ABSTRACT
Medical education has an important role in developing attitudes, behaviors and cultures that support safe care. Increasingly, however, research has argued for a more interprofessional approach to be taken. This scoping review examines the design and impact of interprofessional education interventions involving medical students that focus on patient safety. We systematically searched PubMed, EMBASE, PsycINFO and CINAHL between January 2000 and November 2019. Studies were eligible if they included medical students and at least one other profession, interactive learning, a strong emphasis on patient safety in the learning objectives, and an empirical method of evaluation. Forty-three studies met these criteria and the diverse range of approaches to intervention design and method of evaluation are detailed in this review. We found that interprofessional patient safety education interventions are generally well received by students with knowledge and skill gain documented; several also reported changes in student behaviour. However, the lack of empirically driven study designs, combined with the lack of rigour when reporting, makes it difficult to draw clear comparisons. Future research should address this, and in particular, report how and why the intervention has been designed to be delivered interprofessionally.
Introduction
Patient safety is recognized internationally as a cornerstone of healthcare policy and practice. However, with an estimated 42.7million adverse events each year worldwide (Jha et al., Citation2013), and despite over two decades of improvement focussed on quality and patient safety, it is also regarded as a “tough nut to crack” (Leistikow et al., Citation2011, p. 342).
Patient safety is broadly defined by the World Health Organization (WHO) as the ‘coordinated efforts to prevent harm, caused by the process of healthcare itself, from occurring to patients’ (World Health Organisation, Citation2019) and since the seminal report To Err is Human (Donaldson et al., Citation2000), research unpicking these causes has increasingly gained traction (Okuyama et al., Citation2014). This has led to professional bodies around the world endorsing a patient safety competencies framework for healthcare professionals to firmly cement its place within training (Institute of Medicine (US), Citation2018; Canadian Patient Safety Institute (Canada), Citation2018; General Medical Council (UK), Citation2018).
As the discipline has evolved, medical educators have also worked to explore in what ways it should be adopted into undergraduate curricula (Mayer et al., Citation2009), and have developed initiatives that not only improve knowledge, skills and attitudes, but importantly put it at the forefront of medical graduates’ minds. A systematic review examining curricula targeted at medical students and trainees found that initiatives are generally well accepted and do usually achieve positive outcomes (Wong et al., Citation2010). Yet, integrating effective patient safety teaching that acknowledges the complexity of the modern healthcare environment remains challenging (Nie et al., Citation2011).
The prevailing silo-model of teaching patient safety may be one reason why (Mayer et al., Citation2009). Whilst interprofessional education (IPE) is a compulsory feature of most clinical education curricula (General Medical Council, Citation2018), the majority of undergraduate and postgraduate programmes continue to deliver patient safety teaching uniprofessionally, with limited recognition that this does not reflect how it is addressed in practice. This approach is in contrast with extensive research demonstrating that cohesive teams where health professionals work well together, are associated with better patient outcomes (Grumbach, Citation2004) and that teamwork skills and collaboration are linked with safe and effective health care (Wood, Citation2001). Emergent evidence also suggests that healthcare students viewing patient safety as a team activity, can help address unhelpful cultures and practices associated with imbalances in power and hierarchy that can lead to unsafe care (Paradis & Whitehead, Citation2018). Indeed, a recent narrative review exploring the evidence for interprofessional training and education across both staff and students (S Reeves et al., Citation2017), provides further support for such a hypothesis, in their finding that such approaches can be key to promoting safe patient care. Despite this recent narrative review (S Reeves et al., Citation2017), educators developing medical curricula to support patient safety knowledge and practice, still have little guidance derived from an assessment of the evidence, from which to draw on in making decisions about where, when, and how patient safety should be taught interprofessionally.
This review aimed to address this gap and specifically examine the design and impact of interprofessional patient safety education (IPSE) interventions involving medical students. As researchers based in a UK Medical School with responsibility for ensuring IPE and patient safety are integrated into curricula, we were also interested in understanding some of the practical issues around implementation. Due to the body of knowledge around this topic being heterogeneous, and as the main aim was to summarize, describe and examine evidence, a scoping review was undertaken and is reported in accordance with the PRISMA-ScR guidelines (Tricco et al., Citation2018). Specifically, our objectives were:
identify and describe the educational content, teaching methods and interprofessional approach of IPSE interventions;
describe and assess how IPSE interventions were designed and evaluated;
identify factors which may influence the implementation of IPSE interventions.
Methods
Eligibility criteria
Eligibility criteria were agreed by the authorship team, and comprised:
papers reporting educational interventions with an explicit focus on patient safety, with patient safety listed as a learning objective, and where it was detailed within the intervention content;
papers reporting interventions that involved a minimum of two health and social care undergraduate or postgraduate programmes, one of whom was our home discipline of medical education;
papers reporting interventions that involved interactive learning with some element of face-to-face contact to facilitate this;
papers reporting interventions that included a method of evaluation and/or primary empirical research methods (conference proceedings and case studies were excluded).
Information sources and search terms
The search was performed using the following electronic databases: Pubmed, EMBASE, PsycINFO, Cumulative Index to Nursing and Allied Health Literature (CINAHL) between January 2000 (the year the Department of Health outlined a patient safety strategy in the UK; Department of Health, Citation2001) and February 2017. A further search was also made between January 2017 and November 2019 prior to publication to update the content using the same search terms and across all databases. Search terms were agreed by all authors with reference to our research questions, known literature, and profession-specific terminology (see Supplementary File 2). Reference lists of relevant articles were reviewed to capture missing literature.
