Abstract
Anti-pathogen adoptive T-cell immunotherapy has been proven to be highly effective in preventing or controlling viral infections following hematopoietic stem cell transplantation. Recent advances in manufacturing protocols allow an increased number of targeted pathogens, eliminate the need for viral transduction, broaden the potential donor pool to include pathogen-naïve sources, and reduce the time requirement for production. Early studies suggest that anti-fungal immunotherapy may also have clinical benefit. Future advances include further broadening of the pathogens that can be targeted and development of T-cells with resistance to pharmacologic immunosuppression.
Introduction
Since the advent of hematopoietic stem cell transplantation (HSCT), infections have remained a leading cause of morbidity and mortality in patients.Citation1–Citation4 Although advances in prophylactic therapy have reduced the early burden of viral and fungal infections, therapeutic options for breakthrough infections are complicated by toxicities, and for many viral infections there are no effective treatments.Citation5–Citation9 It has been well established that T-cell reconstitution is the most important factor in preventing viral infection following HSCT, and factors that influence the speed of T-cell recovery also impact the risk of viral infection in this period.Citation2,Citation3 As transplantation protocols have progressed to allow an increasing number of donor sources for transplantation, clinicians have had to balance the risks of graft versus host disease (GVHD) when using a T-cell replete graft versus delayed T-cell engraftment when using T-cell depletion or a naïve donor source such as cord blood.Citation10,Citation11
Given the importance of T-cells to antiviral immunity, use of donor lymphocyte infusions from the stem cell donor was discovered to be an effective salvage therapy for viral infections in HSCT recipients prior to T-cell recovery.Citation12 However, the high rate of potentially fatal GVHD has relegated this treatment to a course of last resort. However, subsequent advances in immunobiology and culturing techniques have permitted great progress in improving the safety and efficacy of cytotoxic T-lymphocyte (CTL) immunotherapy following HSCT. These include: an improved knowledge of conserved T-cell epitopes for various pathogens,Citation13–Citation15 improvements in ex vivo culture of T-cells and antigen-presenting cells,Citation16–Citation18 and rapid tests to evaluate the effector function and major histocompatibility complex (MHC) restriction of T-cells.Citation19,Citation20 In essence, CTL therapy allows clinicians to bypass the months required for T-cell engraftment and a subsequent primary immune response to a pathogen.
Although trials utilizing antiviral CTLs represent the bulk of the studies to date, preclinical studies and early clinical trials of antifungal CTLs have also shown promise. Adoptive immunotherapy targeting tumor targets is also a burgeoning field, and has recently been reviewed.Citation21 In this review, we summarize the methodologies and results of recent and current trials of anti-pathogen CTL therapy, and recap recent preclinical advances that provide the framework for future CTL clinical studies.
Methodologies of CTL production
In CTL production protocols to date, two concepts are essential, ie, harnessing pathogen-specific T-cells, and the exclusion of alloreactive T-cells. This has been accomplished previously by either direct selection of donor cells, or stimulation and ex vivo culture of donor T-cells from peripheral blood mononuclear cells (PBMCs).
Direct selection relies on cell sorting of donor PBMCs, usually after a short stimulation with the antigen of interest.Citation22 Selection can be achieved via multimer selection (selecting for T-cells with a T-cell receptor of known antigen specificity), or by column selection of interferon-gamma-producing T-cells following a brief stimulation with an antigen of interest (). It has the advantage of a minimal time requirement for product manufacturing, and uses existing Good Manufacturing Practice-compliant sorting technologies. However, this technique requires leukapheresis of donors in order to collect sufficient cells for clinical use. Additionally, it requires that there be detectable pathogen-specific T-cells in the periphery, and thus it would not be a viable option for manufacturing of CTLs from pathogen-naïve donors nor for pathogens that induce a poor memory response. Multimer selection has the disadvantage of selecting only CD8+ T-cells of limited specificity and MHC restriction, which could allow pathogen evasion and possibly impair CTL persistence.Citation23 Additionally, previous studies have suggested that residual binding of multimers may impact T-cell function in vitro,Citation24 although the clinical impact of this effect is unclear. The recent development of reversible streptamer technology for selection bypasses this potential risk.Citation25 Interferon-gamma selection allows inclusion of polyclonal antigen-specific CD4+ and CD8+ T-cells, and allows selection of a wider range of antigen-specific cells in the final product.
Figure 1 Current Good Manufacturing Practice-compliant approaches for generation of antipathogen CTL products.
Abbreviations: CTL, cytotoxic T-lymphocyte; IFN, interferon.
