, 97(1S), S9–S15. https://doi.org/10.1097/MD.0000000000010573
- Lamontagne, E., d’Elbée, M., Ross, M. W., Carroll, A., Du, P. A., & Loures, L. (2018). A socioecological measurement of homophobia for all countries and its public health impact. European Journal of Public Health, 28(5), 967–972. https://doi.org/10.1093/eurpub/cky023
- Lance, C. E., Butts, M. M., & Michels, L. C. (2006). The sources of four commonly reported cutoff criteria: What did they really say? Organizational Research Methods, 9(2), 202–220. https://doi.org/10.1177/1094428105284919
- Luz, P. M., Torres, T. S., Almeida-Brasil, C. C., Marins, L. M. S., Bezerra, D. R. B., Veloso, V. G., Grinsztejn, B., Harel, D., & Thombs, B. D. (2020). Translation and validation of the Short HIV Stigma scale in Brazilian Portuguese. Health and Quality of Life Outcomes, 18(1), 322. https://doi.org/10.1186/s12955-020-01571-1
- Luz, P. M., Veloso, V. G., & Grinsztejn, B. (2019). The HIV epidemic in Latin America: Accomplishments and challenges on treatment and prevention. Current Opinion in HIV and AIDS, 14(5):366-373. https://doi.org/10.1097/COH.0000000000000564
- Matsunaga, M. (2010). How to factor-analyze your data right: Do’s, don’ts, and how-to’s. International Journal of Psychological Research, 3(1), 97–110. https://doi.org/10.21500/20112084.854
- Matthews, D. D., Sang, J. M., Chandler, C. J., Bukowski, L. A., Friedman, M. R., Eaton, L. A., & Stall, R. D. (2019). Black men who have sex with men and lifetime hiv testing: characterizing the reasons and consequences of having never tested for HIV. Prevention Science, 20(7), 1098–1102. https://doi.org/10.1007/s11121-019-01022-4
- McDonald, R. P., & Ho, M.-H. R. (2002). Principles and practice in reporting structural equation analyses. Psychological Methods, 7(1), 64–82. https://doi.org/10.1037/1082-989X.7.1.64
- Meanley, S., Chandler, C., Jaiswal, J., Flores, D. D., Stevens, R., Connochie, D., & Bauermeister, J. A. (2020). Are sexual minority stressors associated with young men who have sex with men’s (YMSM) level of engagement in PrEP? Behavioral Medicine, 1–11. https://doi.org/10.1080/08964289.2020.1731675
- Melendez-Torres, G. J., Noori, T., Pharris, A., Spiteri, G., Garner, A., Alba, B., & Bourne, A. (2020). Country level homophobia and protective sexual health behaviours among HIV negative or untested men who have sex with men in 45 countries. AIDS Care, 32(12), 1–5. https://doi.org/10.1080/09540121.2020.1766662
- Meyer, I. H. (1995). Minority stress and mental health in gay men. Journal of Health and Social Behavior, 36(1), 38. https://doi.org/10.2307/2137286
- Meyer, I. H. (2003). Prejudice, social stress, and mental health in lesbian, gay, and bisexual populations: Conceptual issues and research evidence. Psychological Bulletin, 129(5), 674–697. https://doi.org/10.1037/0033-2909.129.5.674
- Muthen, L. K., & Muthen, B. O. (2020). Mplus statistical analysis with latent variables. User’s Guide. Los Angeles, CA: Muthén & Muthén. https://www.statmodel.com/download/usersguide/MplusUserGuideVer_8.pdf
- Newcomb, M. E., & Mustanski, B. (2010). Internalized homophobia and internalizing mental health problems: A meta-analytic review. Clinical Psychology Review, 30(8), 1019–1029. https://doi.org/10.1016/j.cpr.2010.07.003
- Newcomb, M. E., & Mustanski, B. (2011). Moderators of the Relationship between internalized homophobia and risky sexual behavior in Men Who Have Sex with Men: A Meta-Analysis. Archives of Sexual Behavior, 40(1), 189–199. https://doi.org/10.1007/s10508-009-9573-8
- Pallant, J. (2011). SPSS survival manual: A step by step guide to data analysis using SPSS (Vol. 4th). Open University Press/McGraw-Hill.
- Pereira, H., & Leal, I. P. (2005). Medindo a homofobia internalizada: A validação de um instrumento. Analise Psicologica, 23(3), 323–328. 10.14417/ap.96
- Poushter, J., Kent, N. O., & Center, P. R. (2020, August 3). The global divide on homosexuality persists but increasing acceptance in many countries over past two decades. Pew Research Center. https://www.pewresearch.org/global/2020/06/25/global-divide-on-homosexuality-persists
- Reise, S. P., Widaman, K. F., & Pugh, R. H. (1993). Confirmatory factor analysis and item response theory: Two approaches for exploring measurement invariance. Psychological Bulletin, 114(3), 552–566. https://doi.org/10.1037/0033-2909.114.3.552
- Ross, M. W., Berg, R. C., Schmidt, A. J., Hospers, H. J., Breveglieri, M., Furegato, M., & Weatherburn, P. (2013). Internalised homonegativity predicts HIV-associated risk behavior in European men who have sex with men in a 38-country cross-sectional study: Some public health implications of homophobia. BMJ Open, 3(2), e001928. https://doi.org/10.1136/bmjopen-2012-001928
- Ross, M. W., Kajubi, P., Mandel, J. S., McFarland, W., & Raymond, H. F. (2013). Internalized homonegativity/homophobia is associated with HIV-risk behaviours among Ugandan gay and bisexual men. International Journal of STD & AIDS, 24(5), 409–413. https://doi.org/10.1177/0956462412472793
- Ross, M. W., & Rosser, B. R. (1996). Measurement and correlates of internalized homophobia: A factor analytic study. Journal of Clinical Psychology, 52(1), 15–21. https://doi.org/10.1002/(SICI)1097-4679(199601)52:1<15::AID-JCLP2>3.0.CO;2-V
- Sabidó, M., Kerr, L. R. F. S., Mota, R. S., Benzaken, A. S., Guimaraes, M. D. C., Kendall, C., Kendall, C., Kendall, C., & Kendall, C., . . (2015). Sexual violence against Men Who Have Sex with Men in Brazil: A respondent-driven sampling survey. AIDS and Behavior, 19(9), 1630–1641. https://doi.org/10.1007/s10461-015-1016-z.