Data charting process and synthesis of results
As outlined in the Best Evidence Medical Education (BEME) review literature (Harden et al., Citation1999), we extracted the key descriptors of the interventions (e.g. participants, setting, and course structure) and noted the methodological features of the evaluation. Level of evaluation was classified by SH using Kirkpatrick’s model (Kirkpatrick, Citation1967). This model is widely used because it clearly outlines the levels at which you can evaluate education interventions. A description of each of the levels in the context of medical education can be seen in . The key findings were also extracted to meet our aims and data were synthesized iteratively by all members of the research team, to construct themes (Guest et al., Citation2012) relating to the factors associated with successful implementation.
Table 1. The Kirkpatrick model (Kirkpatrick, Citation1967) in the context of medical education
Critical appraisal of individual sources of evidence
The Quality Assessment Tool for Studies with Diverse Designs (QATSDD) was used to assess study quality as it allows an overall assessment to be made on the rigour of research design and execution, both for qualitative and quantitative work (Sirriyeh et al., Citation2012). SH conducted quality assessments for all studies (SH) and JOH conducted a second quality assessment on a random sample of 5 articles (12%). There was 79% agreement between reviewers. Following a discussion on why there was disagreement on certain criteria, a consensus was reached and adjustments were then made to all scores by SH.
Results
Selection of sources of evidence
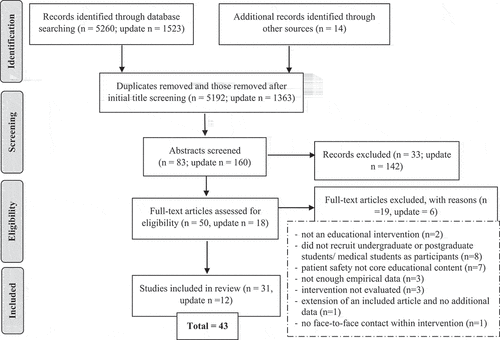
SH undertook the initial search, removed duplicates and screened article titles. The remaining abstracts were screened independently by two reviewers (SH and SF) to determine if they met the inclusion criteria. Any discrepancies were discussed and once a consensus was reached, ineligible papers were removed. Two authors (SH and SF) then assessed the articles in full, with a third author (JOH) screening those where there was a discrepancy. This process identified 43 papers. The full study selection process is illustrated in and all included papers are listed in (study design and methodology) and Supplementary File 1 (intervention design and study findings).
Table 2. Study design and methodology
Critical appraisal within sources of evidence
The quality of the journal articles varied dramatically. QATSDD scores ranged from 9.5% to 74% with an average of 38%. Nineteen articles did not make any reference to a research aim (44%) and no articles justified their sample size in terms of analysis. Few mentioned any kind of user involvement in the design of the study and few made reference to any kind of theoretical framework.
Characteristics of sources of evidence
Of the 43 articles, the majority were from the USA (23), with eight from the UK and five from Canada. Of the remaining seven, two were from Norway, one from Indonesia, one from Sweden, one from Switzerland, one from Germany and one from New Zealand. Twenty seven (63%) of the included articles were published in the last 6 years (2014–2019), three were published in 2013, four in 2012, four in 2010, two in 2009, two in 2006, and one in 2005.
Study design and methodology
Twenty-three of the studies used a post-intervention design and nineteen a pre-post design. Seven of the forty-three involved some method of follow-up and two involved a control group. The full breakdown of study design and methodology can be seen in .
Eighteen of the studies used validated quantitative measures or performance data, for example: the Scope of Practice Checklist (Amerongen et al., Citation2015); the Interprofessional Collaborative Competency Attainment Survey (Baker & Durham, Citation2013); the Teamwork Attitudes Questionnaire and the Attitudes, Motivation, Utility and Self-efficacy Questionnaire (Headrick et al., Citation2012). Qualitative methods included open-ended questions, simulation debrief sessions, focus groups, interviews, observations and written reflections.
Level of evaluation
Descriptions of the levels can be seen in and the level of evaluation judged to have been reached by each study can be seen in Supplementary File 1. The vast majority of the studies (34; 79%) were classified as reaching levels 1, 2a or 2b with their outcomes through: 1) capturing satisfaction with the intervention; 2a) assessing student perceptions of patient safety and interprofessional working and whether their attitude toward it had changed; and, 2b) measuring knowledge or skill gain through self-reporting measures.
However, seven studies (16%) reached level 3 by assessing behavioural change through the use of follow-up questionnaires where participants were asked whether they had retained the knowledge and skills gained from the intervention and/or if it had influenced how they practice in a clinical environment (Clay et al., Citation2017; Ernawati et al., Citation2015; Fowler et al., Citation2018; Headrick et al., Citation2012; Motycka et al., Citation2018; SA Reeves et al., Citation2017; Spence et al., Citation2012). One study (Stevenson et al., Citation2015) assessed organizational change (level 4a) through collecting reports from hospital sites on the impact of staff/student collaborative quality improvement projects. One study (Anderson et al., Citation2009) assessed to what extent patients had benefitted from the intervention (level 4b) by comparing monthly data reports on patient safety events. However, there were no concrete findings at levels 4a or 4b. Supplementary File 1 lists the Kirkpatrick levels alongside the intervention designs and study findings of each paper, should more detail be required.
Student characteristics
All forty-three of the interventions included medical students as participants, but the involvement of students from other professions varied. Thirteen involved medicine and one other profession (30%), eleven involved medicine and two other professions (26%), seven involved medicine and three other professions (16%), nine involved medicine and four or more other professions (21%) and three did not detail the professions in enough detail to extract this information (7%) (Anderson et al., Citation2009; Vyas et al., Citation2012; Wipfler et al., Citation2019).