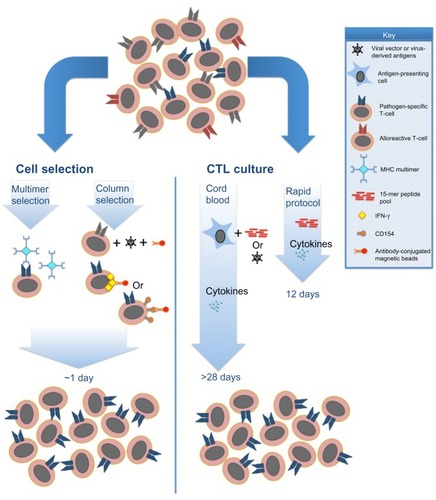
Alternatively, stimulation and ex vivo culture permits expansion of single or multiple pathogen-specific CTLs. Culture has several advantages over cell selection, including generation of polyclonal CTLs, and expansion of cells to clinically useful volumes from a small volume of blood.Citation26 These advantages come at the expense of the culture and processing time required for CTL stimulation and expansion, which can vary from 10 days to more than 3–4 weeks, depending on the donor source. Loss of the ability of cells to self-renew and impaired persistence in vivo has been a longstanding concern with the use of prolonged ex vivo culture and expansion.Citation27 However, clinical trials to date have demonstrated prolonged persistence in spite of ex vivo culture.Citation28 Additionally, studies have demonstrated that ex vivo culturing with pathogen-specific stimuli eliminates alloreactivity,Citation15 likely due to cell death or inability to compete with pathogen-specific T-cells, and residual alloreactivity in manufactured CTLs has been shown to be clinically insignificant.Citation29 Early trials of CTL therapy depended on the use of virus-infected antigen-presenting cells, such as cytomegalovirus (CMV) lysates, CMV-infected fibroblasts, or Epstein Barr virus (EBV)-lymphoblastoid cell lines as a stimulant for expansion of donor-derived memory T-cells.Citation30–Citation32 Subsequent knowledge of dominant and highly conserved antigens such as CMV-pp65 and Adenovirus (Adv) hexon and penton have permitted the replacement of live virus with antigen stimulation using either 15-mer peptide pools spanning viral proteins, or with transduction of DNA plasmids encoding viral antigens into antigen-presenting cells.Citation33,Citation34 New methods to rapidly grow and manipulate antigen-presenting cells have also enabled the use of a wider population of donors and targeting of a greater number of pathogens in a single CTL culture.Citation16,Citation35 Optimization of cytokine cocktails for CTL culture has also allowed improved yields and targeted cellular phenotypes. In the recent rapid CTL protocol, interleukin (IL)-4 and IL-7 were shown to produce CD4+ T-cells with a predominantly Th1 phenotype, whereas IL-2 and IL-15 seem to favor proliferation of natural killer cells at the expense of T-cells.Citation34 Finally, studies have shown that central memory T-cells (characterized by expression of chemokine receptors CCR7, CD62L, and CD45RA) have superior persistence in vivo following adoptive transfer, and may be the ideal cell population for adoptive immunotherapy.Citation36,Citation37 Consequently, studies using both selection and culture methods have demonstrated the development of central memory T-cells in the resulting CTL products.Citation25,Citation34
Clinical studies of anti-viral CTLs
Clinical studies utilizing cell selection
Cell selection has been used in several prior studies to treat patients following HSCT (). Cobbold et al published the first clinical report in which CD8+ CMV-specific CTLs were isolated via tetramer selection.Citation38 Complete or partial clinical responses were achieved in nine patients who received infusions, although there were limited data on long-term persistence of infused CTLs. Feuchtinger et al utilized interferon-gamma column selection (Gamma capture assay; Miltenyi Biotec GmbH, Bergisch Gladbach, Germany) to produce CMV-CTL, resulting in partial to complete responses in 15 of 18 patients who were given a single dose.Citation39 Peggs et al also used interferon-gamma selection to produce CMV-CTL, using either recombinant pp65 or an overlapping peptide pool of 15-mers covering the pp65 protein as stimulants.Citation40 They were successful in protecting seven patients who were prophylactically treated, while in vivo expansion of CMV-CTLs was detected in 11 patients infused who had detectable CMV.Citation40 Schmitt et al produced CMV-CTL from HSCT donors utilizing reversible streptamers with MHC-restricted pp65 peptides.Citation25 These products were used to successfully treat two patients who developed CMV reactivation during treatment of GVHD after HSCT.
Table 1 Previous clinical trials of pathogen-specific T-cell therapy
Fewer clinical studies have been performed using these techniques to produce Adv-specific or EBV-specific CTL. Feuchtinger et al successfully produced Adv CTL by interferon-gamma selection for treatment of nine patients with treatment-refractory Adv infections.Citation41 In vivo CTL expansion was demonstrated in five of six patients tested, and four patients had clearance of disease. Uhlin et al used human leukocyte antigen (HLA)-A2-specific pentamers to produce EBV-CTL from the haploidentical mother of a patient who underwent cord blood transplantation and subsequently developed EBV-induced post-transplant lymphoproliferative disease.Citation42 A complete clinical response was obtained following two doses of CTLs. Moosmann et al treated six patients with EBV-induced post-transplant lymphoproliferative disease with EBV-CTL developed by interferon-gamma selection, and achieved complete responses in three patients with early disease, but no response in three patients with advanced, multiorgan disease.Citation43 Of note, in all studies utilizing cell selection, no significant GVHD occurred, and clinical impacts were seen in spite of very low cell doses (<5×104 cells/kg in most studies).
Clinical studies utilizing cell culture
CTL production utilizing ex vivo cell culture has been the most common methodology to date, and accounts for the majority of patients treated in clinical trials of antipathogen adoptive immunotherapy () over the past decade. Walter et al were among the first to show that stimulation of donor PBMC by CMV extracts resulted in expansion of CMV-specific CTLs, which lost alloreactivity after several weeks of ex vivo culture but retained antiviral activity.Citation32 There have been many advancements in ex vivo CTL culture since then, which have decreased both the manufacturing time and cost. Early notable strides involved the culture and manipulation of antigen-presenting cells for CTL culture. Rooney et al successfully used irradiated EBV-lymphoblastoid cell lines (EBV-LCL) to generate EBV-specific CTL, which were effective as prophylaxis or treatment for EBV-induced post-transplant lymphoproliferative disease in 114 patients.Citation28,Citation31 Of note, the first 26 patients received gene-marked CTLs, and follow-up studies showed persistence of the gene-marked cells as long as 105 months following infusion.