- Shidlo, A. (1994). Internalized Homophobia: Conceptual and Empirical Issues in Measurement. In B. Greene & G. Herek (Eds.), Lesbian and gay psychology: Theory, research, and clinical applications (pp. 176–205). SAGE Publications, Inc. https://doi.org/10.4135/9781483326757.n10
- Shoptaw, S., Weiss, R. E., Munjas, B., Hucks-Ortiz, C., Young, S. D., Larkins, S., Victorianne, G. D., & Gorbach, P. M. (2009). Homonegativity, substance use, sexual risk behaviors, and HIV status in poor and ethnic Men Who Have Sex with Men in Los Angeles. Journal of Urban Health, 86(S1), 77–92. https://doi.org/10.1007/s11524-009-9372-5
- Smolenski, D. J., Diamond, P. M., Ross, M. W., & Rosser, B. R. S. (2010). Revision, criterion validity, and multigroup assessment of the reactions to homosexuality scale. Journal of Personality Assessment, 92(6), 568–576. https://doi.org/10.1080/00223891.2010.513300
- Steiger, J. H. (1990). Structural model evaluation and modification: An interval estimation approach. Multivariate Behavioral Research, 25(2), 173–180. https://doi.org/10.1207/s15327906mbr2502_4
- Sun, S., Whiteley, L., & Brown, L. K. (2020). HIV testing among Chinese Men Who Have Sex with Men: The roles of HIV knowledge, online social life, and sexual identity concerns. AIDS and Behavior, 24(2), 437–449. https://doi.org/10.1007/s10461-019-02471-2
- Torres, T. S., Bastos, L. S., Kamel, L., Bezerra, D. R. B., Fernandes, N. M., Moreira, R. I., Garner, A., Veloso, V. G., Grinsztejn, B., & De Boni, R. B. (2020). Do men who have sex with men who report alcohol and illicit drug use before/during sex (chemsex) present moderate/high risk for substance use disorders? Drug and Alcohol Dependence, 209(107908). https://doi.org/10.1016/j.drugalcdep.2020.107908
- Torres, T. S., Luz, P. M., De Boni, R. B., De Vasconcellos, M. T. L., Hoagland, B., Garner, A., Moreira, R. I., Veloso, V. G., & Grinsztejn, B. (2019). Factors associated with PrEP awareness according to age and willingness to use HIV prevention technologies: The 2017 online survey among MSM in Brazil. AIDS Care, 31(10), 1193–1202. https://doi.org/10.1080/09540121.2019.1619665
- Torres, T. S., Luz, P. M., Marins, L. M. S., Bezerra, D. R. B., Almeida-Brasil, C. C., Veloso, V. G., Grinsztejn, B., Harel, D., & Thombs, B. D. (2021). Cross-cultural adaptation of the Perceived risk of HIV scale in Brazilian Portuguese. Health and Quality of Life Outcomes, 19(1), 117. https://doi.org/10.1186/s12955-021-01760-6
- Torres, T. S., Marins, L. M. S., Veloso, V. G., Grinsztejn, B., & Luz, P. M. (2019). How heterogeneous are MSM from Brazilian cities? An analysis of sexual behavior and perceived risk and a description of trends in awareness and willingness to use pre-exposure prophylaxis. BMC Infectious Diseases, 19(1), 1067. https://doi.org/10.1186/s12879-019-4704-x
- Tran, H., Ross, M. W., Diamond, P. M., Berg, R. C., Weatherburn, P., & Schmidt, A. J. (2018). Structural validation and multiple group assessment of the short internalized homonegativity scale in homosexual and bisexual men in 38 European Countries: Results from the European MSM internet survey. The Journal of Sex Research, 55(4–5), 617–629. https://doi.org/10.1080/00224499.2017.1380158
- Tucker, L. R., & Lewis, C. (1973). A reliability coefficient for maximum likelihood factor analysis. Psychometrika, 38(1), 1–10. https://doi.org/10.1007/BF02291170
- Turpin, R. E., Dyer, T. V., Dangerfield, D. T., Liu, H., & Mayer, K. H. (2020). Syndemic latent transition analysis in the HPTN 061 cohort: Prospective interactions between trauma, mental health, social support, and substance use. Drug and Alcohol Dependence, 214(108106). https://doi.org/10.1016/j.drugalcdep.2020.108106
- UNAIDS. (2020, July 31). Understanding fast-track accelerating action to end the AIDS epidemic by 2030. https://www.unaids.org/sites/default/files/media_asset/201506_JC2743_Understanding_FastTrack_en.pdf
- Wikipedia. (2020, August 10). https://en.wikipedia.org/wiki/S%C3%A3o_Paulo_Gay_Pride_Parade