More specifically, 35 involved nursing, 22 involved pharmacy, nine involved physiotherapy/physical therapy, eight involved physician assistant/associates, six involved occupational therapy and four involved dentistry. Thirteen studies involved students from a range of other professions: social work and public health; industrial engineering, biomedical engineering, public health and mass communication; health admin; nutrition; social work, speech and language pathology; operating room technicians; health sciences ; audiology, radiography, physiology, midwifery, social work and assistant practitioners; paramedics; respiratory therapy and health administration; therapy courses; emergency medical services; and, respiratory therapy and speech and language therapy. Two involved staff members as well as students.
Educational characteristics
Educational setting
The classroom was the dominant setting for interventions with 18 studies based within this setting only. Six studies had a classroom setting with online components; five used a classroom and ward setting and one used a classroom and simulated acute care setting. Eight used only a simulated acute care setting and two used a simulated acute care setting and online components. One used only a ward setting and two did not state the setting.
Teaching methods
Most of the studies (25) had interventions that used small-group work; 18 involved simulations and debriefings; 16 delivered didactic teaching methods such as lectures, seminars and tutorials; 14 studies used video, audio or written resources; 12 involved case-based discussions; 10 featured an online reading or coursework activity; nine had presentations or question and answer sessions as an element; eight included large group work activities; seven adopted experiential learning in a clinical environment (e.g., speaking to patients or staff); four involved role play and three did not fully describe the methods used to extract this information.
Educational content
The interventions covered a range of patient safety content (see Supplementary File 1) and a certain amount of overlap has to be acknowledged, but to summarize the main topics: twenty focused on teamwork and communication; 12 focused on medication safety; 10 on error disclosure or incident reporting; 10 focused on error prevention; seven focused on root cause analysis; four on quality improvement; three on systems based thinking; two on scope of practice; two on human factors.
Factors identified as influential in the implementation of IPSE interventions
Many of the papers discussed factors that inhibited or facilitated implementation of their intervention, with some listing recommendations for those developing similar interventions in the future. Commonly cited factors have been collated by the authors into the following three topics, with illustrative quotes from the papers given.
Logistics
Much of the current IPE literature addresses the fact that logistical challenges are common (e.g. Lawlis et al., Citation2014) and unsurprisingly they were referenced in the majority of included papers. Scheduling, cross programme infrastructure, the level of faculty and programme lead support, the physical space necessary to host the intervention, the training and choice of facilitators, and having a local champion to act as advocate, all emerged as important considerations. Effective logistics management therefore seems to be the bedrock from which any interprofessional intervention should be built.
“Infrastructure must be in place for centralised coordination of IPE between faculties” (Delisle et al., Citation2016, p. 784)
“[consider] curricular culture, philosophy of curriculum of study for each discipline-specific program, faculty awareness and attitudes toward this material, practical aspects of available curricular time across programs, varying requirements for curricular committee approvals by programs” (Galt et al., Citation2006, p. 216)
Educational content
The patient safety-related educational content of the intervention is also important to consider. The included papers argued it should be engaging, realistic and readily applicable to practice with students understanding the relevance and value of the content for their own profession. Referencing international/national guidelines and involving a range of experts and students from all health professions when developing the content was also discussed as beneficial.
“Scenarios that are set for groups need to be developed by interprofessional groups, and specifically provide tasks that engage and challenge all of the professions involved” (Hardisty et al., Citation2014, p. 295)
“Students and their views should be involved when designing similar educational modules” (Gjessing et al., Citation2014, p. 346)
Intervention design
The design of IPSE interventions was commonly cited as important. Where interventions were judged as ‘successful’ by the authors, the number of students, the number of professions involved and ensuring that students were at the appropriate level of training for the content, were discussed as key facilitating factors. The setting and teaching method were also highlighted as significant but there was an extensive amount of variation. For example, many chose to have online components to overcome difficulties around getting students together but this arguably restricts opportunities to learn from each other. The papers show that there is no one set of optimum conditions; they are very much dependent on the learning objectives and aim of the intervention.
“Small group factors of size, mix, balance, and stability are critical to the success of IPL” (Achike et al., Citation2014, p. 837)
“Giving the students the opportunity to practice these new skills in a real-life situation motivated them because they could experience and appreciate the practicality of their work” (Wilson et al., Citation2012, p. 24)
“[provide] encounters with real patients to give meaning, validity, and a ‘face’ to the experience for the students” (Headrick et al., Citation2012, p. 2674)
Discussion
This paper aimed to review the extant empirical literature on IPSE interventions involving medical students and we identified 43 as fulfilling these criteria. We found that to date, most of the literature has taken the form of evaluations of IPSE interventions on particular patient safety topics, in particular contexts, with most well accepted and leading to knowledge or skill acquisition. As 63% were published in the last 6 years it is encouraging that the field also appears to be expanding. However, what is most notable is the degree of diversity reported. IPSE is undertaken with students of different years from an array of professions, with different patient safety foci, in a variety of settings, using a range of teaching methods and various tools to evaluate learning. In many ways this diversity reflects the complexity of the discipline.
Our ability to draw comparisons between interventions, however, is inhibited by the quality of the studies, as most sought only to ‘evaluate’ rather than conduct ‘research’. Consequently, few addressed specific research questions, nor developed a research design before the intervention commenced. 53% of the studies collected data only post-intervention, in relation to students’ movement toward intended learning outcomes, and mostly through self-report measures. The impact of IPSE on clinical processes and patients was only reported in two instances. In some ways this is unsurprising, given that the shift toward empirically driven IPE is slow and that the impact of patient safety teaching on clinical processes and patients is notoriously difficult to measure (Wong et al., Citation2010). However, what this means is that whilst the results indicate that IPSE interventions are likely to be both feasible and (to some extent) impactful, their transferability to other contexts and their sustainability is difficult to establish.