The development of clinical grade Adv vector Ad5f35pp65, which contains immunodominant CMV antigen pp65, permitted transduction of either donor-derived dendritic cells or EBV-LCL for use as antigen-presenting cells for CTL culture. Leen et al used this strategy to produce triviral (CMV, EBV, Adv-specific) CTLs, which were utilized in a dose-escalation trial to treat 26 patients.Citation17 No adverse effects were seen at doses ranging from 5×106 to 1×108 cells/m2, and all patients were effectively protected against CMV, EBV, and Adv disease. However, although EBV-specific and CMV-specific CTLs showed persistence by interferon-gamma ELISPOT, Adv-specific CTLs were not detectable except in the setting of infection. A follow-up trial utilized Ad5f35-transduced EBV-LCL to produce EBV-specific and Adv-specific CTL, which were infused into 13 patients as prophylaxis or treatment of EBV and Adv following HSCT.Citation44 Although the products provided effective protection against EBV and Adv in vivo, Adv-specific CTLs were again not detectable except in the setting of Adv infection, suggesting that even at levels below the limits of detection by interferon-gamma ELISPOT, the Adv-specific CTL provided protection and was able to undergo expansion in the setting of viral infection. Ad5f35pp65-transduced dendritic cells were similarly used by Micklethwaite et al to produce CMV-specific and Adv-specific CTLs, which were clinically effective in 12 patients who received infusions following HSCT.Citation45 Only two subsequent episodes of CMV reactivation occurred in the setting of administration of prednisone at levels as low as 0.5 mg/kg/day. Blyth et al similarly treated 50 patients following HSCT with triviral (CMV, EBV, Adv-specific) CTLs which were derived by a mix of methods: ten were produced by pulsing donor dendritic cells with the HLA-A2-restricted CMV peptide NLVPMVATV and 40 were produced using Ad5f35pp65-transduced donor dendritic cells.Citation46 Only five of the 50 patients developed CMV reactivations following CTL infusions, and one of these five required antiviral pharmacotherapy after being treated with steroids for acute GVHD.
Further protocol advances have validated the use of 15-mer peptide pools encompassing immunodominant viral antigens in place of viral transduction of antigen-presenting cells, thus removing the potential safety and regulatory barriers associated with use of viral vectors.Citation33 The use of gas-permeable rapid-expansion (G-Rex) bioreactors has further simplified CTL culture.Citation47 Gerdemann et al combined these two advances to develop a rapid protocol that yields CTL at clinical volumes in 10–12 days, and provided effective antiviral protection in ten patients who were infused following HSCT.Citation34 The ongoing ARMS (Administration of Rapidly Generated Multivirus-Specific Cytotoxic T-Lymphocytes for the Prophylaxis and Treatment of EBV, CMV, Adv, human herpesvirus 6 [HHV6], and BK virus infections post Allogeneic Stem Cell Transplant; NCT01570283) study has further modified this rapid protocol to produce five virus-specific CTL from a monoculture.
Gerdemann et al have further modified the rapid CTL protocol by utilizing nucleofection of DNA plasmids containing viral epitopes into donor-derived dendritic cells.Citation48 The resulting CTL cultures showed antiviral activity in vitro by interferon-gamma ELISPOT and CrCitation51 cytotoxicity assays comparable with that of similar products derived via stimulation with 15-mer peptide pools for the same viral epitopes.
Adverse events following administration of ex vivo cultured CTL products in 381 infusions for 180 patients on 18 protocols were recently reviewed by the groups at Baylor College of Medicine.Citation49 Twenty-four mild adverse events were reported within 6 hours of infusion, with nausea and vomiting being most common, and 22 nonserious adverse events (fever, chills, nausea) occurring within 24 hours. No significant GVHD was attributable to CTL infusion. The only significant complications of CTL therapy have been rare reports of systemic inflammatory responses following EBV-CTL therapy in patients with bulky EBV+ lymphoma. Blyth et al reported that seven cases of acute GVHD occurred following CTL infusion, although some were attributable to corticosteroid weaning prior to CTL infusion, and additionally the authors noted that the degree of HLA mismatch was greater in patients who received CTL therapy versus controls.Citation46
Recent developments
Third-party CTL use, expanded viral targets, T-cell receptor gene transfer, and CTL manufacture from pathogen-naïve donors
Until recently, the selection or culture of antipathogen CTLs was dependent on the presence of pathogen-specific memory T-cells in donor blood. These protocols failed to help recipients of pathogen-naïve stem cell products, a population that has been well described to be at increased risk of viral infection following HSCT.