As is common within the field of medical education, there was instead a heavy reliance on the outcome evaluation model where studies only ask ‘did it work?’, which does not take into account the contextual factors acting over the time of the intervention and how they influenced the outcomes (Sandars et al., Citation2017). A substantial number of studies also did not report all aspects of their intervention design. Such information is crucial with IPSE because the empirical lens is emergent and learning is very context dependent. Both the evaluation and reporting of IPSE interventions, therefore, needs to be better addressed, in order for findings to be shared with the wider medical education community in a useful way. Frameworks such as SQUIRE (Standards for Quality Improvement Reporting Excellence; Ogrinc et al., Citation2015) or comprehensive checklists in the IPE literature (Meinema et al., Citation2018) may be a way of doing this.
Setting aside these methodological concerns, this scoping review presents a diverse range of approaches to IPSE and can highlight some pressing questions for the discipline. One area for debate is the optimal setting for interprofessional patient safety teaching. Despite the current emphasis on workplace learning within healthcare education (Billett, Citation2016) and IPE (Kent et al., Citation2018), only six studies based their interventions in clinical settings and involved ‘real’ patients and/or staff. Significant improvements in student knowledge and skills were reported within these studies but also high levels of motivation and enthusiasm, with most studies arguing that this was because their intervention reflected, or allowed access to, ‘real life’ patient safety situations. Indeed, research has shown that students lack motivation to learn topics that are not self-evidently at the core of medicine (Aarnio et al., Citation2010) and clinically-based IPSE may help emphasize to students the importance and complexity of delivering safe patient care. Further, Paradis and Whitehead (Paradis and Whitehead, Citation2018) recently called for more practice-based IPE interventions at undergraduate level so that students learn how to navigate and transform power, structures and systems which limit and constrain collaboration within healthcare settings. Most studies, however, relied on classroom-based teaching. Possible reasons for this include the logistical challenges of getting students from different professions together off-campus, a perceived need for all students to have access to the same IPE opportunities and the difficulties around designing and assessing interventions in a potentially unpredictable environment. Currently, there is no rigorous evidence as to which IPE settings are most appropriate for which purposes and why. These studies indicate that there is a balance to strike and further research exploring curriculum designers’ choices and their consequences is necessary to decide where this resides.
Another important question that has emerged concerns the lens through which patient safety is taught. The primary lens in the included studies was teamwork and communication, but there were a variety of others including medication safety, error prevention and human factors which evaluated well. This reflects the growth in literature exploring where the intersections between patient safety and interprofessional working lie (Rowland & Kitto, Citation2014), with efforts nationally and internationally toward standardized patient safety competencies where ‘interprofessional working’ is one of the domains (e.g. Canadian Patient Safety Institute, Citation2018). Effective teamworking is better understood in interprofessional teams with the use of working life concrete examples. Moving forward, therefore, educators might want to question how such examples can be better integrated into patient safety teaching.
Furthermore, given the emergent nature of the IPSE evidence base, it may be premature to extrapolate too much from our findings without first challenging the fundamental assumption that IPE is implicitly a good idea when teaching patient safety. There is arguably no one conceptualization of patient safety (Infante, Citation2006), and the notion that it will act as a unifying mechanism across all professions is being challenged (Rowland & Kitto, Citation2014). Whilst all but two papers explained which professions were involved, very few explained why they were chosen, the interprofessional setup of the groups and how the intervention was developed with specifically those professions in mind, nor how this influenced facilitator training, the language being used or the scenario design. Moving forward more research is required exploring how patient safety, and any lens through which it is taught, is conceptualized differently by healthcare professions and, therefore, how that should shape the uniprofessional or interprofessional approach being used.
Finally, an obvious, and important omission in the current literature, must be the role of the patient perspective in the healthcare ‘team’. There is increasing evidence that patients and families perform a variety of key behaviours that support patient safety (Lawton & Armitage, Citation2012; Ward & Armitage, Citation2012). Thus, it would seem important to include this key perspective and potential source of safety within our conceptualizations of healthcare teams, and by implication, our approach to teaching patient safety across professions.
Limitations
There are limitations to this review. Firstly, this scoping review only included papers where medical students had been participants. Whilst this was always our aim and reflects our professional interests as medical educators, this may have meant important and influential papers exploring IPSE interventions without medical students were omitted. In addition, including only papers written in English may have excluded noteworthy publications. Whilst there was consensus amongst the authors regarding search terms, we are all based within medical education and profession-specific terminology may have been missed and caused pre-exclusion of relevant studies.
Conclusions
IPSE interventions are well received by students, often lead to the acquisition of patient safety knowledge and skills, and can also lead to changes in behaviour around safe care practices. However, at this time there is no evidence that they lead to improvements in clinical processes or patient care. The existing literature is incredibly diverse which reflects the complexity and recent growth of the discipline. The interventions cover different patient safety topics, involve different professions at different stages of training, utilize different settings and teaching methods and have different ways of assessing students. This breadth of work is encouraging for the future development and entrenching of IPSE, but it also makes it difficult to draw firm conclusions and make clear recommendations for research and practice. Indeed, it would at this time be a disservice to the field to attempt to generalize findings into one ‘gold standard approach’.
It may be that to move this field forward, researchers and medical educators need to ‘go back to basics’ and decide why, and under what circumstances, IPE may be the best format for delivering patient safety education. Rather than more studies presenting evaluations of existing IPSE interventions, the evidence base would arguably benefit from more theorizing about the pedagogical foundations of how interprofessional patient safety teaching might work, and ultimately, promote safer clinical practice. Given the ever-increasing number of professions making up healthcare teams, this critique of the underpinnings of interprofessional patient safety teaching will only become more urgent.