One answer to this problem is the use of “off-the-shelf ” CTLs derived from third-party donors. This approach has been successfully used in several prior studies.Citation50,Citation51 Barker et al successfully treated two patients with refractory EBV-induced post-transplant lymphoproliferative disease following cord blood transplantation with third-party EBV-specific CTLs.Citation50 Leen et al utilized a bank of 32 CTL lines with characterized activity against EBV, CMV, and Adv to identify matched lines for 50 patients with refractory viral infections.Citation51 These infusions resulted in antiviral responses in 74%, 78%, and 67% of those with CMV, Adv, and EBV, respectively. This represents a dramatic improvement from the standard therapy response rate in eight patients for whom a matched line could not be found, who had a response rate of 13% and a mortality rate of 75%. In spite of only partial HLA matching (1–4 loci), only two patients developed grade I GVHD. The lower rate of response against EBV relative to CMV and Adv may be reflective of a greater breadth of immunodominant epitopes that differ by MHC types, which complicates the task of selecting the ideal third-party line with both antiviral activity and proper MHC restriction.
Third-party CTL treatment has also been successful using selection methodology. Uhlin et al used pentamer selection to produce anti-viral CTL specific for CMV, EBV, or Adv from related third-party donors for six patients with refractory viral infections (four with CMV, and one each with EBV and Adv).Citation52 Five of six patients had partial or complete responses. Notably, an infant with severe combined immunodeficiency was treated prior to cord blood transplantation with CMV-CTL derived from her mother, with a ten-fold reduction in her CMV DNA level. Wy and Qasim used interferon-gamma selection to manufacture Adv-CTL from related third-party donors to treat two patients who underwent HSCT and subsequently developed Adv viremia.Citation53 Although treatment successfully cleared the Adv infection in one patient, she developed grade III skin and liver GVHD.Citation54 Curiously, cytogenetic studies of liver tissue showed infiltration with T-cells from the original HSCT donor but not the CTL donor. The authors postulated that this was due to a “bystander” effect of CTLs on the HSCT donor cells; however, such an effect has not been seen in larger trials utilizing third-party CTL therapy.
A small number of other viruses have been targeted via adoptive immunotherapy. John Cunningham virus (JCV) is an ubiquitous polyoma virus which can cause progressive multifocal leukoencephalopathy, a devastating neurologic disease, in patients who are profoundly immunocompromised, including recipients of HSCT or solid organ transplants and patients with advanced human immunodeficiency virus or primary immunodeficiency disorders. Balduzzi et al described the use of donor-derived JCV-specific CTL in a 14-year-old patient who developed progressive multifocal leukoencephalopathy in the setting of prolonged steroid treatment for GVHD following HSCT.Citation55 These CTL were manufactured using 15-mer peptide pools encompassing the JCV antigens VP1 and LT, and were cultured for 26 days. The patient received two doses of JCV-specific CTLs, and had a remarkable and sustained improvement, including clearance of JCV-DNA from the cerebrospinal fluid and substantial improvements in his neurologic status.
Although not a frequent problem following HSCT, human papillomavirus (HPV) is not an uncommon late complication of HSCT, particularly in patients treated for primary immunodeficiency disorders. HPV has also been evaluated in preclinical studies as a potential target for CTL therapy. Ramos et al have described the use of peptide pools spanning the HPV E6 and E7 proteins to generate HPV-specific CTLs from patients with oropharyngeal or cervical cancer, many of which arise due to HPV16 infection.Citation56 The resulting CTLs showed specific activity against HPV E6 and E7, and also showed antitumor activity against CaSki, an HPV16 cervical cancer cell line.
Several studies have explored the possibility of transducing CTL with a T-cell antigen receptor of known viral specificity.Citation57–Citation59 This offers a novel strategy to develop CTL from pathogen-naïve donors, but imposes the additional regulatory requirements of transgenic technology. Additionally, the use of a single antiviral T-cell antigen receptor may risk antigenic escape by the pathogen. Nonetheless, a current trial of transgenic CTL utilizing a retroviral vector with a CMV-specific T-cell antigen receptor is being conducted in the UK by Emma Morris (principal investigator).Citation60
An important landmark in the field of adoptive immunotherapy has been the successful development of virus-specific CTLs from virus-naïve donors. Hanley et al first demonstrated that CTL could be produced in a 20% fraction from cord blood using donor-derived dendritic cells and an EBV-lymphoblastoid cell line as antigen-presenting cells, and Ad5f35pp65 transduction as a source of CMV and Adv antigens.Citation16 The resulting cell lines had specific antiviral activity against CMV, EBV, and Adv in interferon-gamma ELISPOT analysis as well as CrCitation51 cytotoxicity assays, with no evidence of alloreactivity. Curiously, epitope mapping showed that the immunodominant epitopes recognized by cord blood-derived CTLs differed from CTLs manufactured from CMV-seropositive and EBV-seropositive adult donors, with the HLA-A2 restricted epitope NLVPMVATV notably absent in the cord blood-derived lines. Despite this finding, CTLs manufactured from cord blood have been used successfully in 12 cord blood transplant recipients to date in the ongoing ACTCAT (Safety, Toxicity and MTD of One Intravenous IV Injection of Donor CTLs Specific for CMV and Adenovirus; NCT00880789) trial.
Most recently, Hanley et al have successfully manufactured multiviral CTLs from CMV-naïve adult donors.Citation35 To do so, CMV-CTLs were produced from CD45RA+ naïve T-cells isolated via column selection, and stimulated by donor dendritic cells pulsed with CMV 15-mer peptide pools. Preclinical data suggest that they have similar antiviral activity, and the current MUSTAT (Multivirus-Specific Cytotoxic T-Lymphocytes for the Prophylaxis and Treatment of EBV, CMV, and Adenovirus Infections post Allogeneic Stem Cell Transplant; NCT01945814) trial will seek to compare the clinical efficacy of CTLs derived from CMV-seropositive versus CMV-naïve donors.
Anti-fungal CTLs
Fungal infections are a well described risk after HSCT. The importance of Th17 immunity in controlling Candida infections has been well demonstrated by forms of primary immunodeficiency such as Hyperimmunoglobulin E syndrome and chronic mucocutaneous candidiasis, as well as human immunodeficiency virus infection.Citation61,Citation62 The importance of T-cell immunity in defense against invasive aspergillosis and mucormycosis is less clear, while their ties to innate defense (most notably neutrophil function) are well established. Interestingly, a recent study of patients with chronic granulomatous disease showed that they have abundant Aspergillus-specific T-cells with increased interferon-gamma production compared with healthy controls.Citation63 Despite these uncertainties, fungal infections may be a valid target for treatment via adoptive immunotherapy after HSCT.
Several preclinical studies have been successful in developing CTLs with activity against Candida, Aspergillus, and Rhizopus species (). Beck et al successfully produced Aspergillus-specific CTLs by stimulation of PBMCs with antigens from Aspergillus extracts, followed by interferon-gamma selection and culture.Citation64 The resulting population was predominantly CD4+ memory (CD45RO+) cells, but demonstrated interferon-gamma production in response to several species of Aspergillus as well as Penicillium. The authors also showed that these T-cells enhanced hyphal damage by neutrophils and antigen-presenting cells in vitro. Tramsen et al similarly used interferon-gamma selection following stimulation with cellular extracts from Candida albicans, Aspergillus fumigatus, and Rhizopus oryzae to produce multifungal-specific CTL lines, which were also almost exclusively CD4+ CD45RO+ HLA-DR+.Citation65 These lines displayed pathogen-specific activation markers (interferon-gamma CD154, tumor necrosis factor-alpha) and also enhanced oxidative activity of neutrophils when coincubated with antigen and antigen-presenting cells and tested via the 123-dihydrorhodamine assay. Khanna et al described a novel selection method based on upregulation of CD154 to produce multipathogen-specific T-cells against CMV, EBV, Adv, Candida, and Aspergillus.Citation66 Donor PBMCs were incubated with peptide libraries from CMV-pp65, EBV-LMP2, Adv-Hexon, Candida MP65, and a 15-mer peptide from Aspergillus CRF1. Following 14 days of culture, the authors showed pathogen-specific interferon-gamma production, proliferation, and cytotoxicity in vitro. Although these results are intriguing, there are very limited data regarding the relative importance of MP65 and CRF1 in antifungal immunity.Citation67,Citation68
Table 2 Preclinical studies of novel antipathogen T-cell therapies
As of the time of this review, only one clinical trial of anti-fungal CTLs has been published. Perruccio et al developed CTLs via stimulation of donor PBMCs with inactivated conidia from A. fumigatus, followed by several weeks of culture, resulting in clonal CD4+ CTLs with anti-Aspergillus activity by interferon-gamma ELISPOT.Citation69 Clinical use of these lines in patients with pulmonary aspergillosis resulted in survival of eight of nine patients treated, compared with a survival rate of 7/13 in patients with aspergillosis who did not receive infusions. There was no difference in the length of antifungal therapy required for survivors in the two groups.
Although these studies are intriguing, several key issues require attention before anti-fungal CTL trials begin to catch up with their antiviral brethren. First, a better understanding of the immunodominant T-cell targets for various fungal species is needed. Second, standardized Good Manufacturing Practice-compliant fungal antigen sources are necessary to allow consistency and valid comparisons between future clinical trials.
Future of CTL therapy
Expanding the breadth of monoculture CTL lines: is there an antigen limit?
As manufacture of CTLs expands to include more pathogens in a single culture, the possibility of antigenic competition between the different pathogen-specific T-cells has caused many to question the limits of CTL monocultures. This concern has certainly been validated in attempts to produce multivirus-specific CTLs from donors who are CMV-naïve, in which the resulting culture is dominated by memory-derived EBV-specific and Adv-specific T-cells. Although the relative proportions of individual virus-specific CTLs decrease as the number of antigens increases, this has not seemed to impact the efficacy of these products in clinical trials. Recent studies have challenged the upper antigen limit of CTL monoculture, as Gerdemann et al successfully produced CTLs specific for seven viruses (CMV, EBV, Adv, BK, HHV6, respiratory syncytial virus (RSV), and influenza) utilizing peptide pools for 15 antigens, and demonstrated specific activity against all targeted viruses via interferon-gamma ELISPOT.Citation34 As additional preclinical studies attempt to add further pathogens to monoculture, it remains to be seen whether an increased number of targets will compromise specific CTL function or persistence in vivo.
Engineering resistance to immunosuppression
The need for immunosuppressive medications is common in recipients of HSCT, and unfortunately the use of these drugs also suppresses CTL products. Most existing protocols require recipients to be receiving less than 0.5 mg/kg/day prednisone and at least 30 days out from any anti-T-cell serotherapy in order to receive a CTL infusion. Calcineurin inhibitors such as cyclosporin A, tacrolimus, or sirolimus would similarly impact the clinical benefits of CTL at therapeutic doses.