Supplemental Material
Download Zip (39.5 KB)Acknowledgments
The authors are sincerely grateful to Dr Alison Ledger for her assistance in synthesising the results. JKO is supported by the National Institute for Health Research Yorkshire and Humber Patient Safety Translational Research Centre (NIHR Yorkshire and Humber PSTRC). The views expressed in this publication are those of the authors and not necesserily those of the NIHR or the Department of Health and Social Care, UK. The authors also wish to thank the Researching Professional Learning Group for their support.
Supplementary material
Supplemental data for this article can be accessed on the publisher’s website
Additional information
Notes on contributors
Sarah D. Howarth
Sarah Howarth is a PhD student and Placement Innovation Officer at the Leeds Institute of Medical Education, School of Medicine, University of Leeds, UK.
Shelley A. Fielden
Shelley Fielden is a Lecturer on the Gateway to Medicine and Applied Health in Medical Education programmes at the Leeds Institute of Medical Education, School of Medicine, University of Leeds, UK.
Jane K. O’Hara
Jane O’Hara is a Professor of Healthcare Quality and Safety at the School of Healthcare, University of Leeds, UK. She is also Deputy Director of the Yorkshire Quality and Safety Research Group and a Theme Lead at the NIHR Yorkshire and Humber Patient Safety Translational Research Centre, both of which are based at the Bradford Institute of Health Research, Bradford Teaching Hospitals NHS Foundation Trust, UK.
References
- Aarnio, M., Nieminen, J., Pyörälä, E., & Lindblom-Ylänne, S. (2010). Motivating medical students to learn teamwork skills. Medical Teacher, 32(4), e199–204. https://doi.org/https://doi.org/10.3109/01421591003657469
- Achike, F. I., Smith, J., Leonard, S., Williams, J., Browning, F., & Glisson, J. (2014). Advancing safe drug use through interprofessional learning (IPL): A pilot study. The Journal of Clinical Pharmacology, 54(7), 832–839. https://doi.org/https://doi.org/10.1002/jcph.289
- Addy, C. L., Browne, T., Blake, E. W., & Bailey, J. (2015). Enhancing interprofessional education: Integrating public health and social work perspectives. American Journal of Public Health, 105(S1), S106–S108. https://doi.org/https://doi.org/10.2105/AJPH.2014.302502
- Amerongen, H. M., LeGros, T. A., Cooley, J. H., Schloss, E. P., & Theodorou, A. (2015). Constructive contact: Design of a successful introductory interprofessional education experience. Currents in Pharmacy Teaching and Learning, 7(5), 565–574. https://doi.org/https://doi.org/10.1016/j.cptl.2015.06.013
- Anderson, E., & Lakhani, N. (2016). Interprofessional learning on polypharmacy. The Clinical Teacher, 13(4), 291–297. https://doi.org/https://doi.org/10.1111/tct.12485
- Anderson, E., Thorpe, L., Heney, D., & Petersen, S. (2009). Medical students benefit from learning about patient safety in an interprofessional team. Medical Education, 43(6), 542–552. https://doi.org/https://doi.org/10.1111/j.1365-2923.2009.03328.x
- Aubin, D., & King, S. (2015). Developing a culture of safety: Exploring students’ perceptions of errors in an interprofessional setting. Journal of Interprofessional Care, 29(6), 646–648. https://doi.org/https://doi.org/10.3109/13561820.2015.1045060
- Baker, M. J., & Durham, C. F. (2013). Interprofessional education: A survey of students’ collaborative competency outcomes. Journal of Nursing Education, 52(12), 713–718. https://doi.org/https://doi.org/10.3928/01484834-20131118-04
- Billett, S. (2016). Learning through health care work: Premises, contributions and practices. Medical Education, 50(1), 124–131. https://doi.org/https://doi.org/10.1111/medu.12848
- Blue, A. V., Charles, L., Howell, D., et al. (2010). Introducing students to patient safety through an online interprofessional course. Advances in Medical Education and Practice, 1, 107–114. https://doi.org/https://doi.org/10.2147/AMEP.S13350
- Breckwoldt, J., Knecht, M., Massée, R., Flach, B., Hofmann-Huber, C., Kaap-Fröhlich, S., Witt, C. M., Aeberhard, R., & Sax, H. (2019, December). Operating room technician trainees teach medical students-an inter-professional peer teaching approach for infection prevention strategies in the operation room. Antimicrobial Resistance and Infection Control, 8(1), 75.
- Bridgeman, M. B., Rusay, M., Afran, J., Yeh, D. S., & Sturgill, M. G. (2018). Impact of an interprofessional medication error workshop on healthcare student perceptions. Currents in Pharmacy Teaching and Learning, 10(7), 975–981. https://doi.org/https://doi.org/10.1016/j.cptl.2018.04.013
- Brock, D., Abu-Rish, E., Chiu, C. R., et al. (2013). Interprofessional education in team communication: Working together to improve patient safety. BMJ Quality & Safety, 22(5), 414–423. https://doi.org/https://doi.org/10.1136/bmjqs-2012-000952
- Canadian Patient Safety Institute (Canada). The safety competencies: Enhancing patient safety across the health professions. (http://www.patientsafetyinstitute.ca/en/toolsResources/safetyCompetencies/Pages/default.aspx). Accessed December 14, 2018.