One answer to this problem is to produce genetically modified CTLs that have resistance to immunosuppressive medications. Several recent studies have successfully demonstrated the viability of this concept. De Angelis et al produced EBV-specific CTLs with resistance to tacrolimus by knockdown of FKBP12 via a retrovirally-transduced specific siRNA.Citation70 Transduction of CTLs did not impact antiviral activity, and the cells showed activity in a mouse EBV-lymphoma model in the presence of tacrolimus. Brewin et al similarly produced EBV-specific CTLs with resistance to both cyclosporin A and tacrolimus by direct mutation of calcineurin.Citation71 The mutation had no impact on the phenotype or antiviral activity of the CTL in vitro, and mutated cells showed a growth advantage in the presence of calcineurin inhibitors.
Although similarly modified cells have not been used clinically to date, they have great potential in treating both HSCT and solid organ transplant recipients. Future extension of these studies could potentially allow production of CTLs with resistance to monoclonal biologic agents such as alemtuzumab.
Conclusion
With several hundred patients having been treated successfully, antipathogen CTLs have been established as a safe and highly effective therapy following HSCT. Further studies to identify preserved viral T-cell epitopes, probe the antigen limits in CTL monoculture, and test the clinical efficacy of immunosuppressive-resistant CTLs will further broaden the usefulness of this therapy. As rapid advances in protocols and multiple available methods of manufacture broaden the availability of this therapy, in time CTL therapy may become the standard of care following HSCT.
Acknowledgments
This work was supported by a National Institute of Child Health and Human Development award to MDK (K12-HD-001399) and Cancer Prevention and Research Institute of Texas (R01 RP100469) and National Cancer Institute (P01 CA148600-02) awards to CMB.
Disclosure
The authors report no conflicts of interest.
References
- BoeckhMLeisenringWRiddellSRLate cytomegalovirus disease and mortality in recipients of allogeneic hematopoietic stem cell transplants: importance of viral load and T-cell immunityBlood2003101240741412393659
- BrunsteinCGWeisdorfDJDeForTMarked increased risk of Epstein-Barr virus-related complications with the addition of antithymocyte globulin to a nonmyeloablative conditioning prior to unrelated umbilical cord blood transplantationBlood200610882874288016804113
- MyersGDKranceRAWeissHAdenovirus infection rates in pediatric recipients of alternate donor allogeneic bone marrow transplants receiving either antithymocyte globulin (ATG) or alemtuzumab (Campath)Bone Marrow Transplant200536111001100816184180
- NeofytosDHornDAnaissieEEpidemiology and outcome of invasive fungal infection in adult hematopoietic stem cell transplant recipients: analysis of Multicenter Prospective Antifungal Therapy (PATH) Alliance registryClin Infect Dis200948326527319115967
- AveryRUpdate in management of ganciclovir-resistant cytomegalovirus infectionCurr Opin Infect Dis200821443343718594298
- BironKKAntiviral drugs for cytomegalovirus diseasesAntiviral Res2006712–315416316765457
- NicholsWGCoreyLGooleyTRising pp65 antigenemia during preemptive anticytomegalovirus therapy after allogeneic hematopoietic stem cell transplantation: risk factors, correlation with DNA load, and outcomesBlood200197486787411159510
- LjungmanPDeliliersGLPlatzbeckerUCidofovir for cytomegalovirus infection and disease in allogeneic stem cell transplant recipients. The Infectious Diseases Working Party of the European Group for Blood and Marrow TransplantationBlood200197238839211154213
- KuehnleIHulsMHLiuZCD20 monoclonal antibody (rituximab) for therapy of Epstein-Barr virus lymphoma after hemopoietic stem-cell transplantationBlood20009541502150510666232
- KomanduriKVSt JohnLSde LimaMDelayed immune reconstitution after cord blood transplantation is characterized by impaired thymopoiesis and late memory T-cell skewingBlood2007110134543455117671230
- RubinsteinPCarrierCScaradavouAOutcomes among 562 recipients of placental-blood transplants from unrelated donorsN Engl J Med199833922156515779828244
- PapadopoulosEBLadanyiMEmanuelDInfusions of donor leukocytes to treat Epstein-Barr virus-associated lymphoproliferative disorders after allogeneic bone marrow transplantationN Engl J Med199433017118511918093146
- SlezakSLBettinottiMSelleriSAdamsSMarincolaFMStroncekDFCMV pp65 and IE-1 T cell epitopes recognized by healthy subjectsJ Transl Med200751717391521
- LeenAMChristinAKhalilMIdentification of hexon-specific CD4 and CD8 T-cell epitopes for vaccine and immunotherapyJ Virol200882154655417942545
- BollardCMRooneyCMHeslopHET-cell therapy in the treatment of post-transplant lymphoproliferative diseaseNat Rev Clin Oncol20129951051922801669
- HanleyPJCruzCRSavoldoBFunctionally active virus-specific T cells that target CMV, adenovirus, and EBV can be expanded from naive T-cell populations in cord blood and will target a range of viral epitopesBlood200911491958196719443656
- LeenAMMyersGDSiliUMonoculture-derived T lymphocytes specific for multiple viruses expand and produce clinically relevant effects in immunocompromised individualsNat Med200612101160116616998485
- SiliUHulsMHDavisARLarge-scale expansion of dendritic cell-primed polyclonal human cytotoxic T-lymphocyte lines using lymphoblastoid cell lines for adoptive immunotherapyJ Immunother200326324125612806278
- KernFFaulhaberNFrommelCAnalysis of CD8 T cell reactivity to cytomegalovirus using protein-spanning pools of overlapping pentadecapeptidesEur J Immunol20003061676168210898504
- HanleyPJShafferDRCruzCRExpansion of T cells targeting multiple antigens of cytomegalovirus, Epstein-Barr virus and adenovirus to provide broad antiviral specificity after stem cell transplantationCytotherapy201113897698621539497
- KalosMJuneCHAdoptive T cell transfer for cancer immunotherapy in the era of synthetic biologyImmunity2013391496023890063
- SellarRSPeggsKSThe role of virus-specific adoptive T-cell therapy in hematopoietic transplantationCytotherapy201214439140022420834
- HansenSGPowersCJRichardsREvasion of CD8+ T cells is critical for superinfection by cytomegalovirusScience2010328597410210620360110
- NeudorferJSchmidtBHusterKMReversible HLA multimers (Streptamers) for the isolation of human cytotoxic T lymphocytes functionally active against tumor- and virus-derived antigensJ Immunol Methods20073201–211913117306825
- SchmittATonnTBuschDHAdoptive transfer and selective reconstitution of streptamer-selected cytomegalovirus-specific CD8+ T cells leads to virus clearance in patients after allogeneic peripheral blood stem cell transplantationTransfusion201151359159921133926
- BollardCMKuehnleILeenARooneyCMHeslopHEAdoptive immunotherapy for posttransplantation viral infectionsBiol Blood Marrow Transplant200410314315514993880
- GattinoniLKlebanoffCAPalmerDCAcquisition of full effector function in vitro paradoxically impairs the in vivo antitumor efficacy of adoptively transferred CD8+ T cellsJ Clin Invest200511561616162615931392
- HeslopHESlobodKSPuleMALong-term outcome of EBV-specific T-cell infusions to prevent or treat EBV-related lymphoproliferative disease in transplant recipientsBlood2010115592593519880495
- MelenhorstJJLeenAMBollardCMAllogeneic virus-specific T cells with HLA alloreactivity do not produce GVHD in human subjectsBlood2010116224700470220709906
- PeggsKSVerfuerthSPizzeyAAdoptive cellular therapy for early cytomegalovirus infection after allogeneic stem-cell transplantation with virus-specific T-cell linesLancet200336293931375137714585640
- HeslopHESlobodKSPuleMALong-term outcome of EBV-specific T-cell infusions to prevent or treat EBV-related lymphoproliferative disease in transplant recipientsBlood2010115592593519880495
- WalterEAGreenbergPDGilbertMJReconstitution of cellular immunity against cytomegalovirus in recipients of allogeneic bone marrow by transfer of T-cell clones from the donorN Engl J Med199533316103810447675046
- TrivediDWilliamsRYO’ReillyRJKoehneGGeneration of CMV-specific T lymphocytes using protein-spanning pools of pp65-derived overlapping pentadecapeptides for adoptive immunotherapyBlood200510572793280115514011
- GerdemannUKeirnanJMKatariULRapidly generated multivirus-specific cytotoxic T lymphocytes for the prophylaxis and treatment of viral infectionsMol Ther20122081622163222801446
- HanleyPJCruizRYMelenhorstJNaïve T-cell-derived CTL recognize atypical epitopes of CMVpp65 with higher avidity than CMV-seropositive donor-derived CTL – a basis for treatment of post-transplant viral infection by adoptive transfer of T-cells from virus-naïve donorsCytotherapy2013154S9
- BergerCJensenMCLansdorpPMGoughMElliottCRiddellSRAdoptive transfer of effector CD8+ T cells derived from central memory cells establishes persistent T cell memory in primatesJ Clin Invest2008118129430518060041
- WillingerTFreemanTHasegawaHMcMichaelAJCallanMFMolecular signatures distinguish human central memory from effector memory CD8 T cell subsetsJ Immunol200517595895590316237082
- CobboldMKhanNPourgheysariBAdoptive transfer of cytomegalovirus-specific CTL to stem cell transplant patients after selection by HLA-peptide tetramersJ Exp Med2005202337938616061727
- FeuchtingerTOpherkKBethgeWAAdoptive transfer of pp65-specific T cells for the treatment of chemorefractory cytomegalovirus disease or reactivation after haploidentical and matched unrelated stem cell transplantationBlood2010116204360436720625005
- PeggsKSThomsonKSamuelEDirectly selected cytomegalovirus-reactive donor T cells confer rapid and safe systemic reconstitution of virus-specific immunity following stem cell transplantationClin Infect Dis2011521495721148519
- FeuchtingerTMatthes-MartinSRichardCSafe adoptive transfer of virus-specific T-cell immunity for the treatment of systemic adenovirus infection after allogeneic stem cell transplantationBr J Haematol20061341647616803570
- UhlinMOkasMGertowJUzunelMBrismarTBMattssonJA novel haplo-identical adoptive CTL therapy as a treatment for EBV-associated lymphoma after stem cell transplantationCancer Immunol Immunother201059347347719908041
- MoosmannABigalkeITischerJEffective and long-term control of EBV PTLD after transfer of peptide-selected T cellsBlood2010115142960297020103780
- LeenAMChristinAMyersGDCytotoxic T lymphocyte therapy with donor T cells prevents and treats adenovirus and Epstein-Barr virus infections after haploidentical and matched unrelated stem cell transplantationBlood2009114194283429219700662