- Clay, A. S., Chudgar, S. M., Turner, K. M., Vaughn, J., Knudsen, N. W., Farnan, J. M., Arora, V. M., & Molloy, M. A. (2017). How prepared are medical and nursing students to identify common hazards in the intensive care unit? Annals of the American Thoracic Society, 14(4), 543–549. https://doi.org/https://doi.org/10.1513/AnnalsATS.201610-773OC
- Cox, K. R., Scott, S. D., Hall, L. W., Aud, M. A., Headrick, L. A., & Madsen, R. (2009). Uncovering differences among health professions trainees exposed to an interprofessional patient safety curriculum. Quality Management in Health Care, 18(3), 182–193. https://doi.org/https://doi.org/10.1097/QMH.0b013e3181aea237
- Delisle, M., Grymonpre, R., Whitley, R., & Crucial Conversations:, W. D. (2016). An interprofessional learning opportunity for senior healthcare students. Journal of Interprofessional Care, 30(6), 777–786. https://doi.org/https://doi.org/10.1080/13561820.2016.1215971
- Department of Health. (2001). Building a safer NHS for patients.
- Donaldson, M. S., Corrigan, J. M., & Kohn, L. T. (Eds.). (2000). To err is human: Building a safer health system. National Academies Press.
- Ernawati, D. K., Lee, Y. P., & Hughes, J. (2015). Indonesian students’ participation in an interprofessional learning workshop. Ibid, 29(4), 398–400.
- Fowler, T. O., Wise, H. H., Mauldin, M. P., Ragucci, K. R., Scheurer, D. B., Su, Z., Mauldin, P. D., Bailey, J. R., & Borckardt, J. J. (2018). Alignment of an interprofessional student learning experience with a hospital quality improvement initiative. Journal of Interprofessional Care, 11, 1–10. https://doi.org/https://doi.org/10.1080/13561820.2018.1455649
- Galt, K. A., Paschal, K. A., O’brien, R. L., McQuillan, R. J., Graves, J. K., Harris, B., Mahern, C., Scheirton, L. S., Bramble, J. D., Clark, B. E., Gleason, J. M., Hoidal, P., Moores, K., Mu, K., Rule, A. M., Bradberry, J. C., Sonnino, R., & Gerardi, D. (2006). Description and evaluation of an interprofessional patient safety course for health professions and related sciences students. Journal of Patient Safety, 2(4), 207–216. https://doi.org/https://doi.org/10.1097/01.jps.0000236913.71826.16
- General Medical Council. (2018). Outcomes for graduates.
- General Medical Council (UK). Good Medical Practice: Safety and Quality. (https://www.gmc-uk.org/ethical-guidance/ethical-guidance-for-doctors/good-medical-practice/domain-2—-safety-and-quality). Accessed December 14, 2018.
- Gjessing, K., Torge, C. J., Hammar, M., Dahlberg, J., & Faresjo, T. (2014). Improvement of quality and safety in health care as a new interprofessional learning module – Evaluation from students. Journal of Multidisciplinary Healthcare, 7, 341–347. https://doi.org/https://doi.org/10.2147/JMDH.S62619
- Gough, S., Jones, N., & Hellaby, M. (2013). Innovations in interprofessional learning and teaching: Providing opportunities to embed patient safety within the pre-registration physiotherapy curriculum. A Pilot Study. Physical Therapy Reviews, 18(6), 416–430. https://doi.org/https://doi.org/10.1179/1743288X13Y.0000000103
- Grumbach, K. (2004). Can Health care teams improve primary care practice? Journal of the American Medical Association, 291(10), 1246–1251. https://doi.org/https://doi.org/10.1001/jama.291.10.1246
- Guest, G., Macqueen, K. M., & Namey, E. E. (2012). Applied Thematic Analysis. SAGE.
- Guilding, C., Hardisty, J., Randles, E., Statham, L., Green, A., Bhudia, R., Thandi, C. S., & Matthan, J. (2014, September). Making it work: The feasibility and logistics of delivering large-scale interprofessional education to undergraduate healthcare students in a conference format. Journal of Interprofessional Care, 54(7), 832–839. https://doi.org/https://doi.org/10.1080/13561820.2018.1496074
- Harden, M., Grant, J., Buckley, G., & IR Hart, R. (1999). BEME guide no. 1: Best evidence medical education. Medical Teacher, 21(6), 553–562. https://doi.org/https://doi.org/10.1080/01421599978960
- Hardisty, J., Scott, L., Chandler, S., Pearson, P., & Powell, S. (2014). Interprofessional learning for medication safety. The Clinical Teacher, 11(4), 290–296. https://doi.org/https://doi.org/10.1111/tct.12148
- Headrick, L. A., Barton, A. J., Ogrinc, G., et al. (2012). Results of an effort to integrate quality and safety into medical and nursing school curricula and foster joint learning. Health Affairs, 31(12), 2669–2680. https://doi.org/https://doi.org/10.1377/hlthaff.2011.0121
- Horsburgh, M., Merry, A. F., & Seddon, M. (2005). Patient safety in an interprofessional learning environment. Medical Education, 39(5), 512–513. https://doi.org/https://doi.org/10.1111/j.1365-2929.2005.02136.x
- Infante, C. (2006). Bridging the “system’s” gap between interprofessional care and patient safety: Sociological insights. Journal of Interprofessional Care, 20(5), 517–525. https://doi.org/https://doi.org/10.1080/13561820600937598
- Institute of Medicine (US). Health professions education: a bridge to quality. (https://www.ncbi.nlm.nih.gov/books/NBK221528/). Accessed December 14, 2018.
- Jha, A. K., Larizgoitia, I., Audera-Lopez, C., Prasopa-Plaizier, N., Waters, H., & Bates, D. W. The global burden of unsafe medical care: Analytic modelling of observational studies. BMJ Qual Saf. [Online]. 2013 August 29. https://doi.org/https://doi.org/10.1136/bmjqs-2012-001748
- Kearney, A., Adey, T., Bursey, M., Cooze, L., Dillon, C., Barrett, J., et al. (2010). Enhancing patient safety through undergraduate interprofessional health education. Health Care Quarterly, 13[ Special issue], 88–93.
- Kent, F., Nankervis, K., Johnson, C., Hodgkinson, M., Baulch, J., & Haines, T. (2018). ‘More effort and more time.’ Considerations in the establishment of interprofessional education programs in the workplace. Journal of Interprofessional Care, 32(1), 89–94. https://doi.org/https://doi.org/10.1080/13561820.2017.1381076
- Kirkpatrick, D. L. (1967). Evaluation of training. In R. L. Craig & L. R. Bittel (Eds.), Training and development handbook. McGraw-Hill.
- Kyrkjebo, J. M., Brattebo, G., & Smith-Strom, H. (2006). Improving patient safety by using interprofessional simulation training in health professional education. Journal of Interprofessional Care, 20(5), 507–516. https://doi.org/https://doi.org/10.1080/13561820600918200
- Langlois, S. (2016). Developing an appreciation of patient safety: Analysis of interprofessional student experiences with health mentors. Perspectives on Medical Education, 5(2), 88–94. https://doi.org/https://doi.org/10.1007/s40037-016-0258-4
- Lawlis, T. R., Anson, J., & Greenfield, D. (2014). Barriers and enablers that influence sustainable interprofessional education: A literature review. Journal of Interprofessional Care, 28(4), 305–310. https://doi.org/https://doi.org/10.3109/13561820.2014.895977
- Lawton, R., & Armitage, G. (2012). The role of the patient in clinical safety. Health Foundation.
- Leistikow, I. P., Kalkman, C. J., & de Bruijn, H. (2011, January 1). Why patient safety is such a tough nut to crack. BMJ: British Medical Journal [Online], 342.
- Mayer, D., Klamen, D. L., Gunderson, A., & Barach, P. (2009). Designing a patient safety undergraduate medical curriculum: The Telluride Interdisciplinary Roundtable experience. Teaching and Learning in Medicine, 21(1), 52–58. https://doi.org/https://doi.org/10.1080/10401330802574090
- Meinema, J., Buwalda, N., & Visser, M. (2018, August 28). Intervention descriptions in medical education: What can be improved? A systematic review and checklist. Academic Medicine [Online]. https://doi.org/https://doi.org/10.1097/ACM.0000000000002428
- Miller, R., Winterton, T., & Hoffman, W. W. (2014). Building a whole new mind: An interprofessional experience in patient safety and quality improvement education using the IHI open school. South Dakota Medicine : The Journal of the South Dakota State Medical Association, 67(1), 17–22.
- Motycka, C., Egelund, E. F., Gannon, J., Genuardi, F., Gautam, S., Stittsworth, S., Young, A., & Simon, L. (2018). Using interprofessional medication management simulations to impact student attitudes toward teamwork to prevent medication errors. Currents in Pharmacy Teaching and Learning, 10(7), 982–989. https://doi.org/https://doi.org/10.1016/j.cptl.2018.04.010
- Nagelkerk, J., Peterson, T., Pawl, B. L., Teman, S., Anyangu, A. C., Mlynarczyk, S., et al. (2014). Patient safety culture transformation in a children’s hospital: An interprofessional approach. Journal of Interprofessional Care, 28(4), 358–364. https://doi.org/https://doi.org/10.3109/13561820.2014.885935
- Nagraj, S., Harrison, J., Hill, L., Bowker, L., & Lindqvist, S. (2014). Promoting collaboration in emergency medicine. The Clinical Teacher, 54(7), 500–505. https://doi.org/https://doi.org/10.1111/tct.12762
- Nie, Y., Li, L., Duan, Y., Chen, P., Barraclough, B. H., Zhang, M., & Li, J. (2011). Patient safety education for undergraduate medical students: A systematic review. BMC Medical Education, 11(1), 33. https://doi.org/https://doi.org/10.1186/1472-6920-11-33
- Ogrinc, G., Davies, L., Goodman, D., Batalden, P., Davidoff, F., & Stevens, D. (2015). SQUIRE 2.0 (S tandards for QU ality I mprovement R eporting E xcellence): Revised publication guidelines from a detailed consensus process. The Journal of Continuing Education in Nursing, 46(11), 501–507. https://doi.org/https://doi.org/10.3928/00220124-20151020-02
- Okuyama, A., Wagner, C., & Bijnen, B. (2014). Speaking up for patient safety by hospital-based health care professionals: A literature review. BMC Health Services Research, 14, 61–69.