- MicklethwaiteKPClancyLSandherUProphylactic infusion of cytomegalovirus-specific cytotoxic T lymphocytes stimulated with Ad5f35pp65 gene-modified dendritic cells after allogeneic hemopoietic stem cell transplantationBlood2008112103974398118768783
- BlythEClancyLSimmsRDonor-derived CMV- specific T cells reduce the requirement for CMV-directed pharmacotherapy after allogeneic stem cell transplantationBlood2013121183745375823435462
- VeraJFBrennerLJGerdemannUAccelerated production of antigen-specific T cells for preclinical and clinical applications using gas-permeable rapid expansion cultureware (G-Rex)J Immunother201033330531520445351
- GerdemannUChristinASVeraJFNucleofection of DCs to generate multivirus-specific T cells for prevention or treatment of viral infections in the immunocompromised hostMol Ther20091791616162519584818
- CruzCRHanleyPJLiuHAdverse events following infusion of T cells for adoptive immunotherapy: a 10-year experienceCytotherapy201012674374920429793
- BarkerJNDoubrovinaESauterCSuccessful treatment of EBV-associated posttransplantation lymphoma after cord blood transplantation using third-party EBV-specific cytotoxic T lymphocytesBlood2010116235045504920826724
- LeenAMBollardCMMendizabalAMMulticenter study of banked third-party virus-specific T cells to treat severe viral infections after hematopoietic stem cell transplantationBlood2013121265113512323610374
- UhlinMGertowJUzunelMRapid salvage treatment with virus-specific T cells for therapy-resistant diseaseClin Infect Dis20125581064107322806594
- Wy IpWQasimWManagement of adenovirus in children after allogeneic hematopoietic stem cell transplantationAdv Hematol2013201317641824288536
- QasimWDerniameSGilmourKThird-party virus-specific T cells eradicate adenoviraemia but trigger bystander graft-versus-host diseaseBr J Haematol2011154115015321501134
- BalduzziALucchiniGHirschHHPolyomavirus JC-targeted T-cell therapy for progressive multiple leukoencephalopathy in a hematopoietic cell transplantation recipientBone Marrow Transplant201146798799220921942
- RamosCANaralaNVyasGMHuman papillomavirus type 16 E6/E7-specific cytotoxic T lymphocytes for adoptive immunotherapy of HPV-associated malignanciesJ Immunother2013361667623211628
- SchubASchusterIGHammerschmidtWMoosmannACMV-specific TCR-transgenic T cells for immunotherapyJ Immunol2009183106819683019864595
- XueSAGaoLAhmadiMHuman MHC Class I-restricted high avidity CD4 T cells generated by co-transfer of TCR and CD8 mediate efficient tumor rejection in vivoOncoimmunology201321e2259023483821
- FrumentoGZhengYAubertGCord blood T cells retain early differentiation phenotype suitable for immunotherapy after TCR gene transfer to confer EBV specificityAm J Transplant2013131455523016879
- MRCCMV TCR Gene Therapy: A Phase I/II Safety, Toxicity and Feasibility Study of Adoptive Immunotherapy in Allo-HSCT Available from: http://gtr.rcuk.ac.uk/project/644662DD-8EE2-4A77-82F2-24DB-D79B1B87. Project reference: G0701703Accessed June 11, 2014
- MilnerJDHollandSMThe cup runneth over: lessons from the ever-expanding pool of primary immunodeficiency diseasesNat Rev Immunol201313963564823887241
- KimCJMcKinnonLRKovacsCMucosal Th17 cell function is altered during HIV infection and is an independent predictor of systemic immune activationJ Immunol201319152164217323894197
- CruzCRLamSHanleyPJRobust T cell responses to aspergillosis in chronic granulomatous disease: implications for immunotherapyClin Exp Immunol20131741899623763437
- BeckOToppMSKoehlUGeneration of highly purified and functionally active human TH1 cells against Aspergillus fumigatusBlood200610762562256916322466
- TramsenLSchmidtSBoenigHClinical-scale generation of multi-specific anti-fungal T cells targeting Candida, Aspergillus and mucormycetesCytotherapy201315334435123579059
- KhannaNStuehlerCConradBGeneration of a multipathogen-specific T-cell product for adoptive immunotherapy based on activation-dependent expression of CD154Blood201111841121113121642594
- GomezMJMarasBBarcaALa ValleRBarraDCassoneABiochemical and immunological characterization of MP65, a major mannoprotein antigen of the opportunistic human pathogen Candida albicansInfect Immun200068269470110639435
- JolinkHMeijssenICHagedoornRSCharacterization of the T-cell-mediated immune response against the Aspergillus fumigatus proteins Crf1 and catalase 1 in healthy individualsJ Infect Dis2013208584785623698813
- PerruccioKTostiABurchielliETransferring functional immune responses to pathogens after haploidentical hematopoietic transplantationBlood2005106134397440616123217
- De AngelisBDottiGQuintarelliCGeneration of Epstein-Barr virus-specific cytotoxic T lymphocytes resistant to the immunosuppressive drug tacrolimus (FK506)Blood2009114234784479119759356
- BrewinJMancaoCStraathofKGeneration of EBV-specific cytotoxic T cells that are resistant to calcineurin inhibitors for the treatment of posttransplantation lymphoproliferative diseaseBlood2009114234792480319770360
- GerdemannUKatariULPapadopoulouASafety and clinical efficacy of rapidly-generated trivirus-directed T cells as treatment for adenovirus, EBV, and CMV infections after allogeneic hematopoietic stem cell transplantMol Ther201321112113212123783429