- Packard, K., Iverson, L., Ryan-Haddad, A., Teply, R., Wize, A., & Qi, Y. (2019, October). A synchronous interprofessional patient safety simulation integrating distance health professions students. Journal of Nursing Education, 58(10), 577–582. https://doi.org/https://doi.org/10.3928/01484834-20190923-04
- Paradis, E., & Whitehead, C. R. (2018). Beyond the lamppost: A proposal for a fourth wave of education for collaboration. Academic Medicine, 93(10), 1457–1463. https://doi.org/https://doi.org/10.1097/ACM.0000000000002233
- Peeters, M. J., Sexton, M., Metz, A. E., & Hasbrouck, C. S. (2017). A team-based interprofessional education course for first-year health professions students. Currents in Pharmacy Teaching and Learning, 9(6), 1099–1110. https://doi.org/https://doi.org/10.1016/j.cptl.2017.07.006
- Reeves, S., Clark, E., Lawton, S., Ream, M., & Ross, F. (2017, February). Examining the nature of interprofessional interventions designed to promote patient safety: A narrative review. International Journal for Quality in Health Care, 29(2), 144–150. https://doi.org/https://doi.org/10.1093/intqhc/mzx008
- Reeves, S. A., Denault, D., Huntington, J. T., Ogrinc, G., Southard, D. R., & Vebell, R. (2017). Learning to overcome hierarchical pressures to achieve safer patient care: An interprofessional simulation for nursing, medical, and physician assistant students. Nurse Educator, 42(5), S27–S31. https://doi.org/https://doi.org/10.1097/NNE.0000000000000427
- Reid, A.-M., Fielden, S. A., Holt, J., MacLean, J., & Quinton, N. D. (2018, October). Learning from interprofessional education: A cautionary tale. Nurse Education Today, 69(69), 128–133. https://doi.org/https://doi.org/10.1016/j.nedt.2018.07.004
- Reime, M. H., Johnsgaard, T., Kvam, F. I., Aarflot, M., Breivik, M., Engeberg, J. M., et al. (2016). Simulated settings; powerful arenas for learning patient safety practices and facilitating transference to clinical practice. Nurse Education in Practice, 21, 75–82. https://doi.org/https://doi.org/10.1016/j.nepr.2016.10.003
- Robertson, B., Kaplan, B., Atallah, H., Higgins, M., Lewitt, M. J., & Ander, D. S. (2010). The use of simulation and a modified TeamSTEPPS curriculum for medical and nursing student team training. Simulation in Healthcare: The Journal of the Society for Simulation in Healthcare, 5(6), 332–337. https://doi.org/https://doi.org/10.1097/SIH.0b013e3181f008ad
- Rowland, P., & Kitto, S. (2014). Patient safety and professional discourses: Implications for interprofessionalism. Journal of Interprofessional Care, 28(4), 331–338. https://doi.org/https://doi.org/10.3109/13561820.2014.891574
- Sandars, J., Brown, J., & Walsh, K. (2017). Producing useful evaluations in medical education. Education for Primary Care, 28(3), 137–140. https://doi.org/https://doi.org/10.1080/14739879.2017.1299594
- Sirriyeh, R., Lawton, R., Gardner, P., & Armitage, G. (2012). Reviewing studies with diverse designs: The development and evaluation of a new tool. Journal of Evaluation in Clinical Practice, 18(4), 746–752. https://doi.org/https://doi.org/10.1111/j.1365-2753.2011.01662.x
- Spence, J., Goodwin, B., Enns, C., Vecherya, N., & Dean, H. (2012). Patient safety education: An exploration of student-driven contextual learning. Journal of Nursing Education, 51(8), 466–470. https://doi.org/https://doi.org/10.3928/01484834-20120615-04
- Stevenson, E., Chudgar, S. M., Turner, K., et al. (2015). How we engage graduating professional students in interprofessional patient safety. Nursing Forum, 51(4), 233–237. https://doi.org/https://doi.org/10.1111/nuf.12146
- Stewart, M., Purdy, J., Kennedy, N., & Burns, A. (2010). An interprofessional approach to improving paediatric medication safety. BMC Medical Education, 10(1), 19. https://doi.org/https://doi.org/10.1186/1472-6920-10-19
- Thom, K. A., Heil, E. L., Croft, L. D., Duffy, A., Morgan, D. J., & Johantgen, M. (2016). Advancing interprofessional patient safety education for medical, nursing, and pharmacy learners during clinical rotations. Journal of Interprofessional Care, 30(6), 819–22. https://doi.org/https://doi.org/10.1080/13561820.2016.1215972
- Tricco, A. C., Lillie, E., Zarin, W., et al. (2018). PRISMA extension for scoping reviews (PRISMA-ScR): Checklist and explanation. Annals of Internal Medicine, 169(7), 467–473. https://doi.org/https://doi.org/10.7326/M18-0850
- Vyas, D., McCulloh, R., Dyer, C., Gregory, G., & Higbee, D. (2012). An interprofessional course using human patient simulation to teach patient safety and teamwork skills. American Journal of Pharmaceutical Education, 76(4), 71. https://doi.org/https://doi.org/10.5688/ajpe76471
- Ward, J. K., & Armitage, G. (2012). Can patients report patient safety incidents in a hospital setting? A systematic review. BMJ Quality & Safety, 21(8), 685–699. https://doi.org/https://doi.org/10.1136/bmjqs-2011-000213
- Wilson, A. R., Fabri, P. J., & Wolfson, J. (2012). Human error and patient safety: Interdisciplinary course. Teaching and Learning in Medicine, 24(1), 18–25. https://doi.org/https://doi.org/10.1080/10401334.2012.641482
- Wipfler, K., Hoffmann, J. E., Mitzkat, A., Mahler, C., & Frankenhauser, S. (2019). Patient safety–development, implementation and evaluation of an interprofessional teaching concept. GMS Journal for Medical Education, 36(2), Doc13.
- Wong, B. M., Etchells, E. E., Kuper, A., Levinson, W., & Shojania, K. G. (2010). Teaching quality improvement and patient safety to trainees: A systematic review. Academic Medicine, 85(9), 1425–1439. https://doi.org/https://doi.org/10.1097/ACM.0b013e3181e2d0c6
- Wood, D. F. (2001). Interprofessional education - still more questions than answers? Medical Education, 35(9), 816–817. https://doi.org/https://doi.org/10.1046/j.1365-2923.2001.01038.x
- World Health Organisation. Patient safety. (https://www.who.int/patientsafety/about/en/). Accessed January 10, 2019.